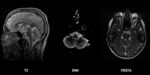
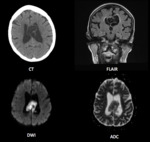
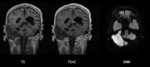
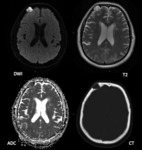
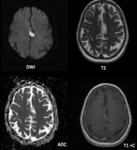
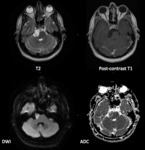
Epidermoid cysts,
also known as primary cholesteatomas or ectodermal/epithelial inclusion cysts,
are usually congenital,
arising during neural tube closure in the 3rd to 5th week of foetal life or from focal expansion of a dermal sinus in the spine.
They can also be acquired secondary to trauma,
which is rare in intracranial epidermoids but can account for up to 40% of spinal epidermoids,
which are generally acquired after lumbar puncture or surgery.
Epidermoids account for about 0.2-1.8% of primary intracranial tumours and 1-2% of spinal cord masses (up to 10% of spinal cord lesions in children).
They are the commonest congenital intracranial tumour.
Approximately 50% of epidermoid cysts occur at the cerebellopontine angle (CPA) and they are one of the commonest tumours in this region.
In the spine,
acquired epidermoid cysts are almost always at the cauda equina.
They are predominantly intradural (approximately 90%),
most commonly arising in the basal cisterns at the CPA and parasellar region.
Up to 10% of epidermoids are intradiploic,
given their ectodermal origin.
In the spine,
about 60% are extramedullary with the remainder being intramedullary.
They occur sporadically with no known mode of inheritance and they may be associated with a dermal sinus tract,
vertebral and rarely spinal anomalies.
There is equal gender predilection for intracranial epidermoids,
although the CT dense lesions tend to favour women.
Spinal lesions are reportedly more common in males.
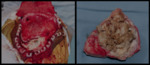
On surgery and pathology,
the tumour is described as having a lobulated,
irregular outline with a pearly external appearance and internal waxy,
creamy or flaky material.
On microscopy,
the cyst wall is composed of a fibrous capsule lined by cuboidal squamous epithelium.
The contents include cholesterol,
keratin and possible calcifications,
but no dermal appendages – the absence of dermal appendages differentiates it from dermoid cysts,
which contain dermal elements.
Lamellations may form as the cyst enlarges.
Clinical presentation depends on tumour location and effect on surrounding structures.
Common presentations include: headache and V,
VII & VIII cranial neuropathies,
cerebellar signs and possibly seizures.
Less common presentations include pituitary dysfunction and aseptic meningitis,
the latter occurring if the cyst ruptures.
Spinal lesions are asymptomatic or present with neural or cord compression.
Treatment is in the form of surgical resection with its associated morbidity depending on the site.
Recurrence is common following excision and the rare but reported malignant change in the form of squamous cell carcinoma often occurs in recurrent tumours.
Therefore,
close follow up is frequently undertaken,
although there are currently no guidelines on this issue.