The main findings seen across all imaging modalities were clustered in 3 groups,
as follows:
A).- NECK SWELLING / PALPABLE MASS:
1.- Cervical lymphadenopathy:
Enlarged cervical nodes are the most common neck masses in children.
Enlargement of cervical lymph nodes may be due to infectious,
inflammatory,
neoplastic,
or idiopathic causes.
Normal lymph nodes are classified according to diameter,
which is generally less than 10 mm in the long axis.
Exceptions are level IB and IIA nodes,
which may be as large as 15 mm in diameter,
and retropharyngeal nodes,
which should not exceed 8 mm.
On US images,
normal nodes appear hypoechoic in comparison with muscle.
They have an ovoid shape and an echogenic fatty hilum.
Imaging findings of cervical lymphadenopathy are often nonspecific,
although the size,
enhancement,
and distribution of nodes,
and associated head and neck findings,
may be suggestive of an underlying cause.
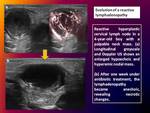
A).- Patients with BENIGN REACTIVE LYMPH NODES typically
present with signs of local or systemic infection,
with painful,
mobile
nodes at physical examination.
At imaging,
these nodes are normal to slightly enlarged in size,
and
they may enhance or demonstrate increased vascularity at US.
Bacterial infections tend to produce greater enlargement of nodes with inflammatory change in surrounding tissues,
and they may
progress to suppurative adenopathy Fig. 1 .
Viral infections produce
diffuse lymph node involvement,
with little surrounding
inflammation.
B).- NEOPLASTIC INVOLVEMENT:
Firm,
nonmobile,
painless cervical lymph nodes.
Neoplastic nodes
demonstrate variable imaging characteristics and may be secondary
to Castleman disease,
lymphoma (both Hodgkin and non-Hodgkin),
leukemia,
or metastases.
Ill-defined borders and loss of fat planes between nodes and
adjacent structures (muscle,
vasculature,
bone) are suggestive of
extracapsular spread of malignancy.
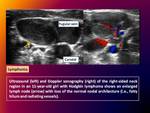
At US,
the affected nodes also show a loss of echogenicity in the
hilum,
peripheral or mixed hypervascularity on Doppler images,
and
possibly,
intranodal cystic change Fig. 2 .
Although metastatic disease is rare in children and young adults,
it
is critical to consider the possibility of metastasis from papillary
thyroid cancer in a young female,
squamous cell carcinoma in young adults,
and neuroblastoma and rhabdomyosarcoma in
children.
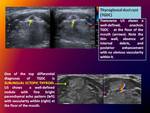
2.- Thyroglossal duct cyst:
The thyroglossal duct is lined by secretory epithelium and connects the foramen cecum at the base of the tongue to the thyroid.
The duct typically involutes between the 8th and 10th gestational weeks; however,
if involution fails,
a cyst may arise anywhere along the surface of the functioning secretory epithelium.
Patients present with a neck mass that moves during swallowing or extension of the tongue or with symptoms of infection,
including swelling,
pain,
erythema,
and fever.
US demonstrates a circumscribed lesion in the characteristic location,
with intralesional echogenicity depending on the proteinaceous content of the cyst (the higher the protein content,
the more echogenic the lesion).
The presence of a thick external wall or internal septa is suggestive of superinfection.
Enhancing material within the cyst may represent ectopic thyroid tissue.
Fig. 3
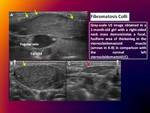
3.- Fibromatosis colli:
Also called pseudotumor of the sternocleidomastoid muscle,
is a benign self-limiting condition that may occur in infants within the first 2–4 weeks of life.
It is thought to result from fibrocollagenous infiltration of the sternocleidomastoid muscle and is often associated with breech or forceps deliveries.
Patients typically present with a unilateral firm and nontender mass within the mid to lower sternocleidomastoid muscle.
Torticollis is seen in an estimated 20% of cases.
US is the most appropriate modality for the initial imaging assessment.
Characteristic US findings include focal or diffuse enlargement of the sternocleidomastoid muscle,
which has variable echogenicity.
Fig. 4
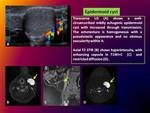
4.- Epidermoid cyst:
Slow-growing subdermal cyst that contains keratin and is lined by stratified squamous epithelium.
Ultrasound appearances depend on maturation of cyst and amount and compactness of keratin.
Well-circumscribed ovoid (80%) is the most common configuration,
with increased acoustic transmission (96%),
mostly avascular and mildly hyperechoic.
