A.
Organization Pitfalls
a) To make the code to wait.
There are different protocols for stroke management,
most of them agree that the first 12 hours from the onset of symptoms are essential for treatment and prognosis.
Delaying the start of treatment in any of the different steps,
either intra and extra-hospital,
little clinical suspicion,
atypical presentations of stroke,
(series determine that up to 4% of acute strokes are ruled out due to low clinical signs) or simply failures of the different links that make up the diagnosis-treatment chain whenever facing a stroke,
is one of the main challenges in the management of stroke.
b) To not be prepared for the arrival of the code:
At the arrival to the CT of the code,
usually the room must be prepared,
even postponing other studies.
All the staff must have clear their functions and be ready at the time of the arrival of the patient.
To not prepare the contrast,
perform other activities,
to not prepare the patient with an adequate peripheral venous access or to not take in consideration possible elements that may artifact the study are the main challenges in this section.
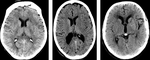
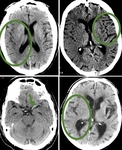
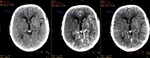
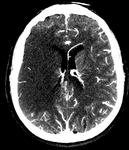
B. NECT:
a) To not give the correct interpretation to the NECT: basics such as hypodense is equal to dead,
overlook the hemorrhages or previous pathologies.
Fig.
1 and 2.
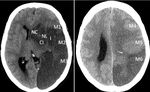
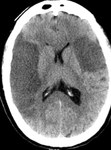
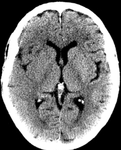
b) Wrong ASPECTS assessment:
ASPECTS (Alberta Stroke Program Early CT Score) is a 10 point scale to give a quantitative assessment by CT in patients with a MCA ischemic lesion,
subtracting 1 point from each infarcted vascular territory,
with a maximum of 10.
Fig.
3.
These territories are:
- Caudate
- Putamen
- Internal capsule
- Insular cortex
- M1: anterior MCA cortex,
(frontal operculum)
- M2: MCA cortex lateral to insular ribbon (anterior temporal lobe)
- M3: posterior MCA cortex (posterior temporal lobe)
- M4: anterior MCA territory immediately superior to M1
- M5: lateral MCA territory immediately superior to M2
- M6: posterior MCA territory immediately superior to M3
C.
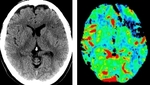
CT Perfusion Pitfalls
Acquisition Mistakes
a) Bad perfusion technique.
• Decrease the contrast flow without having an ideal venous access.
• Changes in the dose of contrast or mA,
con lead to mistakes in the acquisition or interpretation,
both visual and quantitative of the CT perfusion.
• Shoot only a first phase and not have a second one to complete the contrast curve or even use a poor technique in this second acquisition.
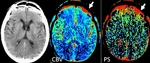
Patient head movements without correcting or even dismissing the area,
can lead to see a non-existing alteration on the perfusion maps.
Fig.
4.
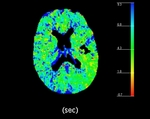
Interpretation
• Nowadays,
there is no study that demonstrates universal values for the interpretation and proper assessment of the perfusion maps,
and this is not the key to decide whether to treat or not.
The volume map should not be assumed as a gold standard for infarcted tissue without the rest of the study (NECT and CTA).
• Not using correctly the software for the evaluation of the perfusion curves.
• Erroneous automatic processing,
choosing the artery or vein incorrectly.
Acquisition of curves can be automatic,
but it must be known where the artery and vein control should be taken.
Fig.
5.
b) To evaluate the perfusion maps without correlation with the CT angiography,
NECT and the clinical findings.
Small infarcts are other potential source of CT perfusion interpretation pitfalls.
Can occur in the deep gray and white matter and often symptomatic,
leading to important neurological deficits.
One limitation of the CT perfusion is that the calculated maps have a relatively low resolution and these small infarcts can be overlooked.
Chronic small vessel disease or microvascular occlusive disease can become symmetrical and extensive,
leading to confusion and simulating an image of acute infarction on the perfusion maps.
D. CT angiography
ACQUISITION:
• Decrease the contrast flow without having an ideal venous access.
• Changes in the dose of contrast or mA,
con lead to mistakes in the acquisition or interpretation,
both visual and quantitative of the CT angio.
• Assess only the intracranial vessels and not to perform the supra-aortic trunks,
where there may be thrombosis.
INTERPRETATION
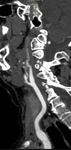
• Misinterpretation of CT angiography due to lack of contrast flow when a thrombus is at the bifurcation of the carotid.
Thrombi in this location can lead to a lack of contrast flow in the intracranial arteries,
as well flow through collateral arteries,
being difficult to delimit the exact location of the thrombus.
One way to correct this is by using the multiphase CT angio.
E.
Acute ischemia chameleons
Vasospasm is another condition in which CT perfusion findings can affect areas of penumbra in the context of acute ischemia.
Severe vasospasm has been correlated with the transient prolongation of MTT and CBF.
F.
Hyperperfusion
Seizures,
in addition to being a clinical presentation of acute cerebral ischemia,
both in convulsive crisis and post-crisis state,
can give an image of hyperperfusion,
which can become confused with acute ischemia,
by suggesting hypoperfusion on the contralateral side.
Fig.
11.
G.
Improper correlation perfusion-CT angio
Extra-cranial stenosis,
especially of the main internal carotid arteries,
leads to hypoperfusion,
which may be difficult to distinguish from acute ischemia.
Post-stenosis areas may overestimate ischemia by slowing the flow.
Fig.
7,
8,
9 and 10.