MRI helps in better tissue characterization with the aid of multiple parameters of the T1 and T2 weighted sequences.
There is inherent contrast between soft tissue and fluid filled structures.
Fetal as well as maternal anatomy can be accurately evaluated.
Single-shot fast spin-echo (SSFSE) T2-weighted imaging or half-Fourier single shot turbo spin-echo (HASTE) are commonly used sequences.
The spatial resolution of T1 weighted sequence improves with gestational age.
Gradient echo sequences (EPI) and true fast imaging with steady state precession (FISP) are better for detecting bony and vascular abnormalities.
Neurological abnormalities includes:
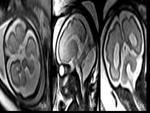
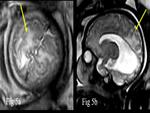
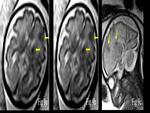
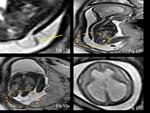
Dandy-Walker malformation is one of the major causes of congenital hydrocephalus.
It is confirmed on MRI with presence of large posterior fossa in communication with the fourth ventricle,
marked degree of ventriculomegaly,
hypoplasia of the cerebellar vermis and the associated hypogenesis of the corpus callosum (Fig.
1).
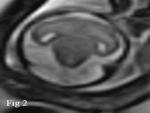
Holoprosencephaly is a congenital anomaly characterized by lack of cleavage of the prosencephalon,
it is divided into 3 types; alobar,
semilobar,
and lobar forms,
prenatal diagnosis of the less severe forms can be difficult.
Absence of the septum pellucidum is the key finding on MRI (Fig.
2).
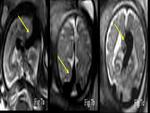
Anencephaly is the most severe form of cranial neural tube defect (NTD) detected on MR.
It is usually diagnosed antenatally (Fig.
3).
Cysts of extra-axial origin are mostly Arachnoid cysts.
Primary arachnoid cysts are filled with cerebrospinal fluid and they are usually not connected to the subarachnoid space [4]. Arachnoid cysts are intracranial,
extra-axial mass lesions (Fig.
4).
Cerebral white matter injury,
consisting primarily of Periventricular leukomalacia (PVL) is manifested clearly on MRI confirming the ultrasound diagnosis (Fig.
5).
It is commonly seen in the periventricular region and leads to cyst formation and later necrosis and vetriculomegaly.
is PVL is a major cause of Cerebral palsy CP,
accurate prenatal diagnosis of PVL can aid proper counseling about the prognosis and possible early treatment.
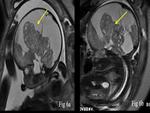
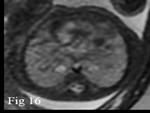
Choroid plexus papilloma presents as a solid intraventricular vascular tumor with or without calcification (Fig.
6).
It is commonly associated with hydrocephalus.
MRI helps to rule out hematoma and study the exact extent of the lesion.
Fetal MRI aids in prenatal diagnosis of Vein of Galen aneurysm confirming the ultrasound findings and to helps to identify prognostically crucial secondary complications (Fig.
7).
Congenital cytomegalovirus (CMV) infection is the most common intrauterine infection.
Early detection of cerebral lesions is especially crucial in many countries where pregnancy termination is possible only before 24 weeks of gestation.
It is widely accepted that fetal magnetic resonance (MR) imaging is complementary to ultrasonography (US) in the evaluation of central nervous system anomalies [5].MR imaging features include cortical malformations,
white matter lesions,
cerebellar hypoplasia,
and temporal lobe lesions [6].
Ventricular dilatation,
intraventricular septa,
ependymal cysts,
calcifications,
microcephaly,
and microencephaly represent nonspecific findings [7] (Fig.
8).
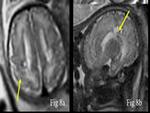
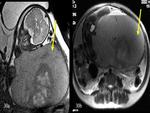
Tuberous sclerosis complex (TSC) is an autosomal dominant disorder in which benign hamartomas develop in multiple organ systems.
MRI is a valuable tool in making the diagnosis of congenital tuberous sclerosis (Fig.
9).
Subependymal nodules and cortical tubers,
while not the most common presenting sign,
are a very frequent finding in infants receiving a Tuberous sclerosis diagnosis (93% and 88%,
respectively).
Chen et al.
concluded that fetal MRI can discover such lesions even when they are not apparent on a detailed sonography [8].
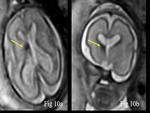
Ventriculomegaly with parenchymal hemorrhage –.
Ventriculomegaly is defined as an atrial width greater than 10 mm measured at the posterior margin of the glomus of the choroid plexus on an axial plane through the thalami [3].
Fetal ventriculomegaly can be detected and classified according to its severity depending on the lateral ventricular diameter.
Our case has associated parenchymal hemorrhage  (Fig.
10).
