IR provides a minimally invasive alternative for the management of post-surgery complications.
Different interventionist procedures have been introduced to the clinical practice as an efficient way to solve the complications,
often avoiding the need for repeat surgical intervention.
Postoperative complications can be broadly grouped into pulmonary problems,
anastomotic leaks,
and technical,
functional,
or delayed complications (Table 1).
Management of Anastomotic leak: Percutaneous drainage and covered metallic esophageal stents.
Anastomotic leak occur in 10%–44% of postoperative patients and account for as much as 40% of postoperative patient mortality (1).
This complication may occur in the first 10 days after surgery and can be attributed to inappropriate anastomosis tension (either excessive or insufficient).
Insufficient tension leading to poor tissue apposition with extravasation and delayed healing. Excessive tension causes ischemia and necrosis.
Ischemia,
if severe,
can lead to necrosis,
the most feared complication.
According to Lerut classification (Table 2) a leak which is visualized in only one radiographic study of an asymptomatic patient (degree I) require conservative treatment such us antibiotics,
nasogastric tube placement,
and total parenteral nutrition.
A small contained leak with the formation of collections and intraabdominal or intrathoracic abscesses (degree II),
can be managed with a minimally invasive treatment (1,5,6,7).
Once identified,
in most cases it is possible to place a percutaneous drainage guided by image.
In the cases the collection is visible by ultrasound,
this technique is generally preferred due to its availability and easy handling,
because it allows a real time supervision of the drainage placement and because it is a radiation free technique.
When the collection is deeply located and can’t be correctly visualized by ultrasound,
computed tomography (CT) offers a good anatomic and spatial resolution to guide the safe placement of the percutaneous drainage.
The correct location of the needle or drainage catheter can be confirmed by aspiration of a little amount of material.
In addition,
it is also possible to inject a little amount of contrast to identify the presence of unknown fistulas.
Major size leaks with important clinical manifestations (degree III) or necrosis in the duct (degree IV) require an immediate intervention.
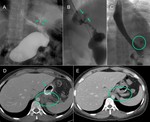
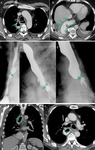
In this clinical setting covered metallic esophageal stents are an effective therapeutic alternative with lower morbidity and mortality compared to conservative treatment and reintervention (2) (Fig.
1,2).
Technical complications: Hemorrhage,
chylothorax,
tracheobronchial lesions,
recurrent laringeal nerve lesion and diaphragmatic hernia are included.
- Management of hemorrhage: Arterial Embolization.
Hemorrhage often occurs because of injury to the spleen,
azygos vein,
intercostal vessels,
right gastric artery,
and lung parenchyma during retraction or dissection (1).
CT is crucial to detect the location of bleeding in hemodynamically stable patients,
and is extremely useful prior to angiography,
as it may avoid it or guide it.
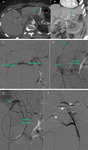
Transcatheter arterial embolization is a safe and effective treatment (Fig.
3).
Once the bleeding spot is identified,
several techniques can be used to stop it and achieve hemostasis.
There are several materials that enable to obtain vascular occlusion,
according to the type of occlusion expected (transient or permanent).
Transient embolization is achieved with absorbable materials,
which allows to restore the blood flow in a variable window of time.
It is main advantage is to avoid the definitive occlusion of the treated vessel.
However,
there is a moderate risk of posterior repeated bleeding once the material has been absorbed.
Permanent embolization is achieved by using non-absorbable materials and inducing a permanent vascular occlusion.
Currently there is no ideal material,
so,
in that way,
the election of the material as well as the embolization technique are crucial to minimize the failure and possible secondary complications,
thus requiring the presence of an interventionist team with high experience and as well as the availability of several materials.
- Management of chylothorax: Thoracic duct embolization (TDE). Chylothorax constitutes a rare complication with an incidence rate of approximately 1-5% (1).
It is defined as the leak of lymphatic fluid (containing lymphocytes,
immunoglobulins and several enzymes) enriched with lipids and chylomicrons,
into the thorax (8).
The mantained loss of chyle diminishes the number of lymphocytes and causes nutritional deficiencies leading to a vulnerable state for systemic infection,
especially if daily chylothorax drainage is superior to 1000 ml.
The conservative treatment is used as the first line therapy,
although the success rate is relatively low.
If chylothorax drainage is higher than 1000 ml per day during more than five consecutive days,
or the leak persists after two weeks of conservative treatment,
or metabolic or nutritional complications are developed,
secondary surgery or direct embolization is required (9,10).
Lymphography (LG) is a useful diagnostic technique to detect the distinct types of lymphatic leaks including chylothorax,
chylous ascytes,
and lymphatic fistulae.
Moreover,
it allows the treatment of the leak through the use of Lipiodol,
a liposoluble contrast that produces a granulomatous reaction during its extravasation and also has embolic properties that help to accumulate in the leak spot (9-11).
There are two methods of LG: pedal LG and intranodal LG.
