Imaging findings:
This study exhibits uncommon tumours of meninges mimicking meningiomas and tumour like lesions of meninges.
A) Uncommon tumours of meninges mimicking meningiomas are as follows:
Extra axial hemangioma
Cavernous angiomas in the brain are usually intra-axial lesions.
Extra-axial cavernous angiomas are rare benign and slow-growing lesions and generally occur in the cavernous sinuses,
Meckel's cavity,
paracavernous regions and posterior fossa (1).
Cavernous angiomas have a tendency to bleed and can present with intra lesional bleed or as subarachnoid hemorrhage.
It may be difficult to diagnose the lesion preoperatively on radiology and are often misdiagnosed as meningiomas on imaging.
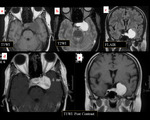
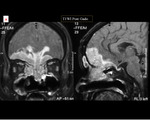
On MRI,
extra axial cavernous haemangiomas are hyperintense on T2WI whereas meningiomas are usually hypo-intense.
Extremely hyperintense signal on T2WI and intense enhancement on contrast MRI is the characteristic feature (Fig 1).
Diagnosing the lesion before surgery can help in avoiding complications (1,2).
Hemangiopericytoma
Intracranial hemangiopericytomas are highly cellular,
vascular tumours of the pericytes that originate in the meninges,
represent less than 1% of all CNS tumors.
They are aggressive and tend to occur at an earlier age than other meningeal tumours,
recur with high frequency,
and metastasize extra-cranially(3).
On CT,
hemangiopericytomas are heterogeneous,
hyperdense,
dural-based lesions that,
unlike meningiomas,
are not associated with calcifications or hyperostosis,
and they typically show heterogeneous enhancement.
Bone erosion is a feature seen in more than half of hemangiopericytomas[3,4].
On MRI,
hemangiopericytomas show prominent internal vessel with heterogeneously enhancing on contrast-enhanced images (Fig 2).
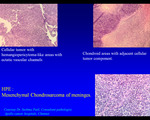
Meningeal chondrosarcoma
Skull base chondrosarcoma believed to arise from cartilaginous synchondroses is a well known entity.
However chondrosarcomas can occur intracranially arising from dura,
most common site being falx.
CT and MR appearance of intracranial dural chondrosarcoma is not pathognomonic,
but has features of a relatively slow-growing extraaxial tumor.
Adjacent bony erosions can occur and it appears avascular at angiography. It is different from the skull-base chondrosarcoma and may mimic an atypical meningioma(5).
|
Differentiating features
|
Intradural chondrosarcoma
|
Skull base chondrosarcoma
|
Meningioma
|
|
Imaging findings
|
Less calcified / lack of matrix calcification
|
Matrix calcifications present
|
Calcifications common
|
|
Changes in adjacent bones
|
Erosions
|
Bony destruction
|
Hyperostosis
|
|
Arteriography findings
|
Avascular
|
Vascular
|
Highly vascular,
enlarged dural feeding arteries
|
In this exhibit,
a calcified meningeal based enhancing tumour (mesenchymal chondrosarcoma of the meninges on histopathology Fig 3,
4 &5) in the left temporal fossa mimicking intraaxial lesion in a 28 yrs old male,
is documented .
Dural metastases
Metastases to the dura constitute one of the least frequent patterns of neoplastic spread to the craniospinal axis.
These neoplasms arise either by direct extension from skull metastases or by hematogeneous spread.
Breast cancer,
prostate cancer,
adenocarcinoma of the lung,
and renal cell carcinoma are the most common[6].
Typically,
these tumors are of increased signal on T2 weighted MRI with an enhancing dural tail mimicking a meningioma (Fig 6).
Primary dural lymphoma.
Primary dural lymphoma (PDL) is rare,
making up less than 1% of all CNS lymphomas (7).
The majority of PDLs represent the low-grade mucosa-associated lymphoid tissue (MALT) subgroup (7).
Since lymphoid tissue is absent in the dura,
the pathogenesis of PDL remains unclear(8).
PDL has a more indolent course than primary CNS lymphoma and is considered a subset of primary leptomeningeal lymphoma,
which originates from the meninges without any brain or systemic involvement as illustrated in Fig 7.
