Aim:
- To discuss types of Invasive Placental Disease (IPD)
- To describe the features of US and MRI in diagnosing IPD
- To calculate the sensitivity of US Vs MRI with the gold standard intra operative findings
- To calculate other statistical parameters by comparing US and MR findings
- To see how MRI can be used as a problem solving tool in equivocal cases
Background:
Invasive Placental Disease (IPD) occurs when there is a defect in the decidua basalis,
resulting in an abnormal invasion of the placenta into the substance of the uterus.
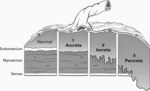
IPD is classified on the basis of the depth of myometrial and serosal invasion as:
- Placenta accreta
- Placenta increta
- Placenta percreta
1.
Placenta Accreta
This is the mildest form of IPD where the villi are attached to the myometrium but do not invade the muscle.
The prevalence of Placenta Accreta is 75%.
2.
Placenta Increta:
This is the intermediate form of IPD where the villi partially invade the myometrium.
The prevalence of Placenta Increta is 20%.
3. Placenta Percreta:
This is the most severe form of IPD where the villi penetrate through the entire myometrium or beyond serosa.
The prevalence of Placenta percreta is 5%.
Risk Factors:
- Previous Caesarean section is the most common risk factor
- Placenta Previa is the second most common risk factor
- Uterine Anomalies
- Previous uterine surgery e-g myomectomy or dilatation and curettage
- Uterine irradiation
- Advanced maternal age > 35 years
- Scar pregnancy
- Multiparity
- Intra uterine adhesion bands (Asherman Syndrome)
- Hypertensive disorder of pregnancy
- Smoking
Serum Markers:
- Elevated levels of α- fetoprotein
- Elevated levels of human chorionic gonadotropin
Complications:
- Massive intrapartum hemorrhage
- Disseminated intravascular coagulation
- Sepsis
- Deep venous thrombosis
- Damage to uterus
- Damage to local organs like bowel,
bladder or ureters
- Amniotic fluid embolism
- Multisystem organ failure
- Feto-Maternal Death
Diagnosis:
Ultrasound Evaluation:
Ultrasonography is the primary diagnostic tool for detecting Invasive Placental Disease (IPD).
US have sensitivity of 89.5%,
Positive Predictive Value of 68% and Negative Predictive Value of 98% for the diagnosis of (IPD).
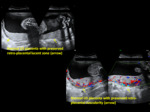
Normal Placenta appears hyperechoic on US surrounded by the hypoechoic myometrium.
A thin hypoechoic line at the inner aspect of the myometrium called the retro-placental hypolucent clear space separates myometrium and placenta.
On US color Doppler normal placenta shows smooth and continuous sub placental blood flow that parallels the myometrium.
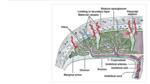
The following sonographic criteria are used for the diagnosis of IPD.
- Marked thinning,
loss or irregularity of retro-placental hypolucent zone.
(sensitivity only 7%,
can be found in normal pregnancies)
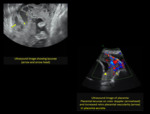
- Interruption of the hyper echoic border between the uterine serosa and bladder wall,
which is replaced by multiple bridging vessels.
- Interrupted and irregular intra-placental vasculature.
- Turbulent placental lacunae with high flow velocity (highest sensitivity 78-93%)
- Myometrial thickness <1mm.
MR imaging Evaluation:
Although US remain the primary diagnostic criteria,
MRI has added value to the cases that appear equivocal on US as in the cases with posteriorly implanted placenta or morbidly obese patients.
MR is usually not performed in the first trimester due to theoretical risk to the embryo.
MR technique:
Two main sequences are usually acquired in all three planes:
- single-shot fast spin echo (SSFSE) or half-acquisition turbo spin echo (HASTE)
- balanced steady state free procession (bSSFP)
Additional oblique planes are also frequently done.
An axial T1 fat-suppressed is performed to evaluate blood products.
Diffusion-weighted sequences have also been used by some to evaluate the placental-myometrial interface.
Intravenous gadolinium contrast is not generally used out of potential risk to the fetus.
However,
recently some centers have started using contrast enhanced examinations.
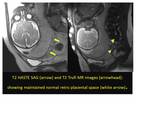
Normal placenta shows homogeneous intermediate signal intensity on T2 weighted images usually clearly separate from the underlying myometrium.
Thin linear hypointense T2 areas are seen running through the myometrium which are normal placental septa.
The myometrium shows three layers,
the hypointense outer and inner layers and hyperintense middle layer which contains multiple flow voids representing normal myometrial vascularity.
The following MR imaging features are seen in Invasive Placental Disease (IPD):
- Focal uterine bulge that disrupts the normal pear shape of the uterus.
- Heterogeneous T2 signal intensity.
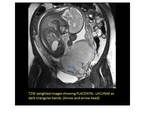
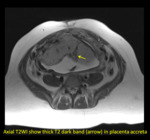
- Thick linear dark T2 bands in random distribution.
- Focal thinning of the myometrium and interruption of the junctional zone.
- Disorganized abnormal intra-placental vascularity.
- Thinning or loss of retro-placental T2 dark zone.
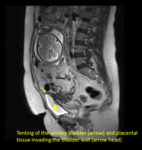
- Invasion of adjacent organs and tenting of the bladder.