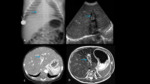
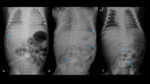
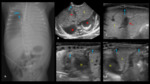
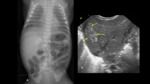
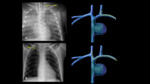
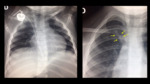
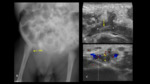
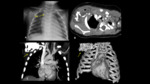
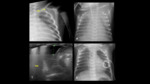
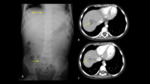
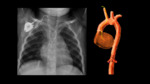
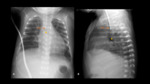
TUBES AND CATHETERS IN PEDIATRICS
The following are the most commonly used devices in pediatrics:
- Umbilical arterial catheter (UAC)
- Umbilical venous catheter (UVC)
- Central venous catheter (CVC)
- Endotracheal tube (ETT)
- Nasogastric tube (NGT)
After placing each device,
the correct positioning must be checked to avoid any complications,
and this is usually made with x-ray,
although it can also be determined sonographically or by other imaging tests,
especially if a complication is suspected.
In the case of vascular catheters,
we have to assess:
⇒ If they have been excessively entered:
- In this case you must move the distance that is considered necessary until its correct position
⇒ If they are too far out:
- In these circumstances,
part of the catheter cannot be reintroduced because the exterior part is not sterile and there is a risk of infectious complications.
- Replace the malpositioned catheter.
Umbilical Artery Catheter (UAC)
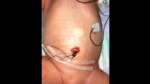
Introduction:
- Catheterization of the umbilical artery is a common procedure in the neonatal intensive care unit.
The umbilical artery can be used as an arterial access during the first 5-7 days of life but rarely beyond 7-10 days since spontaneous thrombosis of the umbilical vessels occurs after one week.
Indications:
- Invasive monitoring of blood pressure.
- Arterial blood gas.
- Blood sampling.
- Exchange transfusion
- Infusion of fluids / intravenous medication / etc.
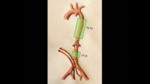
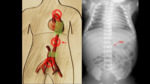
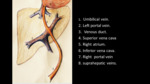
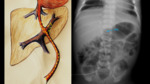
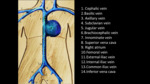
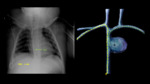
Anatomical path of UAC (Fig. 3 ):
- Enters through the umbilicus in one of the umbilical arteries (there are two umbilical arteries).
- The umbilical artery typically follows a posterior and caudal course to reach the internal iliac artery.
- It then continues upwards from the internal iliac artery to the common iliac artery and posteriorly to the aorta.
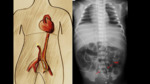
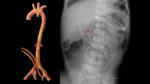
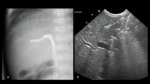
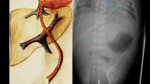
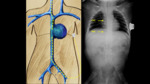
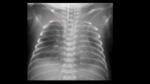
Radiological assessment (Fig. 4):
- To determine its correct positioning,
abdominal or thoracoabdominal AP X-ray is performed depending on the probable location of the end of the catheter and in doubt,
a lateral projection is also used.
- On the X-ray,
we will observe that the catheter initially goes downwards to reach the internal iliac artery and then ascends through the aorta parallel and anterior to the vertebral bodies,
slightly to the left of the spine.
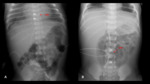
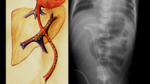
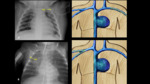
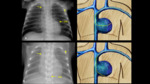
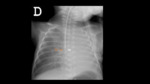
Correct locations (Fig. 5 and Fig. 6):
⇒High:
- At T6-T9 level.
- This is the most recommended as it is only associated with minor complications.
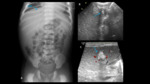
⇒ Low:
Malpositions:
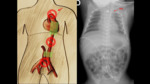
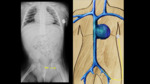
⇒ excessively high / cranial at T6:
- May be responsible for cardiovascular complications if placed in the cardiac chambers
- Risk of injury of the ductus arteriosus or supra-aortic trunks (Fig. 7).
⇒T12-L3:
- Risk of injury of the abdominal visceral trunks (Fig. 8 and Fig. 9),
whose usual origin is:
♦T12: celiac trunk
♦ T12-L1: superior mesenteric artery.