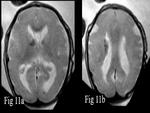
Parenchymal hemorrhage of the abortus is demonstrated (Fig.
11).
(Fig.
10).
Parenchymal hemorrhage of the abortus is demonstrated (Fig.
11).
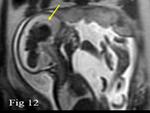
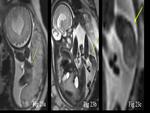
Intracranial hemorrhage – Fetal Intracranial hemorrhage can lead to antenatal fetal brain damage and stroke.
Axial,
coronal and sagittal planes is used to classify and characterize intracranial hemorrhage in respect to location,
size,
appearance,
presence or absence of ventriculomegaly and presence of intraventricular or parenchymal hyperechogenic clots (Fig.
12).
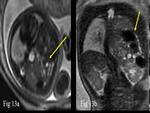
MRI has that advantage over ultrasound to differentiate liver and bowel loops from lung tissue hence and advantage in diagnosing Congenital diaphragmatic hernia [2].
Congenital diaphragmatic hernia (CDH) occurs more often in the posterior aspect of the left hemi-diaphragm,
MRI allows accurate demonstration of the site and contents of hernia either liver or meconium-filled herniated bowel loops (Fig.
13).
Congenital cystic adenomatoid malformation - Congenital cystic adenomatoid malformation (CCAM) is one of the common congenital lung anomaly,
lesions are microcystic or macrocystic.
It may consist of few large cysts (type I) or multiple smaller to moderate sized cysts (type II) showing increased signal on T2-weighted image in either lung.
Microcystic CCAM (type III) typically demonstrates homogeneous moderately high signal intensity on T2-weighted images that can indistinguishable from bronchopulmonary sequestration if feeding artery is not visible arising from the aorta in sequestration (Fig.
14).
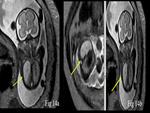
With regards to Spine abnormalities it is interesting that the entire length of fetal spine can be studied in details using multiple MRI parameters which is very important in Neural tube defects such as Iniencephaly [1].
Iniencephaly is a rare neural tube defect characterized by fixed retroflexion of the fetal head,
partial or complete absence of cervico-thoracic vertebrae and occipital bone defect.
Although diagnosed on ultrasound,
the details of the fetal brain and spinal cord can be better determined on MR imaging (Fig.
15).
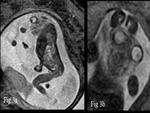
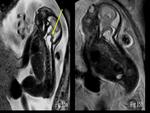
Diastematomyelia is characterized by longitudinal splitting of the spinal cord resulting in two hemicords.
It is classified on the basis of presence of common or separate dural sac and on the basis of presence of a dividing septum.
MRI aids in demonstrating the septum which are of two types,
an osseocartilaginous septum which is more difficult to treat surgically and the fibrocartilaginous septum which has a better outcome.
The bony or fibrous septum is typically detected on an axial or coronal image image as an hypointense band.
It may be an isolated finding or associated with myelomeningocele,
meningocele,
lipoma,
neurenteric cyst,
and dermal sinus which can also be meticulously identified.
It is most commonly encountered at the lumbar or thoracic level (Fig.
16).
Ultrasound is the mainstay in evaluating Neural tube defects,
it however has its limitations.
With advancements in intrauterine therapy of meningomyelocele,
so is the need of more accurate and reliable imaging.
Fetal MRI is an effective,
noninvasive method of assessing CNS abnormalities.
Open neural tube defects are commonly associated with Chiari II malformations,
hence entire central nervous system should be scanned.
Absence of Chiari II should raise suspicion for a closed spinal dysraphism such as a lipomyelomeningocele or terminal myelocystocele [9].
In our case,
there open neural tube defect in the lower lumbar spine with absence of skin and posterior elements with low lying spinal cord suggestive of Myelomeningocele with hydrocephalus (Fig.
17).
In Abdominal Imaging,
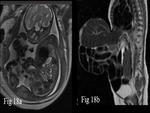
Detecting Omphalocele on prenatal sonography in the second or third trimester has varying rates of success (66–93%) [10,11].
Precise anatomic information can be obtained on MRI.
MRI of fetus with omphalocele shows a central abdominal wall defect,
with abdominal viscera herniating into a thin-walled sac separate from the surrounding amniotic fluid [12].
(Fig.
18).
Genitourinary tract
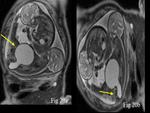
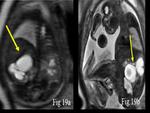
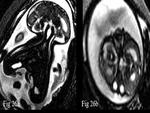
In renal anomalies hydonephrosis appear hyperintense on T2 weighted images.
It is seen commonly seen in congenital Pelviureteric junction obstruction (Fig.
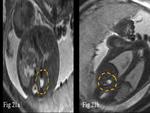
19) MRI can help to add information to different urinary tract anomalies such as posterior urethral valve (Fig.
20) and renal agenesis (Fig.
21).
