Of the 858 MRIs performed in 788 patients over the 2-year period,
23 were performed post-operatively,
within 4 months of the original surgery.
Complete data was available in 22 patients.
On review of the postoperative MRI cases,
none of these patients had pre-operative MRI imaging.
The average age of the patients was 59,
with 12 screening and 10 symptomatic cases.
In 5 cases (21%),
abnormal enhancement was identified in the ipsilateral breast,
distant from the surgical cavity. 4 biopsies were performed following MRI,
3 US and 1 MRI biopsy (1 benign,
1 DCIS,
1 LCIS and 1 IDC) and the fifth proceeded directly to mastectomy.
Each of these cases is reviewed in detail below.
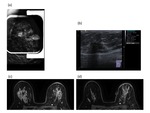
In case 1 the patient was recalled from screening for 23mm of linear branching calcifications in the central right breast (Figure 1 a,
b).
Stereotactic biopsy confirmed high grade ductal carcinoma insitu (DCIS).
Histology of the wide local excision showed grade 2,
invasive carcinoma with mixed ductal and lobular features,
high grade DCIS,
and a whole tumour size 42mm,
with involvement of margins. A postoperative breast MRI was performed to assess for further disease in the breast. In addition to postoperative change at least two further suspicious areas of enhancement were seen inferior and more posterior to the index lesion.
At the level of the nipple,
deep within the breast an irregular avidly enhancing lesion was seen measuring 14 x 10 x 6mm (Figure 1 c). Below the level of the nipple centrally,
a rim-enhancing lesion was seen,
measuring 9 x 7 x 9 mm and demonstrating a type I/II curve (Figure 1d).
Based on the MRI findings a mastectomy was subsequently performed,
which confirmed a further 7mm focus of invasive cancer and 9mm of DCIS.
Both of these areas were deemed to be distant from the original tumour in the wide local excision based on the final histological assessment.
In case 2 the patient presented with a symptomatic lump in the left breast.
The palpable area of concern was a well-defined benign appearing mass,
which was biopsy proven as a fibroadenoma.
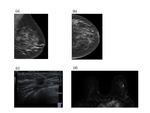
On mammogram an incidental spiculate mass was noted in the upper inner left breast (Figure 2a). US showed an ill-defined hyoechoic mass with irregular margins (Figure 2b).
Biopsy revealed an invasive carcinoma,
NST; grade 2,
ER positive,
HER2 negative.
Histology of wide local excision specimen showed tumour involvement of medial margins.
A postoperative MRI was performed to assess for distant disease.
In addition to postsurgical change,
two further abnormal enhancing lesions were identified in the upper inner aspect of the left breast adjacent to the chest wall (Figure 2 c,
d).
Second look US showed a subtle area of altered echogenicity in the upper inner left breast but no focal mass,
which was biopsied and returned as normal tissue,
B1.
Re-excision of margins demonstrated the tumour to be completely excised.
In case 3 the patient underwent a PET CT to evaluate a right lower lobe pulmonary soft tissue mass.
PET CT showed abnormal FDG uptake in the left axillary tail and the patient was referred to the breast unit for further assessment (Figure 3a). Mammogram showed bilateral breast implants with a 23mm asymmetric density in the left axillary tail (Figure 3b).
US demonstrated an irregular hypoechoic mass 23mm (Figure 3c).
A core biopsy showed invasive carcinoma NST,
grade 2,
ER/PR positive,
HER-2 negative.
Histology of the wide local excision specimen demonstrated residual tumour at the medial margin.
Following MDT discussion an MRI was recommended for detection of further distant disease.
MRI showed multiple foci of type III enhancement in the superior left breast highly suspicious for residual malignancy (Figure 3d). Second look US of the superior left breast was performed which did not demonstrate any obvious abnormality,
but possible subtle architectural distortion.
A fan biopsy was performed.
Histology showed classic lobular carcinoma insitu.
Re-excision of the surgical cavity margins was performed,
with clear margins on histology.
Case 4 was an external referral for further assessment and management of a right breast mass.
Mammogram showed a 35mm spiculate mass in the right upper outer quadrant (Figure 4 a,
b).
On US this appeared smaller measuring up to 19mm (Figure 4 c).
The right axilla was normal.
Histology of the core biopsy of the mass showed a G2 invasive cancer of NST.
A wide local excision was performed and histology showed a 60mm G3 NST with adjacent satellite nodules.
Given the discrepancy in imaging and histology size a postoperative MRI was performed for clarification.
This demonstrated post operative change with 9 mm irregular enhancing mass in the right medial breast at the level of the previous resection,
just above the nipple (Figure 4d).
Second look US showed a 7mm ill-defined mass in the medial right breast corresponding to the enhancing focus on MRI (Figure 4e).
A core biopsy of this lesion was performed and histology showed high grade DCIS with sclerosing adenosis.
The patient went on to have a completion mastectomy,
with the final histology confirming 14mm high grade DCIS but no invasive malignancy.
In the fifth case the patient presented with a lump and skin dimpling in the 3 o’clock position of the left breast.
Tomosynthesis demonstrated an 18mm mass in the lateral left breast which correlated with the clinical abnormality (Figure 5a,
b).
At the site of clinical concern on US there was a hypoechoic solid mass suspicious for malignancy (Figure 5c).
The left axilla was normal.
US guided biopsy showed invasive carcinoma NST,
grade 2; ER/ PR positive and HER2 negative.
Histological review of the wide local excision specimen showed tumour involvement of the superior and medial margins.
Re-excision of margins demonstrated persistent tumour involvement of the margins.
To further evaluate breast MRI was performed.
A 9 mm enhancing nodule was present at the site of surgery,
suspicious for residual disease. A second lesion was seen remote from this in the lower outer quadrant,
measuring 11 mm (Figure 5d).
Both demonstrated type 3 curve with up to 250% enhancement. Second look US was normal and an MRI guided biopsy was performed.
Histology of the MRI guided biopsy of the lesion in the left lower outer breast,
distant from the surgical cavity showed invasive carcinoma NST,
grade 2,
ER positive,
PR weakly positive,
HER negative.
Completion mastectomy showed a 7 mm grade 2 invasive carcinoma NST,
2 mm focus of intermediate grade DCIS and classical LCIS.
In the remaining 17 cases no suspicious lesion was seen on MRI distant from the operative cavity.
2 patients had mastectomies,
either due to extensive pleomorphic LCIS at the resection margins or due to patient choice. 10 cases underwent limited re-excision,
with no further surgery required following this.
5 of the patients had no further surgery performed.