As the incidence of HIV patients continues to increase and long-term survival improves,
more patients are being admitted for routine screening of breast cancer,
which becomes a diagnostic challenge given the particularities of HIV infection.
Therefore,
for the radiologist,
it becomes increasingly important to understand the subtleties in axillary lymph node analysis in these patients.Knowledge of the normal anatomy of this region is essential for the detection and correct interpretation of the tests,
as well as the possible differential diagnoses and the best methods to further diagnostic investigation (1).
There are three levels of axillary lymph nodes: level I,
lateral to the lateral border of the pectoralis minor muscle; level II underneath the pectoralis minor muscle; and level III medial to the medial margin of the muscle (2-4).
Axillary lymph nodes may be seen at mammography,
computed tomography,
and magnetic resonance imaging,
but ultrasound is the modality of choice for the evaluation (2).
Normal morphology
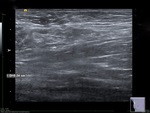
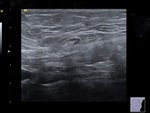
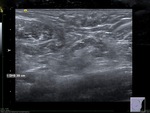
Features suggestive of normal axillary lymph node at ultrasound include on the normal lymph nodes: reniform shape,
with a thin cortex (maximal 3 mm),
a fatty hilum,
smooth margins,
small size (lesser than 10 mm in the maximal size of short shaft) (5-6).
Figures 1 - 2
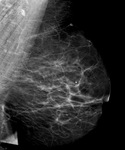
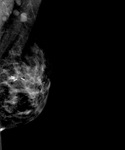
At mammography,
axillary lymph node with reniform shaped with a fatty hilum,
are considered benign.
Figure 3
Adenopathy
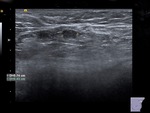
Features suggestive of axillary adenopathy at ultrasound include: cortical thickening (either diffusely or eccentrically),
loss of central fatty hilum,
irregular outer margins,
rounded morphology,
strongly hypoechoic and abnormal color flow.
Figures 4-5
At mammography round lymph nodes without fatty hilum are considered atypical (7-10).
Figure 6 A focal cortical thickening is the earliest detectable morphologic change related to metastasis.
Diffuse cortical thickening can also be seen with metastasis,
but is more often being associated with inflammatory conditions (11-12).
If the initial imaging evaluation of the axilla reveals a suspicious finding,
percutaneous procedures,
such as ultrasound-guided fine-needle aspiration or ultrasound-guided core biopsy,
should be performed (1).
In some special cases,
like patients with HIV,
the presence of multiple axillary lymph nodes or their atypical appearance are common and cytological evaluation may not be indicated.
The anatomopathological study is only justified in few cases,
such as a quick increased cortical thickening,
rounded morphology with the absence of central fat hilus or necrotic degeneration.
Differential diagnosis
Atypical lymph nodes may be seen related to both benign and malignant pathologies.
The differential diagnosis for an atypical axillary lymph node includes reactive hyperplasia to the inflammatories processes (like mastitis),
granulomatous diseases (tuberculosis,
sarcoidosis),
HIV/immunocompromised state,
lymphoma/ leukemia and metastatic disease (most commonly breast cancer and melanoma) (1,
3,
7).