1.
INDICATIONS
SNRB is performed in the context of lumbosacral radicular pain (defined as pain radiating to one or more lumbar or sacral dermatomes caused by nerve root compression and/or inflammation).
The indications can be grouped as follows:
a) Diagnostic intent:
In patients with no imaging evidence of disease but where the symptoms relate to a nerve root level,
or those with multiple abnormal imaging findings such that confirming the origin of symptoms is difficult from imaging alone.[1] In our institution,
levobupivacaine is used for blocks performed with diagnostic intent.
b) Therapeutic intent:
Patients with proven disc herniation can be offered pain relief and may thus even avoid surgery as the majority of disc herniations resolve spontaneously.
As the pain is believed to result from peri-radicular inflammation and not directly from impingement of nerve by the herniating disc,
steroid injections can reduce inflammation and pain in many patients.
Lumbosacral SNRBs may also be offered post discectomy,
where scar tissue tethers the nerve causing chronic radicular pain.[1,2] In our institution,
a combination of levobupivacaine and the long acting steroid triamcinolone acetonide is used for blocks performed with therapeutic intent.
2.
CONTRAINDICATIONS

Fig. 1
References: Department of Radiology, South Devon District Hospital 2018.
3.
EVIDENCE BASE
While lumbosacral SNRBs are now a common outpatient procedure,
our knowledge of the procedure’s efficacy is largely anecdotal.
There is a paucity of data in the literature and variations exist in both criteria for the diagnosis of lumbar radicular pain and in procedural technique.
Datta et al report limited evidence for the accuracy of selective nerve root injections as a diagnostic tool for lumbosacral disorders,
especially for preoperative evaluation of patients with negative or inconclusive imaging studies in their review of literature from 1966-2012.[3] Other studies have reported variably on the diagnostic role of lumbosacral SNRBs.
There is however stronger support for their therapeutic usage,
with most studies reporting an average pain relief period of 1-3 months in patients who show initial response to treatment.
Riew et al conducted a study on patients with radiographic evidence of nerve root compression who had initially accepted surgical management,
whereby patients were randomised to receive SNRB with either local anaesthetic alone or local anaesthetic and steroid.
Of the steroid-treated group,
71% of patients reported sufficient symptom control that they subsequently declined surgery at 1 year follow up,
and a similar percentage at 5 year follow up.[4] Cyteval et al describe greater therapeutic relief with steroid injection in patients with acute rather than chronic lumbosacral radiculopathy.[5] Kanayama et al followed up 641 patients over nearly two years to ascertain types of degenerative lumbar pathologies that respond well to nerve root injection.[6] They report 51.7 % of patients with degenerative lumbar pathologies were successfully treated by peri-radicular injection obviating need for surgery; factors associated with limited efficacy were herniated disc with spinal stenosis,
foraminal disc herniation,
recurrent disc herniation,
and failed back surgery with instability.
4.
EQUIPMENT

Fig. 2
References: Department of Radiology, South Devon District Hospital 2018.
5.
ANATOMY

Fig. 3
References: Department of Radiology, South Devon District Hospital 2018.
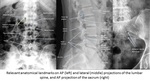
Traditionally practitioners refer to a ‘safe triangle’ when describing bone landmarks used for transforaminal injections.
On an oblique projection,
the triangle is an imaginary area formed cranially by the pedicle and transverse process,
laterally by a line connecting the lateral edges of the superior and inferior pedicle and inferomedially by the spinal nerve root,
which serves as the tangential base of the triangle.
The safety of the ‘safe triangle' has been challenged in recent years as the radiculomedullary artery,
a branch of the anterior spinal artery,
often runs within it.[8–10]
6.
COMPLICATIONS
Common complications
- Haematoma
- Allergic reaction
- Pain
- Nerve injury
- Vasovagal reaction
- Non-response to injection
- Infection
Rare Complications
Spinal cord infarction following high lumbar nerve root block is one of the rarest yet most devastating complications that may follow inadvertent vascular penetration.
Practice of spot film with contrast check for needle position is therefore strongly advocated.
7.
PRE-PROCEDURE
Lumbar or sacral SNRB is performed as an outpatient procedure without premedication.
Prior to performing procedure,
ensure:
- Patient’s previous imaging has been reviewed.
- Check request card for indication and side of symptoms.
- Check INR,
PT,
APTT for patients with coagulopathy.
- Discuss procedure with patient,
checking for contraindications and obtain informed consent.
8.
TECHNIQUE
Whilst there are a variety of different recognised techniques used by different operators,
we will concentrate on one approach for lumbar and one approach for sacral injections in this article.
Lumbar injection set up:
- The patient is positioned lying semi-oblique,
with the patient looking down and away from the operator with the symptomatic side upwards (Figure 4).

