INTRODUCTION
Medical environment has experimented major changes with the introduction of minimally invasive therapies,
where interventional and vascular radiology procedures has becomed essentials in modern medicine.
Many diagnostic and therapeutic new indications have been added to management of disease,
specially in oncology field where treatment of tumoral lesions had experimented great.
Tumor ablation (TA) is an alternative treatment in some types of cancer.
(2)
The meaning of the term “ablation” refers to destruction of material where the objective is to achieve the maximum degree of tumor necrosis,
based on the principle that the reduction in tumor volume or prevention of a new growth may improve prognosis.
These procedures are globally known by the name of TA techniques and refer to the direct application of a treatment within the lesion.
(3)
- Chemical ablation techniques: refers to injection of chemical substances into the tumor,
substances such as acetic acid,
etanol and chemotherapeutic agents
- Thermal ablation techniques: refers to the thermocoagulation methods including laser,
radiofrequency (RF),
microwave (MW) and cryoablation where cold application is used
- Other methods are radioembolization (Y90) and non-thermal irreversible electroporation (NTIRE)
Actually one of the most used technique is TA using RF mostly because of its availability,
however any TA technique offers the possibility to treat a wider variety of tumors and use it alone or in combination with other therapeutic procedures (such as surgery,
portal embolization,
chemoembolization,
etc),
or repeating the procedure as many times as necessary.
Actually MW ablation has gained ground due to a theoretical better usefulness profile (4).
Thermal injury is directly proportional to the temperature reached by the electrode and time of exposure,
on the other hand is inversely proportional to the distance from the electrode (3),
also there is another essential variable that determines ablation results which is the tissue properties of environment.
Both methods,
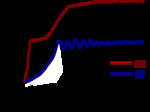
RF and MV relies its effect on thermal injury based on tissue heating up to reach of cytotoxic temperatures (Fig 1),
For successful ablation,
the tissue temperature should be maintained in a range of 50–100ºC to ablate tumour adequately and avoid carbonization around the electrode tip due to excessive heating (5).
The nature of the thermal damage depends on the tissue temperature and the duration of heating (6).
In spite of similar outcomes,
each method has its own mechanisms and quite different physics principles.
PHYSICS PRINCIPLES: RF vs MW
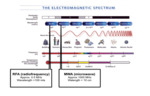
RADIOFREQUENCY ABLATION is based on electrical current in radiofrequency range,
approximately 0.5MHz (400-500kHz) where its wavelength is about >100 meters.
(Fig 2)
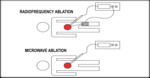
This energy is delivered through needle electrode within the tissue and produces excitement of cellular ions with consequent friction at molecular level that finally increases intracellular temperature and produces thermal cytotoxicity,
coagulation and tissue necrosis (Fig 3).
The active ablation zone is localized just near the electrode but a larger volume of final ablation zone is secondary to thermal conduction (passive diffusion) into more peripheral areas around the electrode.
(Fig 4)
Two primary issues related to heating mechanism have limited the effect of RF ablation.
First,
temperature from 50-60℃ for 4-6minutes causes irreversible cell damage,
60-100º causes tissue coagulation,
but temperatures over 100℃ produces carbonization and charring of tissues (5) that increases the impedance and limits the heat diffusion from the needle to distant zones with subsequent limitation of ablative effect.
Second,
conductive heat transfer in RF depends highly on local tissue environment,
for example,
there is heat dissipation due to blood flow in adjacent vessels areas,
known as “heat-sink” effect,
that results in lower temperatures and lesser ablation effect (Fig 5),
moreover highly aerated tissue like lungs confers poor heat conductivity and high impedance to electric current flow.
Consequently,
the shape and size of the ablation zone in RF,
may be variable and relatively unpredictable depending on tissue environment.
MICROWAVE ABLATION uses non-ionizing electromagnetic waves included in a microwave range,
approximately 1000MHz (900-2540MHz) where its wavelength is about <10 centimeters.
(Fig 2)
This electromagnetic radiation has electric charge which oscillates at a rate determined by its frequency,
it produces dielectric heating,
where dielectric material is the tissue.
The alternating electromagnetic field is applied to an imperfect dielectric material where this electromagnetic field makes oscillate to all water molecules in the tissue (1).
Water is a polar molecule,
and its electric charge is asymmetrical,
the hydrogen is positive whereas oxygen is negative,
this polarity allows that electromagnetic wave can change the water molecule orientation according to the positive or negative field.
(7).
