IODINE MAPS OF THE LUNG: TECHNICAL ASPECTS
There are two ways to obtain iodine maps: dual-energy and subtraction.
We will focus on subtraction technique.
To get perfusion maps based on subtraction technique two scans of the lungs are consecutively obtained.
The first non-contrasted scan is followed by a contrast-enhanced scan.
The contrast-enhanced scan is acquired using bolus tracking in the pulmonary trunk; therefore,
it will be equivalent to conventional CTA.
Both scans use the same scanner settings except for a lower dose in the pre-contrast scan.
After both acquisitions,
a software automatically subtracts the pre-contrast from the post-contrast scan.
Iodine maps should be understood as complementary techniques to CTA.
BASIC INTERPRETATION OF IODINE MAPS
Iodine maps must be evaluated carefully,
as they are very sensitive to artefacts.
Every suspicious finding must be thoroughly evaluated and compared to CTA.
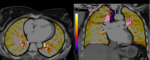
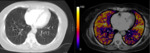
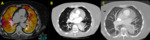
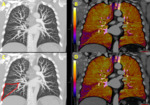
Under normal conditions,
contrast agent is distributed along all vascular territories of the lung,
resulting in a homogeneous yellow-orange perfusion map,
uniformly painting all pulmonary territories (figure 1).
The presence of this single-bright color map,
uniformly distributed,
suggests that contrast material has been placed homogeneously along all pulmonary parenchyma,
with no filling defects.
Therefore,
pulmonary emboli (acute and chronic) can be ruled out.
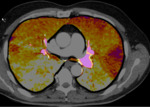
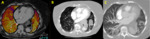
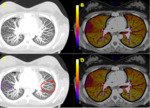
An area of hypoperfusion is by definition an area of decreased blood flow.
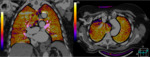
Following the same reasoning,
absent or diminished blood flow to a pulmonary territory implies partial or total reduction of iodinated-contrast delivery to that segment.
Perfusion maps will represent this asymmetry in contrast´s distribution as a mixture of well-perfused yellow-orange areas and not-perfused blue-purple areas (figure 2).
Perfusion studies showing not-uniform color maps,
especially when blue-purple areas are present,
are highly suggestive of affected vascular structures: and thus,
further assessment will be necessary.
However,
not every blue-purple area means diminished perfusion.
There are some conditions that may also alter the uniformity of the color distribution in iodine maps.
Radiologist must be aware of these false positives:
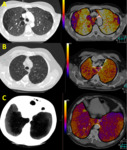
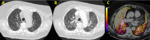
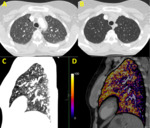
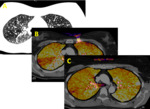
- Bullae and emphysema: Areas of abnormal enlargement of the airspaces and destruction of the alveolar wall; diffuse (emphysema) or focal (bullae).
Figure 3.
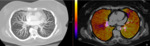
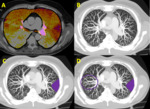
- Lung fissures: formed by double-fold of visceral pleura may sometimes simulate hypoperfused areas (figure 4).
- Motion artifact: It is a patient-based artifact,
voluntary or involuntary,
that occurs due to patient´s movement during image acquisition.
It may mimic pathology.
It might be detectable in CTA by a blurring,
streaking,
or shading in the image (figure 5).
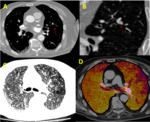
- Beam hardening artifacts: due to intravenous contrast in the superior vena cava,
it may cause bright-color bands in lung apices and pseudo-altered blue-purple imagines in the adjacent lung segments (figure 6).
- Air trapping and mosaic attenuation pattern,
which will be discussed later.
In addition,
gravity affects the regional distribution of ventilation and blood flow in the lung,
in terms of vertical gradients of pleural pressure and pulmonary vascular pressures.
Therefore,
in supine patients,
most anteriorly located segments,
such as middle lobe,
will physiologically show a lower perfusion (figure 7).
Mosaic pattern: how to face lucencies and densities in the lung
Areas of increased density
On our own experience areas of increased density,
such us,
consolidations,
atelectasis,
ground-glass opacities and interstitial pattern seem not to be valuable by iodine maps.
We find that almost every area of increased density corresponds to a blue-purple zone in color maps,
while most of the times they are not consistent with hypoperfused areas.
We infer that it could be due to a non-homogenous distribution of the contrast and a limitation of the subtraction technique.
These areas,
which are hyperdense both in non-contrast scans and in CTA,
seem to be erroneously detected by the software and not subtracted.
The software finds no difference before and after contrast administration.
The result is a mistaken interpretation of the dense area represented as hypoperfused parenchyma.
In addition,
this phenomenon could also be influenced by vascular factors.
These factors include modifications due to the primary process (such us increased vascularization in infectious disease) or due to compensatory mechanisms (re-distribution of blood flow to well-ventilated segments).
They may affect contrast agent-distribution and result in non-homogeneous deposition,
contributing to an altered color map.
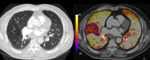
A representative example of this phenomenon is usually seen in the posterior-basal segments of both lungs in supine patients; where alveoli tend to collapse.