Fig. 4
References: Department of Radiology, South Devon District Hospital 2018.
- A metal pointer can be used to locate the correct injection site utilising appropriate collimation to reduce patient dose,
prior to highlighting this position with a skin marker pen.
- An initial AP view with a high enough collimation to count from the lumbosacral junction to the level of the injection site can be used to mark the craniocaudal injection position,
prior to a more collimated oblique view to calculate how far lateral to the midline the injection point should be.
- The starting point for the oblique view is to have the superior end plate of the target lumbar vertebra to be a flat line on the screen,
with the ipsilateral facet column superimposed midway along this line (giving a ‘scotty dog’ projection) (Figure 5).
- The injection point should be just inferior and just lateral to the pedicle.
- The advantage of imaging directly along the planned needle path with an oblique view is ease of assessment of the needle access.
With L5 injections the operator can see if the iliac crest is obstructing this path at the planning stage,
and angle the fluoroscopy tube more cranial and medial to avoid it before marking the injection site.
- Another advantage is that as the needle is imaged end on during its insertion it should remain as a dot on the screen,
making it easy to see if,
and by how much,
the trajectory needs to be adjusted during its insertion.

Fig. 5
References: Department of Radiology, South Devon District Hospital 2018.
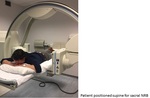
Sacral injection set up:
- The patient is positioned lying prone,
with the symptomatic side closest to the operator (Figure 6).

Fig. 6
References: Department of Radiology, South Devon District Hospital 2018.
- A metal pointer can be used to locate the correct injection site using AP screening,
utilising appropriate collimation to reduce patient dose,
prior to highlighting this position with a skin marker pen.
- S1 injections are like sacral injections at other levels,
though the S1 foramina can be difficult to visualise on fluoroscopy.
This can be overcome by caudally angling and ipsilaterally rotating the C-arm into an obliqued position,
such that the dorsal and ventral foramina of S1 overlap.
The insertion point is level with the lateral edge of the S1 dorsal sacral foramen.
In an optimal position,
on lateral view the needle tip is positioned approximately 5 mm from the floor of the sacral canal.[2]
- The sacral foramina are approached dorsally,
with a slight medial angulation of the needle tract to allow for the angle of the foraminal tunnel.
Procedure
- Having cleaned your hands and donned sterile gloves,
a sterile field is prepared and appropriate medication is drawn up; short acting local anaesthetic for the skin,
contrast to confirm position and long acting local anaesthetic and steroid for the injection.
- The aim is to place the tip of a 22 or 25G needle adjacent to the nerve root as it exits from the foramen,
bearing in mind that the nerve root exits below the pedicle of the vertebral body.
- Short acting local anaesthetic is injected at the site marked as above,
prior to advancing the spinal needle under screening guidance.
- For sacral injections,
the needle tip is angled slightly medially,
and advanced into the foramen.
A lateral view is obtained to confirm that the needle tip has entered the foramen and obtained the necessary depth.
- For lumbar injections,
the needle is advanced in the line of the oblique screening,
aiming for the upper outer quadrant of the foramen.
This position is directly adjacent to the nerve root and dorsal root ganglion.
A lateral view is obtained to confirm that the needle tip has obtained the necessary depth,
and with wider craniocaudal coning to include the needle and the lumbosacral junction can also be used to document that the correct level has been injected.
- The stylet is removed.
Contrast is injected via a connector tube to help keep the operators fingers out of the field of view and reduce movement to the needle tip.
- Contrast is slowly injected,
with warning to the patient to avoid movement and to inform the practitioner of reproduced radicular pain.
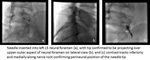
- A spot film confirming perineural and extradural position of needle tip should demonstrate contrast tracking along the nerve inferolaterally.
If the needle has been properly placed,
the contrast medium will flow around the nerve root and may reproduce symptoms of radicular pain.
Contrast should outline the nerve but no vascular or nerve sheath opacification should be demonstrated. (Figure 7)

Fig. 7
References: Department of Radiology, South Devon District Hospital 2018.
- The steroid and long acting local anaesthetic is injected after the correct position is confirmed.
Only a small amount of levobupivacaine 0.25% is injected (approximately 0.5 ml) as larger volumes may falsely affect multiple levels of cord through epidural spread or cause temporary muscle weakness.[2]
- Finally,
the needle is removed,
haemostasis is obtained by applying pressure to site and dressing is applied.
- Patients must be educated of potential complications and informed that pain relief may not be immediate.
They are encouraged to keep a pain diary.