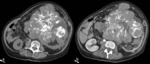
Angiomyolipoma
Angiomyolipoma (AML) is the most common benign solid renal tumor.
Most AMLs are composed of variable amounts of fat,
smooth muscle and abnormal blood vessels.
AMLs can be associated with tuberous sclerosis (20% of cases).
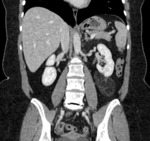
The risk of hemorrhage is related to the size of the tumor,
and it is significantly higher in lesions greater than 4 cm in diameter (Fig 4).
On US,
AML is a circumscribed,
highly reflective mass,
more echogenic than the central sinus fat; renal cell carcinoma is also hyperechoic,
but the lesion echogenicity is usually less than that of renal sinus.
As the amount of fat deceases,
the lesion echogenicity also decreases [4].
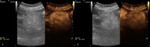
Fat-poor AML exhibits mixed echotexture,
being hyperechoic and isoechoic compared with renal parenchyma (Fig 5).
Unenhanced CT clearly depicts a hypoattenuating area (≤ –10 HU) suggesting fat in fat-rich AML. The amount of fat present is variable and it can even be absent [4].
This is especially the case in the setting of tuberous sclerosis,
where up to a third do not demonstrate macroscopic fat on CT.
Calcification is rare.
Contrast-enhanced CT is not necessary for diagnosing fat-rich AML but should be performed when there is potential for tumor bleeding.
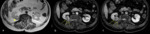
Contrast-enhanced CT frequently shows heterogeneous enhancement within fat-poor AMLs because a small amount of fat is localized or scattered (Fig 6).
On T2-weighted MR images,
fat-rich AML is usually hyperintense compared with renal parenchyma,
but has various signal intensities according to the amount of fat.
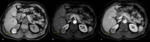
At Chemical Shift Imaging,
fat-rich AML exhibits a decrease in signal intensity on opposed-phase MR images. However,
renal masses that demonstrate chemical shift suppression throughout the mass (but do not suppress on frequency selective fat suppression techniques) can be due to clear cell RCC or angiomyolipoma with small amounts of fat cells dispersed throughout the mass (Fig 7).
However,
these findings are not specific enough to make a confident diagnosis of a non–fat containing angiomyolipoma.
In some cases,
biopsy of the renal mass may be indicated to make a definitive diagnosis of an angiomyolipoma and to avoid surgery [5].
Oncocytoma
The oncocytoma is the most common solid,
non–fat-containing renal mass,
accounting for about 5% of renal cortical neoplasms.
Although oncocytomas are considered benign,
some demonstrate invasive features.
Renal oncocytomas demonstrate various imaging findings.
A central scar may be a characteristic finding,
especially in a large mass.
On US it is represented as a solid mass with internal echoes or,
occasionally,
with a stellate hypoechoic centre; the echogenicity of the mass can be variable (Fig 8).
On CT,
the difference in cellularity and stroma may influence the degree of tumour enhancement and characteristic enhancement pattern of individual oncocytomas.
Segmental enhancement inversion is a characteristic enhancement pattern of oncocytoma [6].
It deals in two distinct zones of enhancement which show inverse patterns between the corticomedullary (30–40 s) and early excretory (120–180 s) phases (Fig 9).
When cystic changes and haemorrhage are extensive,
oncocytomas may present as a hypovascular mass.
On MRI,
the high cellular component demonstrates moderate signal on T2-weighted images and relatively high signal on diffusion-weighted imaging.
High T2 signal within the tumour may reflect oedematous stroma,
central scar or cystic change.
Dynamic contrast-enhanced MRI findings are similar to CT [6] (Fig 10).
Renal Cell Carcinoma (RCC)
Renal Cell Carcinoma (RCC) represents about 85% of all malignant renal tumours.
It can be bilateral in 3–5% of cases.
Anymay,
any solid renal mass should be considered suspect for RCC until proven otherwise.
The classic triad of RCC (hematuria,
flank pain,
and a palpable abdominal mass) is now seen in a very small minority of patients; most newly diagnosed RCCs are discovered incidentally during imaging performed for nonurologic symptoms.
Clear cell RCC,
previously referred to as "conventional RCC",
is the most common histologic subtype.
Imaging features reflect the variegated histologic findings of clear cell RCC.
Clear cell RCC commonly appears heterogeneous at imaging,
due to the presence of hemorrhage,
necrosis,
and cysts [7].
On US,
it appears as heterogeneous,
hypoechoic or mildly hyperechoic mass (Fig 11).
The inherent vascularity of conventional RCC characteristically produces strong enhancement in the mass on cortico-medullary-phase CT images: the change is often in excess of 100 HU from unenhanced to contrast enhanced images (Fig 12).
The degree of contrast enhancement on CT and on MRI may help distinguish clear cell RCC from non–clear cell variants.
Clear cell RCC is hypo- to isointense on T1-weighted MR images and iso- to hyperintense on T2-weighted MR images.
Lesions with microscopic lipid content show a conspicuous drop in signal intensity on images obtained at an opposed-phase echo time compared to in-phase gradient-echo images (Fig 13).
Calcification,
sometimes ossification,
is seen in 10%–15% of tumors.
Capsular or renal vein invasion is seen in up to 45% of tumors (Fig 14).
Lungs (75%),
liver (40%),
bone (40%),
soft tissues (34%) and pleura (31%) are common target sites of metastasis [7].
Hypovascular Carcinoma
Papillary RCC,
the second most common RCC histologic subtype,
accounts for 10%–15% of tumors,
while chromophobe-type RCC represents just 5%.
Some papillary RCCs exhibit little contrast enhancement (an increase of only 10–20 HU between unenhanced and enhanced images in CT or MRI),
making differentiation from a renal cyst difficult (Fig 15,
16).
Papillary RCC commonly demonstrates low signal intensity on T2-weighted MR images possibly due to the presence of by-products of hemorrhage and necrosis.
Unlike clear cell RCC,
papillary RCC demonstrates relative hypovascularity (Fig 17).
Chromophobe RCC appears uniformly hyperechoic at ultrasonography.
Despite their large size,
chromophobe RCCs demonstrate relatively homogeneous enhancement at CT and MR imaging.
A spoke-wheel pattern of contrast enhancement,
classically associated with oncocytomas,
has recently been described in association with chromophobe RCC [7].
Medullary Carcinoma
Renal medullary carcinoma,
also referred to as "the seventh sickle cell nephropathy",
is an extremely rare malignant neoplasm occurring almost exclusively in patients with sickle cell trait.
Renal medullary carcinoma is hypothesized to arise from medullary collecting ducts.
It is almost always found in young patients.
Sarcomatoid Carcinoma
Sarcomatoid renal cell carcinomas (sRCC) may develop when one of the more common subtypes of renal cell carcinoma degenerates into a sarcoma.
On imaging,
they are generally large masses,
with irregular contours and malignant-appearing,
but do not have specific imaging features (Fig.
18).