The diagnosis of CP is based on symptoms,
morphological changes on imaging tests and / or functional tests which demonstrate exocrine pancreatic insufficiency.
Morphological changes are detected with greater sensitivity by echoendoscopy.
However,
the invasive nature of this procedure and its limitations to evaluate complications related to the disease,
explain the need of alternative diagnostic tools.
In this scenario,
both CT and MRI as well as transabdominal ultrasound play an important role.
Imaging for Chronic Pancreatitis
Transabdominal Ultrasound has been used for many years to evaluate the pancreas.
However,
the diagnosis of CP can be difficult.
The limitation of ultrasound is its inability to evaluate the complete pancreas due to patient body habitus and overlying bowel gas.
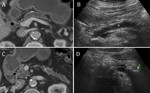
Late findings include alterations in size and echogenicity of the gland,
pancreatic calcifications,
pancreatic duct dilatation and irregularity,
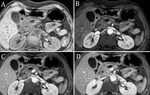
and biliary dilatation (Fig 1).
Computed tomography (CT) is considered the best initial imaging test in the workup for CP.
There are three findings classically seen on CT in CP,
including a dilated pancreatic duct (68%),
pancreatic atrophy (54%),
and pancreatic calcifications (50%) (Fig 1). Note that normal pancreatic morphology may also be observed on CT imaging in CP,
making the diagnosis particularly difficult in certain population of patients.
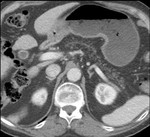
Additionally,
while pancreatic atrophy is visualized in a large proportion of patients with CP,
this is not a specific finding and can also be seen with normal aging (Fig 2).
Advantages of CT scans are that they are widely accessible,
show a detailed view of pancreatic morphology changes seen in CP,
and are especially useful in detecting changes seen in advanced disease.
It can also quickly assess extrapancreatic pathology that may explain various presentations mimicking chronic pancreatitis.
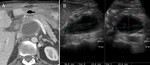
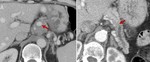
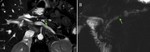
Another advantage of CT is its ability to detect various complications of acute and chronic pancreatitis such as pseudocysts,
biliary or duodenal obstruction,
venous thrombosis,
pseudoaneurysms,
and pancreaticopleural fistulas (Fig 3,4).
While changes in pancreatic parenchyma in late CP are visualized,
CT fails to visualize classic changes seen within the pancreatic ducts,
thus making it unreliable to diagnose early CP.
Magnetic resonance cholangiopancreatograph (MRCP) and secretin-enhanced MRCP (sMRCP) are both sensitive and specific for characteristic changes seen in CP.
Specific advantages of MRCP evaluation in CP are better visualization of both the pancreatic parenchyma and ducts. The normal pancreas is isointense or slightly hyperintense to the liver on T1-weighted non-fat-suppression images.
With fat suppression,
the normal pancreas is best displayed as hyperintense to all other solid organs of the abdomen. The main advantage of MRI compared to imaging modalities is the sensitivity of MR in depicting signal intensity and enhancement abnormalities in early chronic pancreatitis.
Due to its excellent soft-tissue contrast,
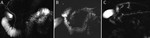
MRI can depict early disease by detecting signal changes before any morphologic changes occur (Fig 5).
Parenchymal changes that are visualized via MRI include pancreatic atrophy,
depressed T1 signal,
irregular contour of head or body,
heterogeneous parenchyma,
and delayed gadolinium enhancement of the pancreas after administration (Fig 5).
Ductal changes include intraductal filling defects often indicative of calculi,
main pancreatic duct dilation,
side branch dilation,
irregular duct contour,
and decreased compliance after administration of secretin (Fig 6).
Secretin-enhanced MRCP allows for a noninvasive approach to evaluate for pancreatic exocrine function. Secretin stimulates the pancreas to secrete fluid and bicarbonate and increase the tone of the sphincter of Oddi and therefore improves visualization and delineation of the main pancreatic duct and its branches.
In addition,
secretin can also be useful for functional evaluation of exocrine pancreas based on quantification of duodenal filling with chronic pancreatitis showing decreased filling (Fig 7).
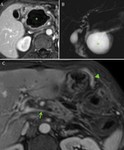
MR imaging is also an excellent modality in the evaluation of potential complications of chronic pancreatitis.
MR has a high sensitivity for the detection of pseudocysts and the characterization of their contents better than CT (Fig 8).
MRCP also can show communication with the pancreatic duct,
which may guide therapy.
MRI also can evaluate vascular complications including splenic artery pseudoaneurysmsm and splenic or portal vein thrombosis (Fig 8).
Potential biliary complications like choledocholithiasis,
fistulas,
and dilatation and transient obstruction of the common bile duct due to inflammatory strictures can also be evaluated by MRCP.
Negatives associated with these modalities include limited access to MR time.
Endoscopic Ultrasound (EUS). As discussed earlier,
the diagnosis of chronic pancreatitis is typically not in doubt in those individuals with severe disease,
as they will have classic symptoms,
risk factors and usually pathologic imaging features on CT or MRCP.
In early CP,
the diagnosis may be confused with other disease entities.
It is in this subset of patients where EUS has the most potential to assist in diagnosis,
as it is rarely needed for diagnostic purposes in advanced CP.
However,
there are important limitations including only fair interobserver agreement and low specificity of some findings.
Considering the large number of potential explanations for EUS abnormalities of the pancreas,
this test should not be used in isolation to establish a clinical diagnosis of CP.
Endoscopic retrograde cholangiopancreatography (ERCP) is a modality seldom used for diagnosis of CP at the present time.
It allows for a detailed pancreatogram,
which can show some changes related to chronic fibrosis and atrophy.
However,
following the advent of CT,
MRCP,
and EUS,
its use is typically limited to therapeutic interventions rather than purely diagnostic.