♦ L1-L2: renal arteries.
♦L3: inferior mesenteric artery.
⇒Excessively low / below L5:
- Risk of injury of iliac and femoral vessels
⇒ Others:
- Any deviation from the usual path,
or the presence of loops,
indicates malposition and it is necessary to remove the catheter.
- A path that does not follow a vessel could suggest vascular rupture and an intraperitoneal position of the catheter (Fig. 10).
Possible Complications:
- Hemorrhage
- Infection
- Thrombosis: In the case of renal artery thrombosis,
the onset of hypertension due to stenosis / occlusion of the vessel is typical.
- Visceral,
spinal or limb ischemia (Fig. 11).
Umbilical Venous Catheter (UVC)
Introduction:
- The umbilical vein,
like the artery,
can be used as venous access during the first 7-10 days of life because after that it is obliterated.
- This venous route is widely used in neonatology since its canalization is very simple due to the wide caliber and accessibility that contrasts with other veins,
which in neonates and premature infants can be very difficult to channel because they have a very small diameter,
and are fragile,
deep,
etc.
(Fig. 12).
Indications:
- Monitoring of central venous pressure.
- Venous access in very low birth weight preterm infants.
- Parenteral nutrition,
intravenous medication and fluid therapy.
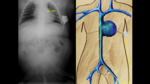
Normal UVC path
- The catheter enters through the umbilicus into the umbilical vein
- The umbilical vein ascends to the liver until reaching the left portal vein,
continues in the venous duct and from there it passes to the IVC at the confluence of the suprahepatic veins (Fig. 13 ).
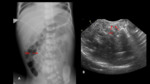
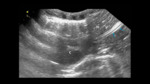
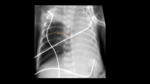
Radiological evaluation:
- Abdomen AP / thorax-abdomen AP X-rays are performed and,
if in doubt,
a lateral projection is made.
The position of the catheter can also be assessed by ultrasound (Fig. 14 ).
- In the radiological study,
we should see an ascending path towards the liver.
In the lateral projection,
we will see how the catheter crosses the liver at the anterior level (Fig. 15 ).
- Normally portal gas can be identified after inserting the catheter with both ultrasound and radiographs (Fig. 16 ).
This pneumatosis is transient,
self-limiting and should not be confused with other etiologies (necrotizing enterocolitis,
etc.).
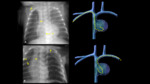
Correct locations (Fig. 17):
⇒High:
- The tip of the catheter should be above the diaphragm without reaching the heart,
ie.
at the level of the inferior vena cava,
approximately between T8 and T9.
⇒Low:
- Below the hepatic border between L1-L2 (“free-flowing" catheter).
Incorrect Locations:
⇒Excessively high
- If the catheter is placed in the cardiac chambers or in the pulmonary veins it can produce cardiovascular and thrombotic complications (Fig. 18).
⇒Intrahepatic
- There is an increased risk of intrahepatic complications of thrombotic,
ischemic type,
etc.
(Fig. 19 ).
⇒We should not observe loops or deviations from the normal path,
especially if they are not following the path of any vessel (Fig. 20 ,
Fig. 21 , Fig. 22).
Possible Complications:
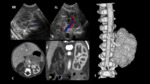
⇒Venous thrombosis (Fig. 23 and Fig. 24 ).
- This complication can occur even if the catheter is well positioned,
with thrombus formation being common throughout the catheter,
especially if there are loops.Ultrasonography is the technique of choice for the diagnosis of venous thrombosis,
although complementary studies can be performed by CT or MRI.
⇒Tearing of the umbilical vein
- This should be suspected if the UVC does not follow a vascular path,
suggesting vascular rupture and passage of the catheter into the thoracic cavity and abdominal cavity (Fig. 25 and Fig. 26 ).
⇒Hematoma / collection / hepatic infarction
- Due to rupture of the vascular wall by the catheter,
which causes bleeding and extravasation to the parenchyma of the infused liquids.
A liver collection / lesion can be seen echographically,
and the appearance of the lesion may be variable (Fig. 27 ).
⇒Cardiac perforation.
Central venous catheter (CVC)
Introduction:
- These are intravenous catheters that are placed in a central vein.
- Unlike UAC and UVC,
these catheters may be implanted for a long time.
In addition,
they will theoretically have a lower incidence of complications due to the greater caliber of the vessel.
