Clinical Features
The clinical presentation of convexal SAH varies depending on the location of haemorrhage as well as the the underlying aetiology.
The onset of symptoms can be sudden or gradual and patients may present with one or multiple neurological features which can be transient in nature.
Common presenting symptoms include:
- Headache: Thunderclap or gradual onset
- Altered mental status
- Sensorimotor symptoms: Weakness,
numbness,
dysarthria or aphasia
- Seizure: Partial or generalised
Clinical features vary depending on patient age.
Cerebral amyloid angiopathy (CAA) is the most common cause of non-traumatic spontaneous convexal SAH in the older population and reversible vasoconstriction syndrome (RCVS) is the most common cause in the younger population.
Aetiology
Trauma:
The focus of recent literature has been on the variety non-traumatic causes of cerebral convexity SAH.
However,
this condition is commonly seen secondary to trauma with haemorrhage localised to cerebral convexities on initial CT brain.
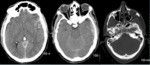
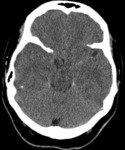
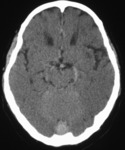
Radiological features: CT soft tissue window (Fig. 1) shows focal and peripheral SAH in the left lateral frontotemporal sulci but also haemorrhagic contusions,
subdural haemorrhage and calvarial fractures – all post trauma.
Non-Traumatic Causes:
While peripheral convexity SAH most commonly occurs secondary to trauma,
there are a wide range of non-traumatic aetiologies:
- Cerebral amyloid angiopathy
- Vasoconstriction syndromes:
- Reversible cerebral vasoconstriction syndrome (RCVS)
- Posterior reversible encephalopathy syndrome (PRES)
- Postpartum cerebral angiopathy
- Vasculitis
- Venous sinus thrombosis
- Vascular malformations:
- Arteriovenous malformations (AVM)
- Arteriovenous fistula (AVF)
- Systemic causes
- Coagulopathy
- Septic emboli
1.
Cerebral amyloid angiopathy
Cerebral amyloid angiopathy (CAA) is a cerebrovascular disorder caused by deposits of amyloid beta peptide in cerebral blood vessels resulting in vascular fragility and increased risk of intracerebral haemorrhage.
Sporadic CAA occurs in the elderly population and is associated with Alzheimer’s disease.
Clinical features: Patients with convexal SAH secondary to CAA typically present with transient focal neurological spells (TFNS) consisting of recurrent unilateral migrating paraesthesia which may be associated with aphasia,
dysphagia or visual symptoms.
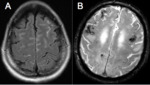
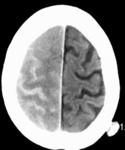
Radiological features: CT brain features include lobar haematomas of different ages and peripheral SAH.
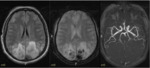
MRI brain shows microhaemorrhages and superficial siderosis (Fig. 2).
2.
Vasoconstriction Syndromes
A. Reversible cerebral vasoconstriction syndrome (RCVS)
Clinical features: Patients classically present with recurrent thunderclap headache that may be associated with photophobia,
nausea or vomiting.
The exact pathophysiology is unknown but symptoms are caused by diffuse segmental constriction of cerebral arteries that typically resolves within three months of onset.
RCVS may be precipitated by vasoactive drugs such as SSRIs,
cyclophosphamide and cocaine and or in a post-partum state,
eclampsia or pre-eclampsia.
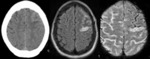
Radiological features: CT brain shows focal and peripheral SAH.
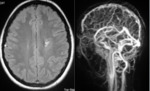
MRI brain is more sensitive and shows FLAIR hyperintensity and marked susceptibility in left frontal sulci near the vertex (Fig. 3).
Diffuse reversible cerebral vasoconstriction is seen on cerebral angiogram studies.
CTA,
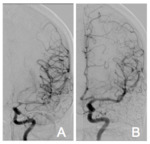
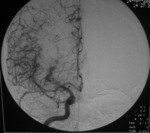
MRA or DSA demonstrates multifocal narrowing in the circle of Willis with post-stenotic segments giving a classical beaded appearance (Fig. 4: A) .
Spontaneous resolution usually occurs and confirmation of diagnosis is made by resolution of angiographic findings on follow-up imaging,
usually within 3 months (Fig. 4: B).
B.
Posterior reversible encephalopathy syndrome (PRES)
Posterior reversible encephalopathy syndrome most commonly occurs secondary to severe hypertension with failed autoregulation and hyperperfusion of the posterior circulation.
Risk factors are chronic kidney disease or eclampsia.
Hyperperfusion results in endothelial injury with vasoconstriction and vasogenic oedema,
most commonly in the parieto-occipital regions.
The syndrome may extend beyond the posterior circulation and while most cases result in complete recovery,
some patients can develop persistent neurological injury.
Clinical features: Patients present with headache,
confusion,
visual disturbance or seizures.
Treatment involves treating the precipitant with aggressive blood pressure management.
Radiological features: MRI brain demonstrates vasogenic oedema most commonly within the occipital and parietal regions.
The three main imaging patterns are: superior frontal sulcus,
parieto-occipital dominance and holohemispheric watershed zones.
Both petechial intraaxial and peripheral sulcal subarachnoid haemorrhage can occur with PRES (Fig. 5).
3.
Other Causes
A.
Vasculitis
Clinical features: Patients present with non-specific neurological symptoms caused by inflammation of cerebral blood vessels.
Convexal SAH may be the first imaging manifestation of CNS vasculitis which can caused by primary CNS vasculitis or be secondary to collagen-vascular disease or autoimmune diseases.
Radiological features: MRI may show multifocal lesions involving the hemispheric cortex,
subcortical white matter and basal ganglia.
Cerebral angiography typically reveals multiple segmental narrowing of the medium and small sized arteries (Fig. 6) .
B.
Venous Sinus Thrombosis (Fig. 7)
C.
Vascular Malformations (Fig. 8)
4.
Mimics
Several imaging patterns can mimic convexal SAH:
- Fig. 9: CT brain post cardiac catheterisation.
- Fig. 10: CT brain during post-ictal state.
- Fig. 11: CT brain in anoxic hypoxic brain injury