On imaging,
they are difficult to diagnose pre-operatively as primary dural lymphomas share many similarities with meningiomas.
Secondary CNS lymphoma
In 5–9% of systemic non-Hodgkin's lymphoma (NHL),
secondary spread involves the CNS (9,10),
usually in the form of leptomeningeal infiltrates,
and has a poor prognosis.
CNS involvement in aggressive NHL tends to occur early at a median of 5–12 months after the primary diagnosis of NHL.
Approximately 2/3rd of patients present with leptomeningeal spread and 1/3rds with parenchymal disease. Leptomeningeal spread,
often involves the cranial nerves,
spinal cord or spinal roots and may present as neuropathies.
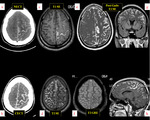
The imaging technique of is choice- contrast-enhanced MRI. CT is less sensitive.
Imaging findings are nodular thickening and abnormal enhancement of dura, Leptomeningeal,
subependymal,
cranial nerve and superficial cerebral lesions (Fig 8).
Absence of hyperostosis helps to differentiate lymphoma from meningioma.
Leptomeningeal leukemic metastases
Infiltration of the meninges by leukemic cells may affect the dura,
leptomeninges,
or both,
and may be diffuse or focal (10).
Leukemic meningitis usually presents as increased intracranial pressure.
CT and MR imaging show involvement of the meninges (diffuse or focal with abnormal meningeal enhancement)and involvement of the subarachnoid space (abnormal appearance of the CSF or diffuse enlargement of the cranial nerves) (Fig 9).
Three main differential diagnosis are subdural(SDH) or subarachnoid hemorrhage(SAH), infectious meningitis and leptomeningeal carcinomatosis.
SDH/SAH can masquerade the underlying dural lesion.
Hence,
contrast MRI might be indicated in a non-traumatic SDH, to assess the meningeal infiltration (Fig 9).
CSF analysis and history helps in differentiating infective versus leukemic meningitis(10).
Langerhans cell Histiocytosis (LCH)
LCH is one of a group of disorders caused by the overproduction of histiocytes,
a subtype of white blood cells.
CNS is involved in approximately 16% of LCH cases (11).Most common involved region in CNS is hypothalamic- hypophyseal region.Meninges,
pineal gland,
choroid plexus,
spinal cord can also be affected by LCH.
Calvarial lesions are associated with soft tissue component with or without dural invasion which typically have sharp borders with unequal involvement of the inner and outer tables,
resulting in a characteristic beveled-edge appearance seen on radiographs and CT scans.(12)
MR imaging shows tumour like lesions of intermediate signal intensity on T1- and T2- weighted images,
with intense contrast enhancement(Fig10).
Differentials include - Lymphoma,
leukemia,
carcinomatous infiltration.
Intracranial Rosai-Dorfman Disease (RDD)
Also known as Sinus histiocytosis with massive lymphadenopathy,
it commonly presents as massive,
painless,
bilateral lymph node enlargement in the neck with fever.
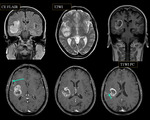
CNS involvement in RDD most commonly occurs in patients between 20-40 years.
Symptoms of intracranial disease include seizures,
headache and weakness.
Over 90% of CNS RDD involve the leptomeninges.
On MRI it usually appears isointense to grey matter on TIWI,
hyperintense on T2WI with typical homogeneous enhancement.
Multifocal meningeal enhancing masses with cervical lymphadenopathy in a child (Fig 11) would be consistent with this entity.
Differential diagnosis includes lesions such as meningioma,
histiocytosis X,
Wegener's granulomatosis,
sarcoidosis,
tuberculomas.
Radiologically and histologically they can mimic granulomatous lesions,
making histological and immune-histochemical confirmation essential (13).
Diffuse melanosis
Primary melanocytic lesions of the CNS arise from melanocytes located within the leptomeninges,
and this group includes diffuse melanocytosis and meningeal melanomatosis (seen in neurocutaneous melanosis),
melanocytoma,
and malignant melanoma (14).
These lesions may be well circumscribed or diffuse,
and their imaging appearances are influenced by the degree of melanin content as well as the presence or absence of hemorrhage.