Conventional pedal LG,
which involves the isolation and cannulation of pedal lymphatic vessels and injection of Lipiodol,
is time-consuming and requires an incision to expose the pedal lymphatics.
Intranodal LG relies on ultrasound-guidance to access inguinal lymph nodes for direct lymph node access and injection of Lipiodol.
Accessing the inguinal lymph nodes requires no incisions and bypasses the lower extremities,
thus decreasing the procedure time for LG and TDE,
radiation dose,
and volume of the contrast medium (9).
For the treatment of chylothorax,
percutaneous thoracic duct embolization (TDE) is an established alternative to surgical ligation of the thoracic duct.
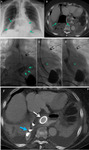
It is a minimally invasive procedure where opacification of the lymphatic system with lymphangiography technique is followed by thoracic duct catheterization and subsequent occlusion (Fig.
4) (9,10).
Once the retroperitoneal lymphatics along the upper lumbar region and cisterna chyli are opacified with Lipiodol,
percutaneous cannulation of cisterna chyli is performed using 22-G Chiba needle (15 or 20 cm).
Once the cisterna chyli or large lymphatic duct is accessed with a needle,
a 0.018 or 0.014 inch microwire is used to thread the thoracic duct,
followed by contrast administration to confirm the location and verify extravasation and leak.
Then,
embolization of distal and proximal portions of the thoracic duct leak is applied using coils. The proximal portion is reinforced adding glue/ónix to complete the occlusion (9,10).
When the thoracic duct is successfully catheterized and embolized,
the success rate for resolution of chylothorax is 90% (9).
In conclusion,
lymphangiography as well as embolization of thoracic duct is a relatively safe and efficient interventionist method.
It allows the identification and the complete occlusion of the leak. Due to its minimally invasive nature and its high efficiency,
surgical re-intervention may be avoided (9,10).
- Management of tracheoesophageal fistulas: covered metallic esophageal stent. Injury to the trachea or mainstem bronchi,
either in a context of intraoperative complication,
secondary to postoperative anastomotic leak or in a patients with advanced cancer,
usually occurs in the membranous portion of the airway (12).
Such injury can lead to fistula formation and resultant respiratory compromise due to recurrent pneumonia,
requiring stent placement or surgical repair.
In a context of the treatment of iatrogenic esophageal perforation fistulas,
various types of covered stents have also been used with excellent results and good short-term quality of life.
In the palliative treatment of patients with advanced esophageal cancer and tracheoesophageal fistulas covered esophageal stents are the treatment of choice.
In these circumstances,
there is a direct beneficial effect on the survival rate of patients,
as if these fistulae are not treated,
they may lead to patient’s death in an average time of three months,
and 85% of them may die due to aspiration neumonia (2,13).
Using fluoroscopic guidance,
it is possible to identify the anastomosis and crossed using standard guidewire and catheter technique.
The placement of covered devices enables the successful treatment of tracheobronchial fistulae (2,13).
Late complications. These late complications are generally anastomosis stenosis or recurrent disease,
being dysphagia the most common symptom.
Additional complications,
which have been discussed previously,
such as leaks and fistulae,
can also develop in the late post-surgery time (1).
- Anastomotic stricture: Balloon dilation and stent placement. Anastomotic stricture and consequent dysphagia has long been treated with surgical and endoscopic interventions.
However,
crossing tight esophageal strictures and positioning metallic stents are sometimes difficult without fluoroscopic guidance and appropriate catheter technology.
Radiologist,
who are already accustomed to using similar materials and techniques,
are in the perfect position to perform these treatments.
Balloon dilation is usually indicated for benign stenoses and is technically successful in more than 90% of cases. The use of stents in benign lesions is plagued by a high long-term complication rate and leads to tissue hyperplasia with recurrent esophageal stenosis.
However,
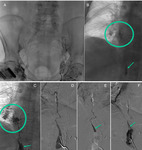
good results have been reported in benign lesions with retrievable stents that are left in the esophagus for a few months (13) (Fig.
5).
Anastomotic stricture in the early postoperative period is due wound healing,
and the prevalence increases if there is an anastomotic leak.
Patients who develop anastomotic stricture in the late postoperative period should be careful evaluated for recurrent disease with endoscopy and CT.
Balloon dilatation has the advantage of producing less incidence of perforation because it is performed under fluoroscopic guide,
and leads to the successful treatment of surgical stenosis.
The first step is to perform an esophagogram and identify the stenosis level.
Then,
a guide is placed orally,
passing through the stenotic zone.
This is followed by the introduction of the balloon,
which is the inflated.
Ballon dilation provides relief in the majority of patients,
thus relieving dysphagia.
In a context of advanced esophageal carcinoma and malignant dysphagia,
the main focus of treatment is palliative.
Esophageal stent placement,
is the primary treatment for malignant dysphagia in patients with poor functional status who cannot tolerate radiation therapy or chemotherapy,
who have advanced metastatic disease,
or in whom previous therapy has failed (13).