- The following are amongst the most-commonly used in pediatrics:
♦ The PICC (peripheral central venous catheter).
♦ The Hickmann catheter (tunneled catheter).
♦ Port-a-cath (reservoir catheter).(PAC)
Indications:
- Measuring central venous pressure.
- Administration of parenteral nutrition and medication.
- Hemodialysis / plasmapheresis.
- Poor peripheral venous access.
Correct locations (Fig. 28 and Fig. 29 ):
- The location of the catheter depends on the access route:
- Upper limb veins or jugular vein: the tip of the catheter should be located in SVC or SVC-RA junction.
- Lower limb veins: The tip of the catheter should be placed in IVC adjacent to the entrance into the RA.
Incorrect location:
⇒Excessively short (Fig. 30 and Fig. 31).
- Catheter tip located in the peripheral veins of the upper or lower limbs,
which represents a greater risk of local vascular complication (thrombosis,
phlebitis by drugs,
etc.)
⇒ Excessively long (Fig. 32 ,
Fig. 33 , Fig. 34)
- Catheter tip located in cardiac cavities or passing through it
⇒Others:
Possible Complications
Endotracheal tube (ETT)
Introduction:
- These devices are used to keep the airway permeable and properly ventilate the patient.
Indications:
- Respiratory insufficiency.
- Airway obstruction.
- Surfactant administration.
- Aspiration of secretions.
Correct location
- Firstly,
it should be noted that head movements,
especially flexo-extension movements,
cause important changes in the position of the tube.
Thus,
the extension will cause removal and vice versa.
This is why the tube should be kept in an intermediate position at the level of the trachea.
- ETT distal end should be located:
♦ distal to vocal chords (C5-C6 level).
♦ proximal to the carina (usually located between T5-T7).
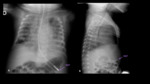
Radiological evaluation:
- This is performed by the AP Chest X-Ray,
which should include the mandible.
- It is considered well positioned when the end of the ETT is located between T3-T4 with the head in a neutral position.
It will be acceptable when placed between C7 and a vertebral body above the carina (Fig. 44 ).
Incorrect Locations
⇒High position (Fig. 45 ):
- Risk of desaturation,
extubation,
etc.
⇒Low position:
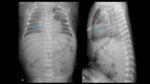
- Risk of selective intubation:
- The right main bronchus is the most common and causes the left lung to collapse (Fig. 46 ).
- The Intermediate bronchi can also be selectively intubated,
which leads to atelectasis of right superior lobe and the left lung (Fig. 47).
⇒Malposition:
- Esophagus,
mediastinum,
etc .
Possible Complications
- Atelectasis:This is the most common complication from selective intubation.
- Barotrauma.
- Tracheal perforation.
- Tracheal stenosis:Prolonged use of ETT is associated with subglottic tracheal stenosis,
caused by chronic mucosal irritation.
On the frontal Neck X-ray it may be seen as a focal narrowing of the trachea.
Nasogastric tube (NGT)
Introduction:
- The gastric tube is usually inserted through the nose: naso-gastric tube (NGT),
except for suspected skull base fracture,
etc.,
when the tube is inserted into the stomach through the mouth: Oro-gastric tube (OGT).
Indications:
- Feeding and aspiration of secretions.
- Decompression of the stomach in patients with abdominal pathologies: intestinal obstruction,
necrotizing enterocolitis,
etc.
Correct location
- The distal end should be located in the gastric chamber.
- Radiological assessment:
- This is assessed by an AP Chest-abdominal X-Ray,
and in doubt with a lateral projection.
- In the AP,
we must identify the end of the probe in the left hypochondrium.
In the lateral projection,
the tip will be placed at the anterior level (Fig. 48).
Incorrect location:
⇒High:
- if the catheter is placed proximal to the gastro-oesophageal sphincter (ie.
in the esophagus) there is a risk of gastroesophageal reflux and bronchoaspiration.
- this may happen because it is short and / or because it loops back into the esophagus (Fig. 49).
⇒Low:
- If the probe passes into the duodenum the tube cannot effectively aspirate the stomach and its secretions (Fig. 50).
⇒Abnormal loops and paths
- If the probe is deviated,
you should suspect: - Congenital anomalies: Diaphragmatic hernia,
tracheoesophageal atresia (Fig. 51).
Complications
- Bronchoaspiration.
- Gastric or esophageal perforation.