In diffuse melanosis,
proliferating melanocytes diffusely involve the leptomeninges but without frank invasion of the brain.
On the other hand, melanocytoma appears as a solitary,
variably pigmented mass of the spinal and basilar leptomeninges resembling pigmented meningioma with minimal cytologic atypia.
Primary leptomeningeal melanomatosis
Primary leptomeningeal melanomatosis is a rare,
aggressive neoplasm of the CNS that arises from melanocytes within the leptomeninges and carries a poor prognosis.
It is also referred to as a meningeal variant of primary malignant melanoma.
CT and MR imaging - Diffuse thickening of the leptomeninges appears hyper intense on T1WI,
hypointense on T2WI,
with abnormal enhancement on the postcontrast images(Fig12).
Differential diagnosis include meningeal carcinomatosis,
meningitis,
and idiopathic hypertrophic pachymeningitis(15).
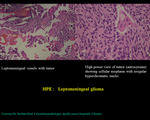
Leptomeningeal glioma
A primary leptomeningeal glioma is a rare neoplastic condition in which glial tumor cells extend diffusely throughout the leptomeninges without forming any intra-axial lesions.
Two anatomical and clinical forms have been described: a diffuse gliomatosis and a focal mass-forming lesion (16).
Diffuse form –
· More common form.
· Wide extra-axial dissemination of tumor cells with no mass formation.
· Diagnosis is challenging since it only depends on imaging studies.
· Histopathological examination is very important to differentiate from viral and fungal infections as well as tuberculosis and sarcoidosis.
Solitary and focal form –
· Rare,
often mimics meningioma.
· Prognosis better than that of a diffuse form.
· Enhancement on T1WI is less.
· Neither dural tail nor calcification.
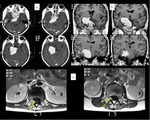
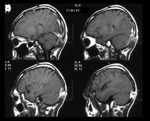
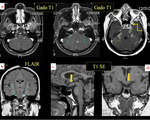
In this exhibit,
a heterogeneously enhancing lesion in the right temporal region mimicking intraaxial glioma in a 49 yrs old male is documented. The lesion appears to be supplied by multiple enlarged meningeal vessels and along with meningeal enhancement and without NAA peak on MRS indicating leptomeningeal glioma (Fig 13,14).
B)Tumor like lesions of meninges mimicking meningiomas:
o Sarcoidosis
o Granulomatosis with polyangiitis – Wegeners
o Meningeal angiomatosis
o Plasma cell granuloma
o Reactive lesions of meninges
· Superficial siderosis
· Meningeal fibrosis
o Meningeal granuloma
· Fungal lesion – pachymeningeal/ leptomeningeal form
· TB
Inflammatory myo-fibroblastic tumour
Plasma cell granuloma is a rare form of idiopathic inflammatory pseudotumour often characterized by non-neoplastic proliferation of plasma cells clinically mimicking a neoplastic process(13).
Pseudotumours of the CNS,
however,
are exceptional and rare.
In reported cases,
these reactive lesions occurred primarily in adults,
usually presenting as discrete tumours arising from the leptomeninges or dura.
In this study,
MRI displays as T1 low signal intensity infiltrative lesion involving pachymeninges and marked low signal intensity on T2WI with heterogeneous contrast enhancement (Fig 15).
Granulomatosis with polyangitis (Wegeners granulomatosis)(GPA)
GPA is a rare systemic disease characterized by necrotizing granulomatous inflammation and vasculitis(17).
Meningeal involvement is rare accounting 4-11% cases.
Pachymeningitis is the most common form of GPA related meningeal disease.
Focal / diffuse forms of dural thickening can occur.
o Focal form is contiguous with the adjacent sinonasal or orbit disease (direct spread) (Fig 16).
o Diffuse symmetric enhancing dural thickening (independent).
Differential diagnosis include lymphoma,
Neurosarcoid,
Infectious meningitis(17).
Neurosarcoidosis
Sarcoidosis is a systemic disease with non caseating granulomas.
Neurosarcoidosis occurs in approximately 5% of patients with sarcoidosis(17).
