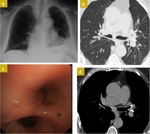
The non-neoplastic lesions of the tracheobronchial wall have different aetiologies.
We will review the main radiological characteristics of the following abnormalities: relapsing polychondritis,
granulomatosis with polyangiitis,
osteochondroplastic tracheobronchopathy,
tracheobronchial amyloidosis,
papillomatosis,
post-intubation stenosis,
idiopathic stenosis,
Mounier-Kuhn syndrome and bronchial anthracofibrosis.
1.
Relapsing polychondritis
Rare auto-immune syndrome characterised by the destruction of the cartilage,
especially from the auricle (90%),
nose (50%),
tracheobronchial wall (50%) and peripheral joints.
The laryngotracheobronchial presentation is seen in 10% of the cases,
but in approximately 50% of these,
the disease will eventually progress affecting the tracheobronchial wall.
When it affects the respiratory,
it is associated with a poorer prognosis,
being pneumonia the first cause of death in approximately 30% of patients.
It is more prevalent in Caucasian at the 40-60 years old.
Despite it affects equally men and women,
the tracheobronchial involment is more frequent in women.
It is characterized by recurrent episodes of cartilage inflammation with subsequent degeneration,
loss of structure and fibrosis.
It usually affects the larynx and the upper trachea,
although it can progress to the subsegmentary bronchi.
It can be diagnosed when three or more of the following are observed: bilateral auricular chondritis,
seronegative inflammatory polyarthritis,
nasal chondritis,
ocular inflammation,
chondritis of the respiratory tract,
and audio-vestibular lesions.
Conventional chest radiograph might show diffuse or focal airway affectation.
However,
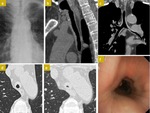
CT scan is the main tool ( Fig. 1 ),
which may present:
- Increased airway wall attenuation (calcium) and smooth thickening of the anterolateral tracheal wall with loss of structure of the cartilaginous rings and sparing of the posterior wall.
- Focal stenosis due to cartilage destruction and fibrosis.
- Collapse in the end-expiratory HRCT scan.
As for the bronchoscopy images,
diffuse airway narrowing,
mucosal oedema and erythema may be appreciated.
2.
Granulomatosis with polyangiitis
Granulomatosis with polyangiitis,
previously known as Wegener granulomatosis,
is a systemic necrotising non-caseating granulomatous vasculitis with unknown pathogenesis.
It usually occurs in middle-aged men.
Although it can affect any system and organ,
it has predilection for respiratory system and kidneys.
There is also a form of the disease affecting the lung and the lower airway,
without altering the upper airway or the kidneys.
In the classic granulomatosis,
larynx and endobronchial implication are usually late complications.
Conventional chest radiograph might present diffuse or focal airway affectation,
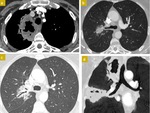
and the HRCT scans show ( Fig. 2 ):
- Circumferential and irregular thickening of the mucosa with ulceration.
- Rare affectation of the tracheal rings,
which can lead to stenosis.
If the peripheral bronchi wall is affected,
it can cause obstruction and atelectasis.
- Pulmonary nodular areas of increased attenuation that can cavitate.
- Ground-glass opacities.
- Pleural effusion is a rare presentation.
Findings at bronchoscopy are very variable.
Inflammatory ulcerations are the most frequent,
yellow-green plaques are related to active illness and,
therefore,
are the site of greater profitability on a biopsy; subglottic stenosis,
granulomatous inflammatory pseudotumors,
purulent secretions or lobar haemorrhage would be other presentations.
3.
Osteochondroplastic tracheobronchopathy
Rare idiopathic benign disease that affects the lower 2/3 of the trachea and major bronchi.
It is characterised by multiple submucosal osteocartilaginous nodules,
which can be focal or diffuse.
Men around 50 years old are more likely to suffer from osteochondroplastic tracheobronchopathy than women,
with a 3:1 ratio.
It is believed that this disease has a higher prevalence than estimated due to its asymptomatic course.
It is usually diagnosed after a difficult intubation or during bronchoscopy.
Cough,
shortness of breath,
recurrent infections,
wheeze and,
sometimes,
haemoptysis can be present.
Conventional chest radiograph shows nodular irregularity or asymmetric irregular stenosis in moderate-severe disease.
The HCRT scan shows ( Fig. 3 ):
- Thickening tracheal cartilage with irregular calcified nodules,
which spare the posterior tracheal wall,
as a pathognomonic featured.
- Pneumonia or atelectasis as possible complications.
Bronchoscopy shows multiple smooth,
white,
cartilaginous and hard nodules distributed in the anterolateral tracheal wall.
4.
Tracheobronchial amyloidosis
Disease characterized by abnormal protein deposits (amyloid) in the extracellular tissue,
it can be of idiopathic,
hereditary,
or inflammatory/neoplastic related aetiology.
Tracheobronchial amyloidosis can be found in two different scenarios: (i) as a part of a systemic process or,
(ii) rarely,
involving the airway and pulmonary parenchyma exclusively.
