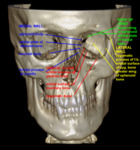
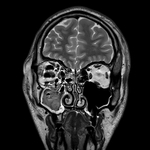
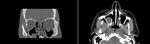
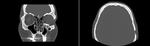
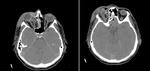
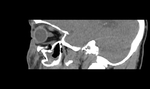
IMAGING
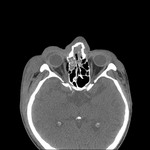
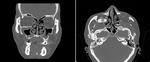
CT imaging in trauma patients remains the gold standard for detecting and evaluate orbital fractures.
Imaging of the entire face is recommended as concomitant facial fractures are commonly seen.
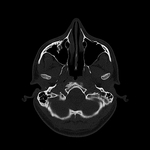
Axial,
coronal,
and sagittal images (slice thickness 1,25 mm),
and three-dimensional (3D) rendering is recommended.
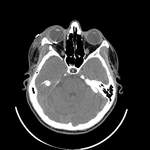
The medial and lateral wall fractures are best visualized in a bone window axial view.
Axial images can be also used to evaluate the fractures involving the zygomaticomaxillary complex.
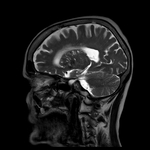
The sagittal view may be helpful in assessing orbital floor and roof fractures.
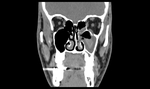
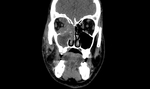
Coronal images are particularly useful to identify orbital roof,
floor,
or extraocular muscle involvement,
as well as the degree of enophthalmos.
Both coronal and sagittal views can be used to assess the orbital soft tissue and evaluate for fat herniation or extraocular muscle entrapment.
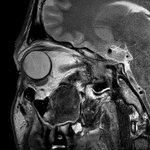
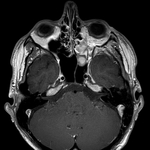
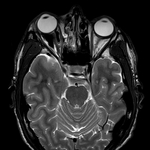
MR imaging may be used to evaluate soft tissue injury.
MR imaging is helpful in assessing cranial nerve deficits,
although it is limited in its ability to assess cortical bone.
(Fig.
1)
ORBITAL FLOOR FRACTURES
The orbital blow-out fracture typically occurs when an object larger than the bony orbit impacts the orbit with sufficient force to increase intraorbital pressure and fracture the orbital floor.
The free fragment sign on CT demonstrates an isolated fragment within the maxillary sinus with depressed or displaced orbital floor fractures.
With an acute injury,
hemorrhage into the maxillary sinus should be present.
If the sinuses are clear,
the injury is likely remote.
The most common indication for emergent repair of an orbital floor fracture is extraocular muscle entrapment.
The oculocardiac reflex may be elicited in an orbital fracture due to entrapment of the extraocular muscles and can result in bradycardia,
vomiting,
syncope.
The oculocardiac reflex more commonly occurs with trapdoor type fractures where a segment of bone is displaced,
and and then bounce back,
entrapping the inferior rectus muscle,
so entrapment of the inferior rectus.
This is more common in pediatric patients presumably due to a more elastic orbital bone.
The coronal CT scans can provide information about the shape and position of the inferior rectus muscle.
If the rectus remains flattened and in the correct position,
then the periorbital fat have been only slight entrapment.
If the inferior rectus is round and inferiorly displaced,
then muscle has prolapsed into the orbital floor defect.
(Fig.
2)
Orbital emphysema is another complication,
in which floor and medial wall fractures allow the release of adjacent paranasal sinus air into the orbit.
Although this is usually a self-limited condition,
it can cause mass effect on the adjacent soft tissues and be a rare cause of decreased vision due to either occlusion of the central retinal artery or optic neuropathy.
From the infraorbital foramen exits the infraorbital nerve,
providing sensory innervations to the middle floor of the face.
The infraorbital nerve dysfunction occurs and is often the only complaint following pure orbital floor fracture.
This sensory disturbance traditionally has not been an indication for repair.
Nonemergent operative indications for the orbital floor include fractures that involve greater than 50% of the floor or fractures greater than 1 cm2,
and enophthalmos > 2 mm.
The surgery for nonemergent injuries is performed around 7 to 14 days after trauma before soft tissue scarring develops,
but after resolution of posttraumatic edema.
MEDIAL WALL FRACTURES
Medial orbital wall fractures often present with orbital emphysema due to fracture and involvement of the adjacent ethmoid air cells,
which can leads to orbital compartment syndrome by the air trapping within the orbit and cause vascular compromise to the intraorbital contents.
The medial wall and rim provide a site of insertion for the medial canthal tendon,
which provides medial support to the globe and fractures in this location may lead to telecanthus.
Although the tendon is not visible at multidetector CT,
identification of a fracture through the inferomedial orbital rim at the level of lacrimal fossa implies a disruption of the medial canthal tendon.
(Fig.