Imaging findings (Fig 17)
· Leptomeningeal involvement (most common)
· Pachymeningeal/dural masses (dark on T2WI)
· Enhancing brain parenchymal lesion
· Cranial nerve involvement
· Homogeneous post contrast enhancement
· Variable surrounding vasogenic edema
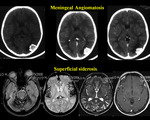
Meningeal angiomatosis
Meningioangiomatosis (MA) is a rare,
benign lesion usually affecting the leptomeninges and underlying cerebral cortex (18).
The pathogenesis of MA is unknown.
It can be diverse in its presentation on imaging ; for example,
MA can be gyriform or can be associated with a cystic component.
Imaging findings include calcification on CT,
susceptibility artifact on GRE and enhancement on T1WI( Fig18).
A diagnosis of MA should be considered when a young patient presents with a headache,
uncontrolled seizure,
in the setting of a calcified mass on CT and difficult to characterize mass on MRI (18).
Reactive lesions of meninges:
- Superficial siderosis
- Meningeal fibrosis
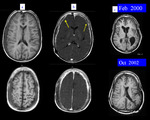
i)Superficial siderosis
Superficial siderosis of the CNS is a rare clinical entity that results from chronic hemosiderin deposition in the subpial layers of the brain and spinal cord that leads to gradual progressive neurologic deterioration (19).
Patients frequently present with slowly progressive gait ataxia and sensorineural hearing impairment.
Role of MRI is to establish or confirm diagnosis and also to evaluate potential causes of chronic or large hemorrhages.
Imaging findings are dark signal on T2 WI with blooming effect on GRE along the pial surface of the brain ( Fig 18).
ii)Meningeal fibrosis
Meningeal fibrosis is a noninflammatory pathologic process characterized by hypertrophy of the dural and arachnoid membranes of the brain(20).
It occurs in association with chronic subdural hematomas or subarachnoid hemorrhage,
with ventricular shunt placement,
and with rheumatoid arthritis.
Meningeal fibrosis is characterized by granulation tissue and collagen deposition.
Meningeal callus or post shunt meningeal fibrosis is a rare phenomenon seen in patients treated with shunt insertion that may mimic chronic subdural hematoma on unenhanced CT and MRI(21).
CT and MRI demonstrate low-density extra-axial collections that is indistinguishable from chronic subdural hematomas.
Contrast MRI can easily distinguish meningeal fibrosis (Fig 19) from chronic subdural hematoma(21).
As differential diagnosis,
intracranial hypotension in post surgery,
post lumbar puncture can also result in diffuse pachymeningeal enhancement similar to post shunt meningeal fibrosis.
The clinical features of intracranial hypotension help in differentiating this condition from meningeal fibrosis.
(20,21)
Meningeal granulomas:
- Fungal lesion
- Tuberculosis
Fungal meningeal granulomatous lesions
Acute or subacute fungal meningitis is often caused by yeast organisms,
and cerebrospinal fluid (CSF) analysis serves as the diagnostic gold standard(22).
.
Typical enhancement of the meninges is smooth or thick,
nodular and irregular,
long and continuous,
or asymmetric,
and may extend into the base of the sulci.
The image findings of fungal meningitis/granulomas are nonspecific and need to be correlated with CSF analysis and lab findings.
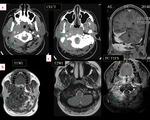
Tuberculosis meningeal granuloma
Imaging findings:
- Thickening and abnormal enhancement of meninges over the basal cistern
--Tuberculomas - parenchymal and meningeal
- Enhancing chronic basal exudates.
MRI is more sensitive than CT scanning in determining the extent of meningeal and parenchymal involvement
Granulomas shows T2 hypointense signal which raises the suspicion of tuberculomas (23) .
Systematic approach plays an important role in differentiating these lesions.
Age,
clinical history,
associated clinical conditions are important as also,
- Pattern of meningeal involvement
- nodular masses /nodular thickening/ sheet like involvement of pachymeningeal / leptomeningeal or both
- Extent of meningeal involvement – focal,
diffuse,
multifocal.
- Signal characteristics (extreme T2 hyperintensity,
T1 hyperintensity,
T2 hypointensity)
- Adjacent bone changes.