This later form is usually asymptomatic,
and can be found in three forms: diffuse interstitial lung deposits,
single or multiple nodules,
or submucosal tracheobronchial deposits.
Conventional chest radiograph might show a nodular appearance with irregular narrowing of the tracheal lumen.
If there is endobronchial occlusion,
lobar atelectasis can be seen.
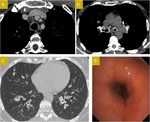
HCRT scan shows ( Fig. 4 ):
- Diffuse,
nodular and concentric thickening of the trachea and main bronchi wall.
- Sometimes nodular calcified lesions can be seen.
In this case,
differential diagnosis include osteochondroplastic tracheobronchopathy and relapsing polychondritis.
Whereas tracheobronchial amyloidosis has a concentric involvement of the lumen,
osteochondroplastic tracheobronchopathy and relapsing polychondritis spare the posterior tracheal wall.
Bronchoscopy shows white-grey flat plaques of amyloid deposit in the tracheal and main bronchi wall.
5.
Laryngotracheobronchial papillomatosis
Infection of the upper respiratory tract by the human papillomavirus (HPV).
It is more frequent in children,
after vaginal delivery infection.
Nontheless,
it can also occur in adults,
probably due to oral contact with infected genitals.
Papillomatous lesions are usually found in the larynx,
but the viral infection can be spread all through the tracheal and bronchial lumen,
and even reach the lung parenchyma.
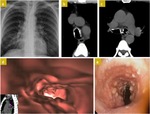
Radiological features are better viewed in the HRCT scan ( Fig. 5 ),
with:
- Diffuse nodular thickening of the airway wall,
or multiple nodules projected to the airway lumen.
- When it reaches the lung,
multiple and bilateral cysts and cavitated nodules can be seen.
- Atelectasis,
air trapping,
infections or bronchiectasis can also be seen when airway obstruction happens.
Bronchoscopy shows white polypoid appearance in the larynx,
trachea or main bronchi wall.
6.
Post-intubation stenosis
Among others,
post-intubation stenosis is caused by the high pressure of the endotracheal tube balloon against the tracheal wall,
with mucosal necrosis and secondary scar and stenosis outcomes.
It occurs in the subglottic region,
typically 3-4 cm below the cricoid cartilage,
whereas stenosis in patients with history of tracheostomy occurs at the stoma site.
Symptoms are variable and can include shortness of breath or stridor.
Conventional chest radiograph and HRCT scan show a symmetric,
focal subglottic stenosis with an hourglass shape ( Fig. 6 ).
7.
Idiopathic laryngotracheal stenosis
Idiopathic stenosis consists in the narrowing of the upper airway due to an unknown cause,
although gastroesophageal reflux or autoimmune diseases have been suggested as aethiology.
It is a rare and slowly progressive disease more prevalent in women than men.
It usually affects the subglottic region,
but it can also involve the upper trachea.
Symptoms are variable,
similar to those present in post-intubation stenosis,
including dysphonia or life-threatening airway obstruction,
with a long duration of 2 years on average.
Radiological features are heterogeneous,
although the most frequent appearance is a smoothed hourglass shaped stenosis ( Fig. 7 ).
8.
Mounier-Kuhn syndrome
Mounier-Kuhn syndrome or tracheobronchomegaly is characterised by the important and diffuse dilatation of the trachea and the main bronchi due to atrophy of smooth muscle and elastic tissue,
especially in middle aged men.
This disease has an unknown cause,
although a congenital predisposition has been hypothesised.
This condition can be an accidental finding in a chest X-ray of an asymptomatic patient undergoing imaging for other indications,
but the most frequent symptom is recurrent airway infection.
HRCT scan shows an increased diameter,
more than 3 cm,
of the trachea and more than 2,4 cm in main bronchi.
Further,
airway dilatation with multiple diverticula projected between the cartilaginous rings,
and bronchiectasia.
( Fig. 8 ).
9.
Bronchial anthracofibrosis
Bronchial anthracofibrosis is characterised by bronchial lumen narrowing associated with anthracotic pigmentation without a significant exposure to smoking or pneumoconiosis.
It is described mostly in women in their sixties and it can be associated with tuberculosis in around 50% of the cases,
as well as with chronic exposure to biomass smoke.
Symptoms are very variable,
from chronic productive cough and dyspnoea,
to chest pain or obstructive pattern in pulmonary functional tests.
Conventional chest radiograph is not specific and does not show luminal stenosis,
but can show atelectasis,
and a reticular or reticulonodular pattern,
and sometimes a mass lesion.
HRCT scan shows ( Fig. 9 ):
- Mediastinal or hilar lymphadenopathies,
with calcified nodes adjacent to bronchi.
- Multifocal thickening of the bronchial wall causing smooth narrowing,
with a predilection for the upper and middle right lobe bronchi.
- Collapse in distal lung portions to the site of airway stenosis.
- Fibrotic bands.
- Nodules.
- Bronchiectasis.
Bronchoscopy shows a darkened bronchial mucosa.