Classically,
epidermoid cysts have the same density as CSF and may displace or encase surrounding structures.
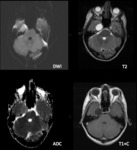
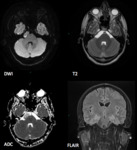
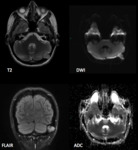
The investigation of choice is magnetic resonance imaging (MRI) with fluid attenuation inversion recovery (FLAIR) and diffusion weighted imaging (DWI),
although a large number of patients will have had a CT as a first line neurological investigation,
therefore it is important that the radiologist suspects this diagnosis and recommends further confirmatory imaging.
Unenhanced CT will typically show a well-circumscribed,
rounded or lobulated CSF-density lesion,
which is hypodense to the brain parenchyma.
It can have an atypically dense appearance,
occurring in about 3% of cases,
which can be mistaken for a meningioma.
Postulated causes for increased density include haemorrhage,
proteinaceous fluid or changes secondary to cyst degeneration.
Calcification can be a feature in up to 25% of epidermoid cysts.
Bone window may show bony erosion with sclerosis in the intradiploic type.
In spinal epidermoids,
widening of the spinal canal and flattening of the pedicles and laminae at the level of the lesion can occur.
Post-contrast CT commonly shows no enhancement,
however rim-enhancement has been reported in the setting of infection or more commonly if malignant degeneration has occured.
On conventional angiography,
the lesion may show as an avascular area with pressure effects on the adjacent vasculature.
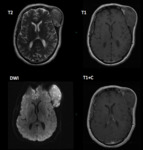
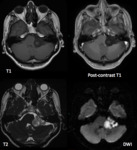
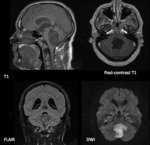
On MRI,
the lesion commonly replicates CSF signal on T2-weighted imaging with infrequent hyperintensity to CSF in atypical tumours.
Even rarer would be hypointensity to CSF,
occurring due to calcification,
iron deposition or high viscosity secretions.
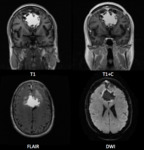
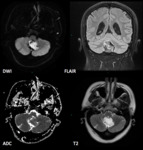
On FLAIR images,
epidermoid cysts rarely lose all their signal.
On T1-weighted imaging,
an epidermoid cyst is commonly mildly hyperintense to CSF,
with atypical appearances including white and black epidermoids.
In white epidermoids,
the lesion is hyperintense to the brain parenchyma and with high density on CT usually due to high lipid content with triglycerides but no cholesterol.
Black epidermoids are hypointense to CSF on both T1 and T2 weighted imaging due to the lack of fat and the presence of solid crystals,
such as cholesterol,
as well as epithelial debris and keratin.
Haemorrhage within the lesion can also account for the variable imaging features,
although,
given the avascular nature of epidermoid,
haemorrhage is rare with only few reported cases.
If there is haemorrhage within an epidermoid cyst,
lesions are often dense on CT and hyperintense on both T1 and T2,
although this can vary with ageing of the blood products.
On post-contrast T1 imaging,
as on post-contrast CT,
rim enhancement may be seen,
although this is thought to indicate malignant degeneration,
with the majority of cysts showing no enhancement.
Epidermoid cysts show restriction of diffusion,
with diffusion-weighted imaging typically showing hyperintensity,
with isointensity to the brain on the ADC map.
This feature differentiates epidermoid cysts from arachnoid cysts,
which do not restrict diffusion.
MR Spectroscopy shows no NAA,
choline or lipid with a high lactate peak (at 1.3 ppm),
although atypical features with low creatine,
choline,
NAA and inverted peak of lactate have been reported.
Differential Diagnosis:
The differential diagnosis of epidermoid cysts varies according to their location and morphology.
Differential diagnoses include meningiomas,
arachnoid cysts,
infected cysts/abscesses and cystic tumours including Schwannomas,
craniopharyngiomas and gliomas.
Meningiomas can be a differential for epidermoid cysts which are dense on CT,
although sclerosis of the underlying bone and intense enhancement post-contrast would be in keeping a meningioma.
Arachnoid cysts are smooth,
CSF density lesions,
which can displace but do not compress or encase adjacent structures.
They also show signal loss on FLAIR and no restriction of diffusion,
i.e.
mimicking CSF density on DWI and ADC.
Dermoid cysts are also in the differential,
but they are usually midline lesions of fat density and signal and contain dermal elements on histopathology (unlike epidermoid cysts which lack dermal elements).
Infected cysts/abscesses and other cystic neoplasms can also be confused for epidermoid cysts,
but these are less likely to be of CSF density and often show adjacent signal change and post-contrast enhancement.
If the lesion is in the CPA,
a cystic Schwannoma is in the differential,
although a purely cystic schwannoma is rare and Schwannomas avidly enhance with extension into the internal auditory meatus or growth along nerves.
If the lesion is perisellar with focal calcification,
a craniopharyngioma may be suspected,
however the majority of these tumours would enhance.
In the spine,
neurenteric cysts can give a similar appearance,
although they are often intradural and can be associated with vertebral anomalies,
with pathology being confirmatory.