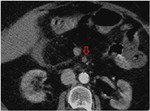
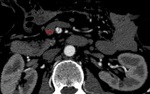
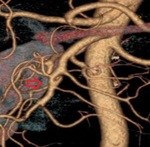
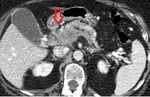
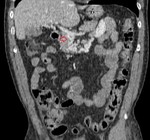
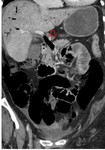
Causes of MI:
Embolism of the superior mesenteric artery (SMA): it is the most frequent cause of MI,
with an incidence of up to 60% of the ischemia.
It is produced by an embolus that originates in the left atrium or due to an arrhythmia (atrial fibrillation) or in hypokinetic regions produced by a previous myocardial infarction.
The superior mesenteric artery is the visceral vessel most susceptible to emboli due to its acute angle,
long diameter,
and high flow.
About 15% of the emboli are affected at the origin of the SMA,
while the rest can be located between 3 and 10 cm from the origin,
close to the emergence of the middle colic artery.
Up to 20% of the cases of emboli located at the origin of the SMA are associated with emboli elsewhere in the vascular branches.
Mesenteric arterial thrombosis: Arterial thrombosis is typically associated with preexisting atherosclerosis.
Responsible for 20-30% of the causes of MI.
In contrast to the abrupt presentation of occlusion by embolism of the superior mesenteric artery,
in more than 50% of cases,
a history of intestinal angina is present.
Patients with mesenteric arterial thrombosis have a history of symptoms such as post prandial pain and weight loss.
Thrombosis is observed proximal to the origin of the artery (in association with atherosclerosis that causes stenosis),
as opposed to embolism,
which is located more distally.
It can occur in patients with mycotic aneurysm,
dissection of the mesenteric artery and in vasculitis.
Mesenteric venous thrombosis: Represents 5-15% of MI cases.
95% affect the superior mesenteric vein.
60% of patients have a history of peripheral venous thrombosis.
The risk factors associated are: portal hypertension,
hypercoagulation,
trauma,
abdominal inflammatory diseases,
recent surgery (splenectomy).
It can be acute (appearance in minutes or hours) subacute (pain lasts for days or weeks) or chronic (months or years).
In the case of acute thrombosis,
it is the one with the greatest risk of intestinal ischemia and peritonitis,
the subacute is not as frequently associated with intestinal ischemia and the chronic is associated with important collateral venous circulation and manifests as complications of portal thrombosis or splenic.
Thrombosis of intraabdominal causes begins in the vessels of greater caliber and progresses peripherally,
affecting the smaller branches,
however when the cause is due to a prothrombotic state,
they begin in the small vessels and progress affecting the major vessels.
Isolated thrombosis of the proximal mesenteric vein usually does not produce severe ischemia because of the collaterals between the mesenteric veins and the systemic veins.
Distal thrombosis (hypercoagulability) is associated with ischemia of the intestinal wall.
There is a reduction of the venous return,
this produces a mural edema,
microvascular perfusion alteration,
intestinal distention and segmental or total infarction.
Ischemia leads to intestinal anaerobic metabolism,
local acidosis and pain due to hypoperfusion.
The location of the thrombus in the vein in relation to the mesenteric circulation,
the extension,
the presence or absence of collateral circulation are important factors to predict intestinal ischemia and infarction.
Dissection of the superior mesenteric artery: Rare.
5% of patients with mesenteric dissection develop MI as a complication.
The etiology of the dissection isolated from the AMS could not be clarified,
usually starting at a distance of 2 or 3 cm.
The AMS is more susceptible to tensile forces in a transition zone between the fixed retro-pancreatic proximal part of the artery,
and the more distal,
relatively mobile part that pivots according to bowel movement.
It is at this point that an intimal flap is normally formed that allows the entry of blood into the middle layer,
which causes a longitudinal dissection along the laminar plane of the vessel.
Aortic dissection: 5% of patients with aortic dissection develop MI.
The dissection may extend to the proximal portion of the vessels and reduce flow or cause complete obstruction.
NOMI (non-occlusive mesenteric ischemia): occurs due to hypoperfusion and reduction of mesenteric blood supply without vascular obstruction.
It is the result of reflex vasoconstriction,
hypotension or vasoconstrictor drugs (digitalis,
vasopressin,
amphetamines,
cocaine) and its consequences range from reversible damage to severe involvement of the entire intestine.
Other causes are shock,
hypovolemia,
dehydration,
chronic renal failure.
Arcuate ligament syndrome:The middle arcuate ligament of the diaphragm is made up of muscle fibers that connect the right and left diaphragmatic crura together,
forming the anterior margin of the aortic hiatus,
almost always located above the origin of the celiac trunk,
at the level of the first lumbar vertebra.
In 10 to 24% of people may have a more caudal location,
which conditions a previous compression and indentation characteristics in the celiac trunk.
It usually affects young women (20 to 40 years old).
Other:
Vasculitis:
Takayasu arteritis,
polyarteritis nodosa and mediolitic arteriopathy.
They produce stenosis,
occlusion,
aneurysms,
thickening of the arterial wall with reinforcement in the contrasted phase.
Connective tissue disorders: Ehlers-Danlos syndrome.
Intestinal wall:
It is composed of inside out by 4 layers: the mucous membrane,
submucosa,
muscular layer and serosa.
MI has three stages according to the involvement of the different layers of the intestine:
- Also known as colitis or reversible ischemic enteritis.
Erosion and / or necrosis of the mucosa occurs.
It can heal spontaneously,
without leaving sequels.
- When the damage extends to the deep submucosa and muscular layers.
Reparative changes can produce fibrotic stenosis.
- Transmural necrosis: necrosis of the wall (infarction) has already occurred.
It is associated with a high mortality rate and requires immediate surgical intervention.
Portal pneumatosis or mesenteric venous gas in the MI,
are the result of various factors such as the integrity of the mucosa,
gas and intraluminal pressure and bacterial flora.
Pneumatosis intestinalis is a finding of an underlying pathological process.
The finding of mesenteric porto venous gas is very suggestive of intestinal necrosis.
When arterial obstruction occurs,
the initial response is the reversible vasodilatation of the splanchnic branches,
which in the CTMS are visualized as the increase in the attenuation of the wall of the intestinal loops.
If the obstruction persists,
vasoconstriction occurs and is seen as a decrease in the reinforcement of the walls of the intestinal loops,
thickening of the intestinal,
mural edema,
decreased peristalsis,
distension and dilation.
In MI due to venous obstruction,
marked mural thickening of the intestinal wall is observed,
with a "target" appearance due to submucosal edema.