Consecutive cases treated at the interventional radiology service over 4 years period from Sep 2013 to April 2017 were included in the study.
Minimum follow up of any case was six months.
Preoperative clinical data and the follow up findings recorded by the surgeon colleagues (KB,
BK,
SK) were retrieved and charted,
and the images reviewed by the radiologists (SK,
PK).
All interventions had been done by single operator (SK).
Syndromic malformations were excluded from the review.
Oral cavity and tongue lesions were not included as these are managed under a different protocol.
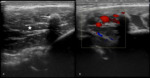
Diagnostic ultrasound (US) and color doppler examination (Fig 1) was done by either of the two radiologists using 6-15 Mhz linear probe.
Magnetic resonance imaging (MRI) study included at least T1 and T2 weighted images,
and post contrast fat-suppressed T1 images wherever available.
A goal was set for each patient,
relating to their chief complaints.
Subsequently they underwent sclerotherapy usually every 2-4 weeks,
sometimes delayed upto 3 months also.
For sclerotherapy,
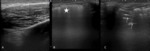
US (Fig 2),
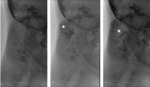
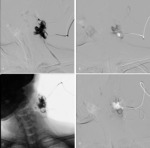
fluoroscopy (Fig 3),
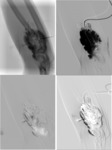
double/multiple puncture (Fig 4),
negative filling technique (Fig 3,4,5),
digital subtraction phlebography (Fig 5) were used alone or in combination. Puncture of VM was done using 22G needle under US guidance.
Microfoam was prepared using 3% polidocanol (Asklerol,
Samarth Life Sciences Pvt Ltd,
Mumbai,
India) and room air in 1:4 ratio using air using Tessari’s method.
[7,8]
Pain reduction,
swelling reduction,
imaging resolution and patient satisfaction were evaluated using chi-square,
paired t-test and regression analyses.
The lesions were classified using three classification systems
I. A descriptive classification scheme derived from the Hamburg’s calssificatio,
in which lesions were divided into three categories:
II. An US based classification,
developed by the authors,
[9] in which the lesions were classified into four types.
1. type I was a well-defined predominantly echogenic or hypoechoic mass,
partially or poorly compressible,
without visible connection to adjacent veins
2. type 2 was a well-defined mixed echogenicity lesion with up to 50% anechoic spaces and partially compressible with or without few connections to adjacent veins
3. type 3 lesions were significantly anechoic lesions with tubular or serpentine channels and/or anechoic spaces with or without connections to normal or dilated adjacent venous system
4. type 4 was a totally diffuse or dysmorphic lesion with or without direct connections to adjacent veins.
III.
An imaging classification originally given on direct puncture phlebographic appearance –the Puig’s classification.
[10,11].
Oral paracetamol (PCM) was prescribed,
if needed,
for pain relief after the procedure.
Non-steroidal anti-inflammatory drugs (NSAIDs) were prescribed only if pain was not controlled by PCM.
Post-sclerotherapy follow-up US was done at 2-4 weeks and if needed further sclerotherapy sessions were repeated.
Outcome at 6 months follow up (clinical and US) after the last session were taken as end point for this study.
Follow up MRI scans were not taken into consideration for the study.
Imaging findings were classified into four groups: (1) excellent resolution(2) satisfactory resolution (3) fair resolution: the VM had resolved by upto 50% of original and seen as partially shrunken mass with partial decrease in the sinusoidal spaces; and (4) poor resolution.
Excellent and satisfactory resolution on US were taken as ‘good response to therapy’ while fair or poor resolution were taken as ‘poor response to therapy’.
Patient satisfaction was measured by a 4 point classification scheme as very satisfied,
satisfied,
neutral and dissatisfied.
The extent of resolution of original clinical presentation (swelling and pain),
was classified as markedly improved,
moderately improved,
no change,
and worsening.
Markedly improved and improved classes for swelling and pain were considered as ‘good response to therapy’ while no change or worsening were considered as ‘poor response to therapy’,
and similarly very satisfied and satisfied were considered as ‘satisfaction to therapy’ and neutral or dissatisfied were considered as ‘dissatisfaction to therapy’.
Pain was also scored on a 0-10 point scale and change in the score was noted.