3) The nasolacrimal sac damage may lead to tear outflow obstruction.
The nasofrontal ducts disruption,
which drains the frontal sinus predisposes the patient to future mucocele formation unless the sinus is surgically obliterated,
so the report should include a description of the degree of comminution of the ethmoid sinus in the region of the nasofrontal ducts.
The anterior and posterior ethmoidal arteries traverse the medial wall at its junction with the orbital roof,
carrying blood from the ophthalmic artery to the nasal cavity.
So injury to these vessels can cause significant intraorbital hemorrhage and even orbital compartment syndrome.
Fractures of the medial wall must accordingly be evaluated for potential effect on these associated structures.
Enophthalmos from isolated medial wall fractures occurs less frequently than it does with isolated orbital floor fractures,
as the force of gravity does usually displace orbital contents downward to the maxillary sinus.
Both blow-in and blow-out patterns can result in the medial rectus muscle entrapment.
Any radiologic findings of potential damage to the globe or optic nerves,
such as a retrobulbar hematoma or an impinging bone fragment,
should be communicated to the surgeon since they require immediate surgical treatment if associated with decreasing vision.
Operative indications for medial wall fractures include medial rectus muscle entrapment,
enophthalmos > 2 mm,
persistent diplopia in a primary gaze that persists for 2–4 weeks after injury,
and large defects (more than 50% of wall or 1cm2).
LATERAL WALL FRACTURES
The lateral orbital wall is the site of insertion for the lateral canthal tendon onto Whitnall’s tubercle.
Lateral orbital fractures that require surgical intervention are commonly linked to fractures of the zygomatic bone,
also known as zygomaticomaxillary complex or tripod fractures.
Nondisplaced orbitozygomatic fractures are often managed conservatively.
Displaced fractures,
generally require surgical stabilization to maintain facial width and prominence of the cheek.
During surgical repair of the lateral wall with zygomatic arch fracture,
the temporal and zygomatic branches of the seventh nerve and the zygomaticotemporal and zygomaticofacial branches of the fifth nerve must be avoided in order to prevent complications of paresis and paresthesias.
(Fig.
4)
ORBITAL ROOF FRACTURES
Orbital roof injuries appear more commonly in the pediatric population,
prior to the pneumatization of the pediatric craniofacial skeleton.
The blow-in fracture usually results from a high energy impact to the frontal bone and consists of fracture and depression of the orbital roof into the orbit.
Blow-in fractures are often associated with intracranial injury and loss of orbital volume leading to exophthalmos.
The blow-up fracture involves cranial displacement of the orbital roof,
which increases orbital volume and is strongly indicative of intracranial injury.
The fracture that extends to posterior frontal sinus wall creates a communication between the frontal sinus and the anterior cranial fossa,
a condition that increases the likelihood of complications such as CSF rhinorrhea,
brain herniation,
and intracranial infection.
If the fracture propagates to the orbital apex,
the optic nerve can be injured by direct fracture fragment penetration,
hemorrhage into the sheath or ischemia resulting from increased intraorbital pressure.
Suspicion of an optic nerve impingement is an indication to emergent surgery.
Injury to the nasofrontal outflow tract is indicated by anatomic outflow tract obstruction.
Coronal images are helpful for evaluating the base of the frontal sinus at the site of the ostium of the duct.
Nasofrontal duct injury or posterior wall injury with a dural tear usually requires removal of the sinus mucosa and obliteration of the cavity to prevent mucocele formation.
In surgical procedures where the frontal sinus is preserved,
serial CT scans in the postoperative period are often performed to assess for adequate drainage of the sinus.
Displaced fractures,
blow-out or blow-in fracture,
often undergo open reduction and stabilization,
particularly if they cause diplopia,
proptosis,
or extraocular muscle entrapment.
GLOBE INJURY
Injury to the globe,
retrobulbar hematoma,
and optic nerve injury are considered more emergent than entrapment or enophthalmos.
Blunt and penetrating trauma to the globe can disrupt the integrity of the sclera and result in globe rupture.
CT is the initial imaging modality when ocular trauma with an open-globe injury is suspected.
MR imaging should be considered when a clinically suspected open-globe injury is not identified at CT.
Evident imaging findings of open-globe injuries include alteration of the globe contour or volume and evidence of scleral discontinuity.
Indirect imaging findings of globe injuries are decreased the volume of the anterior chamber,
and intraocular foreign body or air.
Vitreous hemorrhage is readily seen at CT as hyperattenuating fluid in the posterior segment.
Hyphema is defined as a collection of blood in the anterior chamber of the globe,
at unenhanced CT an area of hyperattenuation in the anterior chamber is seen.
Blunt force may cause the tear of the zonular fibers on the lens.
This mechanism can result in partial or complete dislocation of the lens.
Partial tear of the zonular fibers leads to lens subluxation may be seen on CT as an obliquely oriented lens.
A tear involving all of the zonular fibers around the lens causes complete dislocation of the lens,
which usually dislocates into the posterior segment of the globe.
