Patients:
From January 2006 to December 2010,
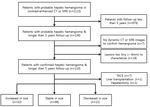
a total of 1115 consecutive patients were recognized to have suggestive features of hepatic hemangiomas on contrast-enhanced CT or MRI at our institution.
Among those patients,
only 101 patients (55 males and 46 females,
mean age 51.9 years) were finally included in the study according to the following criteria (Figure 1); 1) having one or more follow-up CT or MRI with an interval of >5 years,
2) at least one session of dynamic CT or MRI available for the diagnosis,
3) the lesion should be large enough (≥ 6mm) at one or more imagings in follow-up period for clear characterization,
4) patients who underwent liver transplantation,
partial hepatectomy or transarterial chemoembolization were excluded.
Imaging Protocols:
CT examinations were performed with one of two scanners; a 16-slice or a 64-slice multidetector CT scanner (Somatom Sensation 16 or Somatom Sensation 64; Siemens Medical Solutions,
Erlangen,
Germany).
For contrast enhancement,
120–150 mL of nonionic iodinated contrast medium was administered intravenously with an automatic injector at a rate of 2.5–3 mL/s.
For dynamic CT,
the average start times for the arterial and portal venous phases were 34 s (30–38 s) and 70 s,
respectively,
after the initiation of contrast medium injection.
Delayed phase scan was acquired at 3 min after the start of the contrast material injection.
MRI exams were performed using 1.5-T systems (Magnetom Vision or Avanto; Siemens,
Erlangen,
Germany).
The MRI protocol consisted of fat-suppressed T2-weighted images,
opposed- and in-phase images and contrast-enhanced images.
The dynamic series consisted of one precontrast scan followed by three sequential postcontrast series (early arterial,
late arterial,
and portal phase) with 34-s intervals.
The postcontrast series were performed after a bolus injection of gadoxetic acid disodium (0.1 mL/kg) (Primovist; Bayer Healthcare,
Berlin,
Germany).
Delayed phase and hepatobiliary phase images were acquired at 5 and 20 min,
respectively,
after the contrast agent injection.
As our institution is a tertiary referral hospital,
there were numerous imaging data from other institutions,
and those images were also used for data analysis if the digital image was available for lesion comparison on PACS.
Data Analysis:
Two radiologists (one with 10 years’ experience with abdominal imaging and the other a second-year radiology resident) reviewed the images independently and recorded the size of each hepatic hemangioma.
The selection of imaging slices and the contrast-enhanced phase depended on the largest lesion diameter and the most conspicuous lesion-to-liver contrast in each patient.
The lesion size was defined as the mean value of the longest dimensions measured on the axial images by the two radiologists.
Size measurement was performed in the initial and final follow-up imaging studies for each patient.
The change in size was categorized into three groups: “enlarged,” with a final size >120% of the initial size; “not-changed,” with a final size 80–120% of the initial size; “shrunken,” with a final size <80% of the initial size.
Furthermore,
imaging data on the closest to the median date between the initial and final examinations were also reviewed to reveal possible fluctuations in size.
The study coordinator (20 years’ experience of abdominal imaging) recorded the background hepatic condition of each case to determine the underlying liver problem such as liver cirrhosis and fatty liver.
The presence of liver cirrhosis was determined according to relevant hepatic contour changes and portal hypertensive stigmata in the imaging studies,
in addition to the patients’ medical records.
Hepatic steatosis was defined as the liver showing lower attenuation than that of the spleen on nonenhanced CT based on rather specific criteria (liver – spleen,
<1 Hounsfield unit) [10].
The medical records of all cases were reviewed for medication history,
including steroids,
female hormones,
and chemotherapy for controlling malignancy.
Statistical Analysis:
To determine the relationship between the patients’ ages and the size change of the hemangiomas,
the correlation coefficient between the patients’ ages and the diameter change ratio (the final diameter divided by the initial diameter) of the lesion was calculated.
Continuous variables were analyzed using one-way analysis of variance combined with Student-Newman-Keuls test for all pairwise comparisons among the three groups of size change.
The categorical variables were analyzed with a chi-square test.
Values of p<0.05 were considered statistically significant.
Logistic regression test was additionally conducted for statistically significant variables.
All statistical analyses were performed with SPSS Statistics version 23 (IBM Corp.,
Armonk,
NY,
USA).