Keywords:
Multidisciplinary cancer care, Venous access, Ultrasound, Fluoroscopy, Veins / Vena cava, Oncology, Interventional vascular
Authors:
I. Jurca, R. Smiljanic, M. Prutki, A. M. Alduk; Zagreb/HR
DOI:
10.1594/ecr2018/C-0782
Methods and materials
A total of 159 consecutive patients referred for port system implantation between August 2015 and March 2017 were included in this retrospective study.
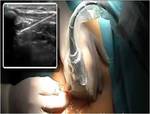
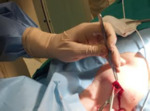
All procedures were performed in local anesthesia using ultrasound-guided puncture of the internal jugular,
subclavian or femoral vein ( Fig.
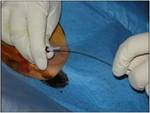
1). After inserting the guidewire in the right atrium or inferior vena cava under fluoroscopy guidance,
a peel-off sheath was inserted.
Through the sheath,
a polyurethane or silicone catheter was deployed,
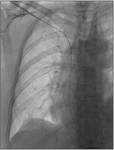
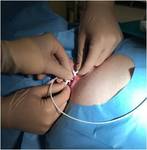
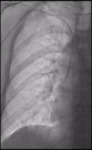
after which a sheath was extracted (Fig.
2,
3 and 4). A 3 cm-long subclavicular incision was made to form a subcutaneous pocket ( Fig.
5). A catheter was then pulled through the subcutaneous tunnel,
with the tip positioned under fluoroscopy guidance at the cavoatrial junction ( Fig.
6).
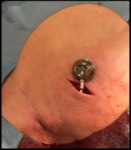
The catheter was connected to port system chamber (Fig.
7),
which was placed in the subcutaneous pocket.
The correct port system position was confirmed under fluoroscopy,
after which a port system was flushed with 5 ml of heparinized saline ( 100 I.U.).
The incision was closed with subcutaneous and intracutaneous resorptive sutures.
The medical records of all patients were reviewed and demographic data,
indications,
puncture site,
duration time,
and complications were analyzed.