If one lens appears hypodense relative to the contralateral lens,
acute lens edema should be suspected because this may lead to a traumatic cataract.
The difference in attenuation is usually approximately 30 Hounsfield units.
The wall of the posterior segment of the globe is composed of three layers: the sclera,
the retina,
and the choroid.
Trauma to the globe may disrupt the attachments between these layers and result in detachments.
Retinal detachments may have a characteristic V-shaped appearance at imaging,
with the apex at the level of the optic disc,
where it has a strong attachment.
The choroidal detachments have a lentiform shape at imaging and spare the posterior portion of the globe.
SURGICAL MANAGEMENT
Subciliary,
subtarsal,
and transconjunctival incisions are the most commonly performed for correction of the orbital floor fractures.
Medial wall fractures are difficult to repair,
though there are many approaches like the transcutaneous (Lynch incision),
transconjunctival inferior fornix,
transcaruncular,
and endoscopic trans-ethmoidal.
The endoscopic approach can be technically challenging,
but it avoids eyelid complications and improve visualization of the orbital walls and can provide a valuable assessment of soft tissue reduction and implant positioning.
Early postoperative CT imaging could be performed to assess implant position.Intraoperative imaging has the advantage of showing the actual implant as it is positioned in the orbit,
if a radioopaque implant,
such as titanium,
is used.
Autogenous material
Bone from the calvarium,
iliac crest,
nasal,
maxillary,
and mandibular bone have been used as donor sites,
with the first two being the most commonly used.
Bone has good strength and can be fixed to the adjacent bone,
but its lack of flexibility makes difficulty in forming it into complex shapes.
Bone graft have similar attenuation to the native bone: intact grafts have a well-defined cortex and lower density central medullary canal,
and morcellized graft manifests as masslike opacity.
Septal and auricular cartilage has been used for reconstruction of orbital defects,
but although they are completely biocompatible,
they provide limited structural support and are prone to resorption.
Alloplastic materials
Titanium is highly biocompatible,
easily adjusted to architecturally fit simple and complex orbital defects,
provides strong support and it can be easily fixed to the adjacent bone.
It has well osseointegration and readily available,
although at a high cost.
Titanium in CT images is hyperattenuating (denser than native bone) and associated with a small amount of beam-hardening artifact.
Polyethylene material exhibits high biocompatibility,
is easily trimmed into any desired shape,
can be screw-fixated to the bone,
and has good strength with good long-term stability.
Using preoperative CT,
patient-specific implant (PSI) can be specifically designed to mirror the non-affected orbit.
Porous polyethylene has a similar density to fat in the early stage after implantation and appears as soft tissue after few months to a year because of fibrovascular ingrowth.
Nylon has soft-tissue density with a linear structure.
Silicone is hyperdense relative to soft tissue but less dense than bone.
(Fig.
5,6,7)
POSTOPERATIVE IMAGING
CT is the dominant modality for postoperative imaging of facial trauma.
MRI is indicated,
when cranial nerve deficits are present,
to detect nerve compression due to hematoma,
nerve transection,
or axonal injury.
(Fig.
8,9)
The three most common unfavorable outcomes of orbital fracture repair are diplopia,
persistent enophthalmos,
and infraorbital nerve hypoesthesia.
Both diplopia and enophthalmos tend to be related to inaccurate reduction and reconstruction of the orbital walls.
The implant uses in orbital floor reconstruction should be anchored posteriorly to the stable bone,
otherwise,
it is a high likelihood of implant collapse and reherniation of orbital contents into the maxillary sinus.
Placement an implant too far on the posterior ledge can lead to displacement of the implant superiorly into the optic nerve.
When an implant with lower tensile strength,
such as silicone,
is used to repair a large defect,
it can lead to the folding of the central portion of the implant.
(Fig.
10,
11)
Displaced osseous fragments after facial trauma should be documented on preoperative imaging.
Osseous fragments present in the maxillary sinus may be left in place or extracted.
However,
abandoned osseous fragments can cause an episode of sinusitis due to obstruction of the infundibula.
One of the most frequent complications in the reconstruction of medial wall fractures is a placement of the implant without securing it onto a stable ledge of bone superiorly,
resulting in herniation into the ethmoidal sinus.
Visualization of the optic nerve or extraocular muscle impingement requires urgent revision.
The typical appearance of orbital hemorrhage on CT is a hyperattenuating collection,
although a chronic collection of blood can have the same density as simple fluid.
Retrobulbar hemorrhage requires immediate intervention and may occur after surgery as a result of injury to the zygomaticotemporal,
posterior ethmoidal arteries or the vessels accompanying the infraorbital nerve.
CT is used if there is clinical suspicion for infection,
and identification of an orbital abscess prompts urgent surgical intervention for drainage.
Orbital emphysema after orbital fracture repair due to the incomplete restoration of the defect is an important complication because it can lead to displacement of the repaired fracture.
(Fig.
12,13,14,15,16)