Musculoskeletal -Additionally musculoskeletal conditions such as club foot,
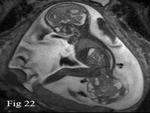
complete phocomelia and tumors like sacrococcygeal teratoma.
MRI characterizes Sacrococcygeal tumors more accurately than ultrasound determining its intrapelvic and abdominal extent (Fig.
22).
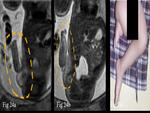
The sagittal plane of MRI is useful in evaluating Club foot and also associated abnormalities can be detected.
MRI enables differentiation between isolated and complex talipes equinovarus (Fig.
23).
Phocomelia is the congenital malformation of fetal hands and feet characterized by shortened or absent arms or legs (Fig.
24).
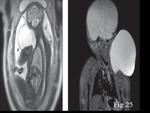
Cystic Hygroma- Also known as cystic lymphangioma occurs in the cervico-facial region commonly in the neck.
MRI can easily detect cystic structures which appear hyperintense on T2 weighted images (Fig.
25).
Multifetal pregnancy - Twin pregnancies have comparatively higher morbidity and mortality risk than singleton pregnancies.
Monochorionic twins (monozygotic twins contained in a single chorionic membrane) can have several complications that may be indications for fetal intervention,
including twin–twin transfusion syndrome,
twin-embolization syndrome,
acardiac syndrome,
and conjoined twinning [3].
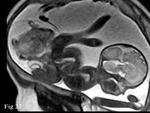
These complications of multifetal pregnancies such as Conjoined twins (Fig.
26) like Ischiophagus (Fig.
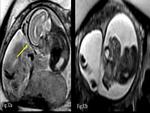
27) and Acardia twin monster (Fig.
28) and others are well demonstrated on MRI which delineates the entire extent of the condition and associated anomalies.
Twin reversed arterial perfusion (TRAP) is a rare complication where one twin is structurally normal while the other is abnormal twin also referred as Acardiac monster twin receives its blood supply from normal or the pump twin and puts the normal fetus at risk from high output cardiac failure.
With the advent of prenatal diagnosis of the acardiac twin's circulation,
it became possible to save the pump twin.
Other than Fetus: Evaluation of Placenta,
Umbilical cord and Amniotic sac is a part of fetal MR examination.
Placenta appears moderately hyperintense on T2-weighted images.
In later gestation placenta shows increase in T2 signal intensity and lobules.
Multiplanar MR imaging aids in precise examination of placenta including its insertion and tumors.
[1]
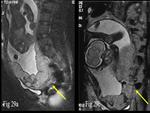
Placenta previa – Abnormal position on the placenta lying in the lower uterine segment and completely covering the internal os (Fig.
29).
In addition to second trimester bleeding and post partum hemorrhage,
pregnancies with a placenta previa have an increased risk of pathologic presentation,
placenta abruptio and placenta accreta,
congenital malformations and perinatal mortality.
There are 4 types,
Complete,
Incomplete,
Marginal and Low-lying.
Chorioangioma with placental bleed – Chorioangioma is the most common benign placental vascular tumor and frequent incidental finding in antenatal scans.
Follow-up monitoring is recommended for size,
development of  polyhydramnios or even
polyhydramnios or even  hydrops fetalis.
There is a heterogeneous mass located at umbilical cord insertion bulging into amniotic cavity (Fig.
30).
hydrops fetalis.
There is a heterogeneous mass located at umbilical cord insertion bulging into amniotic cavity (Fig.
30).
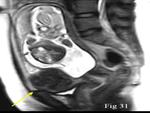
Uterine fibroid in gravid uterus – Fibroid is benign uterine neoplasm,
the growth accelerates during pregnancy,
hence it is important to localize it and determine its growth.
Non-degenerated fibroids appear low in signal intensity on T1 and T2 weighted images.
In our case,
a well-defined hypointense fibroid is seen in the lower uterine segment (Fig.
31).
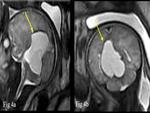
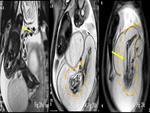
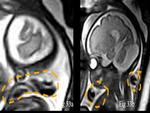
Amniotic band – Linear hypointense (arrow) amniotic band,
entrapment of fetal body part can lead to amniotic band syndrome (Fig.
32).
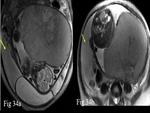
Cord around the neck – When one or more loops of umbilical cord are wrapped around the fetal neck.
It is essential to identify this,
it can lead to arterial compromise and serious complications.
In our case two loops of umbilical cord tightly wrapped around the fetal neck (Fig.
33).
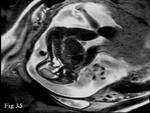
Maternal ascites - Abdominal free fluid can be easily detected on MRI with low signal on T1 weighted and high signal on T2 weighted images.
It can be due to multiple causes in normal pregnancy.
MRI is a safe and accurate modality to demonstrate the cause (Fig.
34).