This alternant change in orientation of water molecules movement generates kinetic energy that finally is converted to heat (Fig 3).
In contrast to electric currents,
MW radiate through all biological tissues,
including those with high impedance and the “heat-sink” effect is attenuated by faster heating and higher temperatures,
also electromagnetic field generates homogeneous heating of tissue that results in faster,
larger and more predictable ablation zones (Fig 5).
In MW,
as well as RF,
there is an active ablation zone central and near the antenna and a secondary peripheral ablation zone (bring about by passive diffusion),
that globally are larger in MW (Fig 4).
Each MW system performance can vary widely by combination of different factors like antenna design,
frequency,
time and power generator that finally determine size and shape of the ablation zone.
EQUIPMENT AND ENERGY APPLICATION: RF vs MW
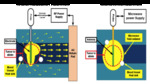
In RFA (Fig 6),
there is an external energy source that provides 50-200W approximately and delivers oscillating current of high frequency by using “monopolar” or “bipolar” modes; in the first one,
a single internal electrode is located at the tumor site,
while a surface electrode (ground pad) completes the electrical closed circuit through the body (6).
In bipolar mode there are two internal electrodes (or multiple) that are localized around the interest zone,
where no closed circuit exists so no ground pad is needed,
this mode provides more effective and focused heating in the área between the electrodes,
but it is less available and more invasive than monopolar.
Generally,
the needles / electrodes has a 14-21G in diameter.
In order to attain larger necrosis volumes,
electrodes with numerous innovative modifications are applied,
such as expandable electrodes (Fig 7),
permanent infused or internally cooled electrodes or multiple needles systems.
The result is larger ablation aereas up to 2-5cm.
In MWA (Fig 6),
there is a energy source that provides 45-60W approximately,
and delivers oscillating current of very high frequency by using an antenna (monopolar electrode) that is introduced into the lesion through an access needle.
Multiple antennas can be used at the same time that allows treatment of multiple lesions concomitantly (Fig 8).
Ground pad are not needed since there is no a closed electrical circuit,
thus,
no burn risk.
Recently there have also developed improvements in material like high-power generators,
antennas with internal cooling or mechanism to prevents the power return to the antenna,
achieving more energy concentrated at the tip and therefore more effective and larger ablation zone around 6cm,
also different ablation shapes can be obtained by combination of varied types of antennas,
power applied and procedural time.
Generally,
antennas have 14G in diameter.
In both methods,
the configuration of the procedure is applied following the manufacturer's recommendations in terms of electrode/antenna type,
potency and time duration depending on desired results.
Each system has its own protocol to determine when the treatment is finished.
Overall,
the potential advantages of MV over RF ablation include faster ablations (typically 2–8minutes with high-powered systems) and higher temperatures without the limitations related to electric impedance (Fig 9).
MW has less dependence on tissue properties with more uniform results,
relative insensitivity to “heat-sink” compared with RF,
and the ability to create much larger ablation zones if needed.
(8)
TISSUE PROPERTIES: RFA vs MVA
In RF ablation,
the most important tissue properties are electrical and thermal conductivity,
in the other hand tissue impedance is inversely proportional to conductivity that inhibits heat transfer from direct heating zone into the surrounding tissues.
In MWA ablation,
the most important tissue properties are dielectric constant of tissue (relative permittivity) and effective conductivity,
the first one refers to how well energy will propagate through the tissue,
the second one refers to the amount of tissue water content and how well tissue will absorb microwave energy.
The rate of blood tissue perfusion and therefore “heat-sink” effect is much more important for RF than MV.
ORGAN-SPECIFIC CONSIDERATIONS: each organ system has different underlying tissue characteristics,
which can have substantial effects on the resulting thermal changes and ablation zone,
a list of thermal ablation considerations can be provide,
taking into account the most frequently organs treated.
• LIVER: The primary indications for thermal ablation in the liver are HCC and metastatic disease,
although lately it is increasingly used to treat benign lesions.
A particular consideration of thermal ablation is that it is more effective in HCC than in liver metastases due to “oven effect” produced by cirrhosis and the pseudocapsule,
this results in higher cytotoxic temperatures within the tumor.
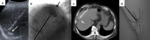
Small HCCs (up to 3cm in diameter) are affectively treated with RF or MW ablation alone (Fig 10).
Treatment of larger tumors (>3cm) with RF or MW monotherapy is associated with high rates of local recurrence (9),
so combination treatment with transarterial chemoembolization (TACE) and RF ablation (Fig 11) or MW ablation (Fig 12) results in fewer local failures (10,11) .
