ANATOMY
Anatomically,
the cavernous sinuses (CS) are paired structures located immediately lateral on either side of the sella turcica and they measure approximatively 2 cm anteroposteriorly,
1.3 cm in vertical dimension and 1 cm lateral width.
The cavernous sinus is a septate venous channel formed by the splitting in two layers of the dura.
The outer layer of the dura is in direct contact with bony structures,
while the inner layer is in contact with either blood or cerebrospinal fluid.
(15,18)
CAUSES
Carotid-cavernous fistulas (CCFs) are a rare and serious disorder consisting of an abnormal communication between the carotid arterial system and the cavernous sinus.
This disorder may appear either spontaneously or be posttraumatic in origin.
In 75% of cases the cause of CCF was secondary to craniocerebral trauma,
basilar skull fracture being among the most common and less commonly the cause may be projectile or slash injuries,
sinus surgery,
endovascular procedures,
transsphenoidal exploration etc.
Traumatic causes tend to affect young male patients,
while spontaneous causes are usually found in older female patients.
There are predisposing factors that may contribute to formation of spontaneous CCFs such as ruptured cavernous ICA aneurysms,
genetic disorders such as Ehlers-Danlos syndrome and fibromuscular dysplasia.
In these patients with arterial wall defects,
pregnancy,
hypertension,
minor trauma and collagen vascular disease may provide a final step leading to rupture of the vessel and formation of a fistula.(15)
CLASSIFICATION
The arterial-venous fistulas of the cavernous sinus may be classified according to anatomy,
etiology,
hemodynamics and angiographic arterial architecture.
Anatomically and according to the angiographic appearance CCFs can be of two distinct types direct or indirect fistulas.
Direct CCFs: In this type the internal carotid artery (ICA) communicates directly with the cavernous sinus and a large-volume arteriovenous shunt is present.
Hemodynamically they are high-flow fistulas and etiologically the most common causes are either traumatic in origin or aneurysmal rupture in the cavernous portion of the ICA.
The clinical aspects of these fistulas include: proptosis,
chemosis,
orbital bruits,
diplopia,
blurry vision and orbital pain.
These symptoms may be produced by retinal ischemia which is an indication for urgent intervention.
Indirect CCFs (Dural cavernous sinus fistulas) represent an abnormal communication between the meningeal braches of the external or internal carotid artery and the cavernous sinus.
From a hemodynamic standpoint they are low-flow fistulas usually presenting with a more covert onset.
The patient may present with conjunctival injection and in such cases,
the diagnosis can be missed initially because of confusion with conjunctivitis.
An important classification of CCFs was made by Barrow et al.
who defined 4 types according to the angiographic findings based on their arterial supply.
Type A CCFs are the most frequent,
representing approximately 75%–80% of CCFs.
These are direct fistulas that connect the intracavernous segment of the internal carotid artery directly to the cavernous sinus resulting in high-flow rates.
Type B,
C and D are indirect CCFs (dural arteriovenous fistulas) with low-flow rates.
Type B CCFs: dural communication between meningeal branches of the ICA and the cavernous sinus.
Type C CCFs: dural communication between meningeal branches of the external carotid artery (ECA) and the cavernous sinus.
Type D CCFs: are the most prevalent form of indirect CCFs,
they are a dural communication between the meningeal branches of both the ICA and the ECA,
and the cavernous sinus.
CLINICAL PRESENTATION
The communication between the ICA and CS has important clinical consequences by the hemodynamic changes that it produces; it determines the increase of blood volume and pooling,
it increases venous pressure,
determines reversing of the ophthalmic vein flow,
and reflux into cortical veins and other venous sinuses.
These changes determine the neuro-ophthalmic symptoms that the patients present.
(1)
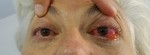
Case 1: A 66 year-old female with indirect type D CCF,
presenting with bilateral subconjunctival injection,
conjunctival edema and bilateral palsy of nerve abducens.
Fig. 1