These hypoventilated areas not necessarily need to be hypoperfused although they are always interpreted as non-perfused areas in iodine maps (figure 8).
Another example is usually seen in mosaic pattern due to air trapping,
which results in some low-attenuated areas (air trapping) and other dense areas.
As the primary alteration is on the airways,
non-altered perfusion should be seen.
However,
dense areas are always drawn blue-purple in perfusion maps (figure 9).
Areas of low attenuation (lucent areas)
On the contrary,
iodine maps seem to be very helpful to evaluate low attenuated segments of the lung,
as they may discern if the lucency is due to a problem in the vascular bed or in the bronchial tree.
When assessing a low attenuated area on CT,
there are two possible situations:
On the one hand,
the lucency may correspond to a hypoperfused area in the color map.
It may be inferred that the lucency is consequence of primary vascular problems (limited contrast delivery or diminished amount of vessels).
Correlation between CTA and iodine maps is mandatory in these cases.
We strongly recommend using post-processing techniques such as Maximum Intensity Projection (MIP) to improve the assessment.
When CTA shows decreased amount of vessels and/or abnormal morphology or caliber of vessels in the area of hypoperfusion,
there is a miss-match between both techniques.
Therefore,
we can assume that some vascular problem is the primary cause for the lucent area (figure 10).
Chronic thromboembolism is a diagnostic option that suits in this pattern many times.
However,
we might find a lucent and hypoperfused area which does not meet miss-match criteria (figure 11).
In these cases vessels on CTA are normal (in quantity,
morphology and caliber).
On our experience these findings should be interpreted carefully,
taking into account all clinical and radiological aspects.
Most of the times,
they are consequence of artifacts or physiological areas of hypoperfusion.
On the other hand,
iodine maps can show well-perfused lucent areas.
We can assume that vascularization is correct; and thus,
lucencies must be the consequence of pathology in the airways (air trapping or others).
Figure 12.
When mosaic pattern is secondary to air trapping,
it usually tends to disappear in inspiratory scans.
If the altered pattern persists in both expiratory and inspiratory CT,
other pathologies of the bronquial tree should be further studied.
DIAGNOSIS OF CHRONIC PULMONARY THROMBOEMBOLISM USING IODINE MAPS
We defined some criteria for the diagnosis of chronic pulmonary thromboembolism in iodine maps.
These criteria have been developed taking into account that iodine maps are very sensitive to artifacts.
Every area of presumed hypoperfusion should be carefully evaluated and correlated with CTA.
To consider cPE,
a suspicious area must meet at least 5 criteria:
- Localization: the abnormal lung segment must be located in the same territory where the acute emboli took place.
- Morphology: Subpleural,
triangular or wedge-shape.
- Color: consistent with hypoperfusion (blue or purple).
- Miss-match: There must be correlation between the hypoperfused area of the color map and abnormal vessels on CTA.
Post-processing techniques (MIP) might be helpful to demonstrate this altered vessels.
- Absent of pitfalls: The pathologic area should not overlap with pitfalls (false positive).
Only after having checked every feature we can assume that the abnormal lung segment is related to cPE.
As mentioned,
these patients are in high risk of developing CPEH,
and thus,
should undergo specialized care.
See examples of cPE meeting all criteria in figures 13,
14,
15,
16 and 17.
OUR RESEARCH LINE
Hypothesis
Iodine maps represent the distribution of iodinated contrast in the pulmonary capillary bed using a color scale.
Therefore,
they allow evaluation of small-sized arteries of the peripheral territories.
It is outlined as a suitable technique to study the pulmonary microcirculation.
Combination of CTA and Iodine maps could combine specificity and sensibility of CTA in evaluating proximal territories and the ones of the Iodine maps in assessing distal vasculature.
Therefore,
global diagnostic capability in detecting chronic pulmonary thromboembolism will increase.
To demonstrate our hypothesis a retrospective observational study was planned.
Between January 2016 and May 2017 a cohort of 86 patients with diagnosis of acute PE was studied.
After 6 months of anticoagulant therapy all patients underwent CTA and iodine map to asses for residual emboli (cPE).
We compared proportion of cPE detected by CTA with proportion of cPE detected after combination of CTA and iodine maps.
Results
CTA: CTA was able to detect 25 cases of chronic pulmonary thromboembolism; while resolution of acute emboli was seen in 61 patients.
|
|
Frequency
|
Percentage
|
|
No cPE
|
61
|
70,9
|
|
cPE
|
25
|
29,1
|
|
Total
|
86
|
100.0
|
Combination of CTA and Iodine maps: Assessment of both techniques allowed diagnosing 36 people with chronic pulmonary thromboembolism.
|
|
Frequency
|
Percentage
|
|
No cPE
|
50
|
58,1
|
|
cPE
|
36
|
41,9
|
|
Total
|
86
|
100.0
|
False negative (CTA):
|
|
Frequency
|
Percentage
|
|
No cPE
|
75
|
87,2
|
|
cPE
|
11
|
12,8
|
|
Total
|
86
|
100.0
|
Analysis
In a cohort of 86 patients CTA could detect 29.1% of cPE; while simultaneous assessment of CTA and iodine maps increased detection up to 41,9%.
The false negative rate for CTA is 30.56% (95%CI: 18.0% - 46.9%).