Liver´s high perfusion rate decreases the effectiveness of thermal ablation that’s why the clinical practice guides recommend MWA in lesions up to 5cm in diameter (12),
even 7cm in some trials.
(Fig.
13)
• KIDNEY: Most tumors treated with ablation are renal cell carcinomas (RCCs),
although sometimes this therapy can be applied to benign lesions (oncocytoma,
angiomyolipoma).
There are come critical considerations that must be considered in order to achieve effective treatment,
such as tumor size,
tumor location and proximity of vulnerable structures (8) (central tumors near vascular structures or near collecting system and ureter).
Central tumors may benefit from the placement of an ureteral stent and continuous pyeloperfusion.
Proximity of adjacent structures to kidneys (such as bowel,
spleen or pancreas) may require hydrodissection to allow safe ablation (13).
In small peripheral masses (<3cm),
RF and MW ablation have proven successful results (Fig 14),
even though MW is the preferred method because of its better ablation profile (faster and higher temperatures).
Tumors larger than 3cm can be difficult to completely treat with ablation (8),
and adjuvant therapies must be considered.
• LUNG: Most frequent lesions treated by thermal ablation are nonoperable non-small-cell lung carcinomas or metastases disease (8).
Aereated environment of lungs confers low electrical conductivity and poor thermal conduction that may restrict RF effect,
by contrast,
the lower permittivity and conductivity of air allows deeper MV penetration,
so it seems to be less susceptible to these effects and creates larger and more confluent zone of ablation compared with RF,
therefore MVA results in larger and more homogeneous ablation zones.
(14) (Fig 15).
Unlike standard lung biopsy technique,
in which the shortest possible path to the tumor is often desirable,
an indirect longer approach that traverses normal lung is better in ablation,
leaving an unablated tract of at least 2cm of aerated lung (Fig 16),
this consideration is based on possible pain,
potential skin burns or persistent air leaks and bronchopleural fistulas when ablation extends into pleural surface or chest wall.
Note that tract cautery should not be performed for same reasons.
• MUSCULOSKELETAL: Pain is the most common indication for percutaneous ablation of MSK tumors.
It is widely accepted for both painful bone disease metastatic and osteoid osteoma (8).
Soft tissue ablation is mostly performed for metastatic disease and both RF and MW seem to be effective,
always considering MWA advantages already mentioned.
In bone,
mostly same principles mentioned in lung may be applied.
Since bone has low conductivity and poor thermal conduction,
RF ablation is limited,
in contrast,
MW penetrates in bone deeper and is less affected by tissue heating or dessication,
therefore produces more effective ablation zones.
RFA is considered a standard therapy in osteoma osteoid (Fig 17) because of its availability,
but MWA may have a role in future.
Although radiotherapy is considered first-line treatment for intractable pain in metastatic disease,
it is expensive,
repeated sessions are often limited by dose and it is associated with delay in onset of effect,
so percutaneous ablation is good alternative therapy since it is widely available,
it can be performed repeatedly and its effects are almost immediates.
In summary,
MW energy produce faster and higher ablative temperatures,
thus larger ablation zones in shorter times,
besides its mechanism is less dependant on tissue properties of environment (15),
therefore MV produces predictable and more homogeneous ablation zones in comparison with RF.
GENERAL CONSIDERATIONS:
The WORK PLACE is an interventional radiology room,
adequately equipped.
The procedures are performed under aseptic conditions.
The ANESTHESIA TYPE required usually combine local anesthesia and conscious sedation in order to control the pain (16),
usually in presence of an anesthetist
The PREVIOUS PLANNING is fundamental to achieve successful results.
Check over previous imaging studies and medical history is very important.
Knowledge of number,
size and location of lesions to be treated as well as relations with other anatomic structures is primordial in order to selected the adequate system,
type needles,
imaging guide and routes of approach,
all these should be decided previously.
The GUIDE SYSTEM most frequently used is ultrasound due to its low cost,
wide availability and real-time visualization,
although CT/cone beam CT or even fluoroscopy are also possible alternatives.
The risk of BLEEDING is always present,
so a coagulation study before the procedure must be done (including platelets,
PT,
INR).
threshold values accepted are platelets >50000/mL,
PT>50%,
INR<1.3.
Patients with antiplatelet or anticoagulant therapy should discontinue medication.
SUMMARY
We provide two summary tables,
Table 1 sums up tissue reaction for various degrees of thermal injury (6),
and Table 2 summarizes a comparison between RF and MW ablation (1).