It contains thin hypoechoic cyst wall (unless superinfection).
Fig. 5
MR findings: Isointense to slightly hyperintense relative to muscle in T1WI,
Hyperintense signal with T2WI,
T2-hypointense rim due to stratified squamous epithelial wall and absent to low level of central enhancement with enhancing capsule in T1WI C+.
It may show restricted diffusion.
The main differential consideration is branchial cleft cyst.
Fig. 5
B).- FEVER AND DYSPHAGIA:
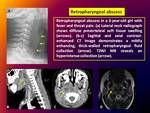
1.- Retropharyngeal abscess:
Retropharyngeal abscesses result from spread of infection from retropharyngeal lymph nodes,
which drain the middle ear,
sinuses,
and upper respiratory tract.
Such abscesses are more common in children younger than 6 years,
as the retropharyngeal nodes atrophy with age.
Because of the possibility of life-threatening complications due to airway compromise and spread of infection to the mediastinum,
the recognition of these abscesses is important.
The retropharyngeal space is a potential space between the prevertebral and visceral spaces,
between the middle and deep layers of the deep cervical fascia.
The space is not well depicted at imaging unless a pathologic process is present.
The clinical manifestations are variable: fever,
neck pain,
sore throat,
and cough are common.
Possible complications include mediastinitis,
necrotizing cervical infection,
internal jugular vein thrombosis,
carotid artery involvement,
and aspiration of pus with pneumonia or empyema.
Lateral neck radiographs demonstrate prevertebral or retropharyngeal soft tissue thickening.
Fig. 6
On CT and MR images,
characteristic findings include fluid within the retropharyngeal space,
with peripheral rimlike enhancement after contrast material administration.
Fig. 6
2.- Tonsillitis:
Peritonsillar infections are commonly encountered in pediatric clinical practice.
The infection usually begins as a superficial infection or tonsillitis and progresses through peritonsillar cellulitis to the end point of peritonsillar abscess,
which can be potentially life-threatening.
Due to the similar clinical presentation,
differentiation of peritonsillar abscess from peritonsillar cellulitis or uncomplicated tonsillitis can be very challenging based on clinical exam alone.
The role of imaging in the diagnosis of tonsillar disease is to help differentiate tonsillitis from peritonsillar abscess.
Imaging is particularly useful in the presence of atypical clinical manifestations,
trismus that limits physical examination,
failure of resolution despite adequate antibiotic treatment,
or clinical suspicion of the extension of tonsillar disease into the deep spaces of the neck.
US findings in uncomplicated tonsillitis manifests as tonsillar hypertrophy without fluid collection.
The affected tonsil shows increase in size greater than 2 cm in at least one dimension,
with preserved homogeneous echotexture.
Fig. 7
C).- BREATHING DIFFICULTIES:
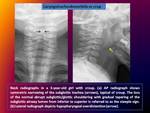
1.- Laryngotracheobronchitis:
Also called crup,
most commonly occurs between the ages of 6 months and 3 years.
Various viral causes,
including parainfluenza,
are most commonly implicated.
The disease onset is signaled by prodromal symptoms of viral infection,
which are followed by fever,
inspiratory stridor,
hoarseness,
and a classic “barking” cough.
The condition typically occurs during the fall and winter months.
In pediatric patients in whom croup is suspected,
imaging is performed to determine whether another cause of inspiratory stridor is present that may require emergent intervention (epiglottitis and foreign body ingestion).
Frontal radiographs demonstrate symmetric straightening of the normally convex appearance of the “shoulders” of the subglottic airway,
a finding also referred to as the “steeple sign.”
Lateral radiographs show narrowing of the subglottic airway with distention of the hypopharynx.
Fig. 8
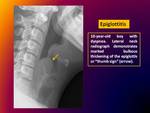
2.- Epiglottitis:
Acute epiglottitis is one of the most serious emergent conditions of the pediatric head and neck because of its association with airway compromise.
Fever,
sore throat,
drooling,
posturing with neck extension,
and respiratory distress are common clinical symptoms of the condition.
Epiglottitis is normally diagnosed on the basis of clinical findings,
and imaging should be performed only if necessary and if it will not interfere with bronchoscopy or maintenance of airway patency.
If the patient’s condition permits,
lateral neck radiography is the preferred modality.
Thickening of the epiglottis (the “thumb sign”) and aryepiglottic folds is a characteristic finding.
Fig. 9
Endoscopy is performed emergently to confirm the diagnosis.
Treatment measures include securing an airway and initiating intravenous antibiotics.