From 202 women eligible for the study,
one was excluded because of proven genetic mutation and 15 patients were excluded for the following reasons: 9 inappropriate registrations,
5 benign lesions and 1 lost of follow up (surgery performed out of our institution without available data).
A total of 186 patients were included in the analysis (Figure 1) addressed for 163 BIRADS 6 lesions and 35 suspicious lesions (BIRADS 0,
4 or 5) which were biopsied and confirmed as malignant.
Twelve patients had bilateral lesions.
The median age was 61,35 years (34,4 to 92,8).
Seventy-nine patients had MRI,
before or after review (42,5%)
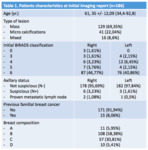
The population characteristics are listed in Table 1.
Primary objective:
Fifty-seven additional BIRADS 4 and 5 lesions and 23 additional suspicious lymph nodes were identified and sampled secondary to imaging review (details below).
This led to a change of management in 45 patients (45/186,
24% p < 0,01 and 45/62 patients with complementary exploration),
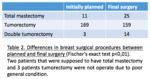
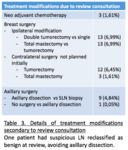
as shown in Tables 2 and 3:
- 35 patients had breast surgery modifications
- 4 patients had added axillary dissections
- 6 patients had both breast and axillary surgery modifications
Among the 18 neoadjuvant chemotherapies prescribed,
3 were secondary to the result of the review.
Secondary objectives:
1- Number of additional biopsies and USFNA and radiological-histological correlation
a- Breast lesions (Table 4):
A total of 69 additional breast core biopsies were realised after the review consultation in 48 patients (25,8% of total patients with 31 single,
14 double,
2 triple and 1 quadruple biopsies).
Among the 57 BIRADS 4 and 5 lesions explored,
malignancy was confirmed in 34 samples (49,3%) with 7 atypical lesions,
6 ductal carcinomas in situ (DCIS) and 21 infiltrative cancers.
Benign histological result was found in 23 biopsies and mostly in BIRADS 4 lesions.
Twelve additional BIRADS 3 lesions were sampled because of malignant lesion context: 8 were indeed benign lesions whereas 4 were atypical (n=3) or DCIS (n=1).
Finally,
false positive lesions at imaging represented 33,3% (23/69) of all breast additional biopsies,
occurring in 16 patients (8,6%).
b- Axillary status:
Reviewed images showed additional suspicious LN in 21 patients (two with bilateral suspicious lesions).
23 additional US-FNA were realised,
proving metastasis in 11 cases (47,8%),
leading to 9 ALN dissections.
In one case Hodgkin lymphoma with homolateral benign breast lesion was diagnosed (BIRADS 4 before biopsy).
Two patients had false negative results but one underwent axillary LN dissection in the first place because of suspicious MRI.
Besides,
22 patients without suspicious node showed metastatic cells on SLN biopsy with 8 micro metastatic and 14 macro metastatic lymph nodes.
2- Preoperative wire localization
Preoperative localization was modified in 40 cases (21,5%): in 14 cases it was no longer necessary because either a complete mastectomy or exclusive neoadjuvant treatment was decided.
In 26 cases,
management was modified because an additional lesion was discovered or the tumor size was underestimated.
Localization was easier after review thanks to the synthetis report performed by the reviewer.
3- Delay in surgery
Data for planned surgery was available for 49 patients (26,3%).
No significant delay was observed between planned and final surgeries except for 2 patients who had neoadjuvant chemotherapy.
4- Repeat surgeries (Figure 2)
Second hand surgery had to be performed for 38 patients (with one bilateral breast surgery and one breast and axillary surgeries)
- Repeat breast surgery was realised in 27 patients (14,5%): 2 for post-surgical hematoma and 25 for insufficient or invaded margins (19 DCIS,
4 No Special Type and 2 lobular invasive carcinoma)
- Repeat axillary surgery was realised in 13 patients (6,98%): 12 axillary LN dissections and 1 SLN biopsy because of micro metastasis
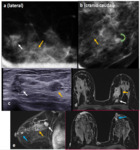
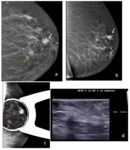
Figures 3 to 5 are examples of pateints with additional lesions.