We show our experience in oncohematologic patients who underwent MRI from January 2015 to date and showed focal lesions in the spine or pelvis.
MRI was performed on a 1.5 T unit with our standard protocol,
including :
- In the spine,
T1WI and T2WI spin-echo (SE) sequences in sagittal,
and axial plane,
STIR or T2 FSE FAT SAT and IF-OF in sagittal.
- In the pelvis,
T1WI and T2FSE FAT SAT in coronal,
and STIR and IP/OP in axial plane.
In some patients,
an elliptical/rounded region of interest (ROI) was placed at identical sites on the in-phase/out-phase images using electronic calipers to calculate signal intensity ratio (SIR) of OP/IP.
Final diagnosis was made on clinical basis,
radiologic follow up for at least 6 months,
biopsy and pathologic proof,
or according to other imaging methods such as nuclear medicine.
Metastasis,
malignant hematologic lesions,
typically bening lesions and other bening diseases such as degenerative disease,
bening fractures,
osteomyelitis,
or post-treatment changes such as medullary reconversion,
are shown.
We describe the radiological semiology in detail,
emphasizing on the imaging findings and clinical data that were hepful for making and accurate diagnosis.
BONE METASTASIS.
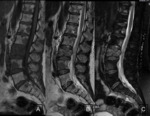
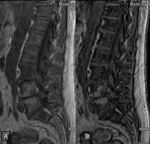
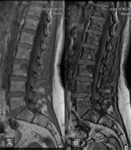
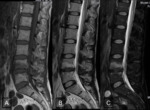
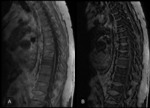
A 61-years old female with gastric adenocarcinoma stage IIIB with invalidant back pain.
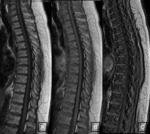
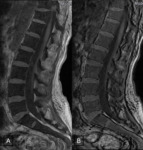
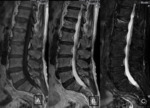
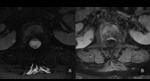
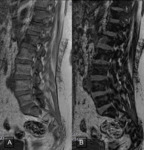
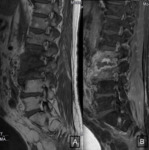
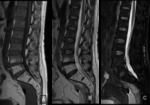
MRI images showed multiple focal lesions in the spine which were hypointense on T1, hyperintense on T2 and T2FatSat (Fig. 1) .
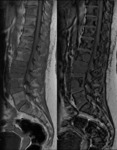
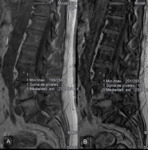
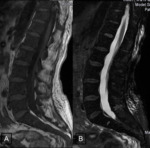
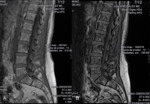
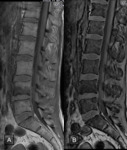
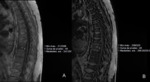
On the OP sequence,
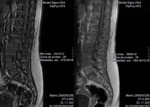
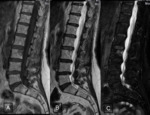
they showed a signal drop (Fig. 2 );inthe quantitavie assessment,
the signal intensity (SI) was higher in some locations; where there was a signal drop,
it was lower than 20% ( Fig. 3 ) .
Bone metastasis diagnosis is usually made with conventional sequences of MRI. However,
as it is a rapid and easily performed sequence,
some authors have proposed to include CSI in routine bone tumour protocol of the spine and pelvis (4).
IP / OP MRI does not inherently differentiate between benign and malignant marrow-replacing tumours,
and it is only useful for differentiating non-marrow-replacing processes (that are usually benign) from malignant lesions (5).
Some cases of false negatives in the IP/OP sequences in metastasis with a signal drop higher than a 20% have been published.
This has been attributed to the extensive normal fatty marrow and the small amount of tumor within the lesion (4).
Magnetic susceptibility artifact of densely sclerotic metastases,
and renal cell carcinoma metastases containing fat may produce it (6).
In our experience,
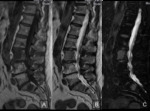
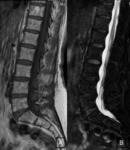
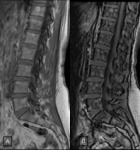
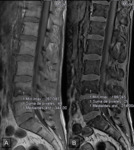
the signal intensity in blastic metastasis on the out of phase sequence may have an atypical behaviour in comparison with the on-phase sequence ( Fig. 4 ,
Fig. 5 ,
Fig. 6 ).
Some authors have also shown a return to a benign SIR of malignant lesions treated with radiotherapy,
whereas the standard spin-echo sequences remained abnormal.
Therefore,
quantitative evaluation of the signal intensity in the in-out of phase could be a early marker of treatment response of bone metastasis (7).
MALIGNANT HAEMATOLOGICAL DISEASE.
A 23 year-old male with acute lymphoid leukemia who underwent a stem cell trasplant four years ago showed a metabolic increase on T5 in a PET-CT study.
As a consequence,
an MRI was performed.
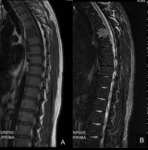
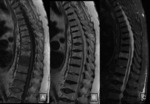
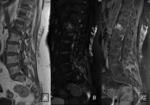
On it,
a diffuse alteration of the SI,
with hipointensity on T1, and hyperintensity on STIR sequences and on OP compared with IP sequence was observed.
Biopsy confirmed the leukemia relapse ( Fig. 7 ,
Fig. 8 ).
Bone marrow infiltration of leukemia,
lymphoma and multiple myeloma on MRI can show various patterns,
ranging from normal to focal or diffuse appearance. When infiltrative,
enough interspersed fatty marrow may be present between malignant cells,
leading to a signal drop on OP compared with IP images,
which may produce a misleading result on IP / OP MRI.
As an example,
we show a case of a quiescent multiple myeloma with an abigarrated pattern of bone marrow infiltration and a clear signal drop in the out of phase sequence ( Fig. 9 ).
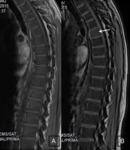
The opposed phase technique is less useful on primary haematopoietic malignancies,
which are disorders that can contain neoplastic elements admixed with fat (8).
However,
when lesions completely replace the normal marrow,
a haematological malignancy should follow the pattern of a primary lesion,
with no signal drop on OP compared with IP images ( Fig. 10 ,
Fig. 11 ).
ATIPICAL HEMANGIOMA.
A 68 years old female with invasive ductal breast carcinoma T2N0M0 in January 2015 underwent an MRI due to a back pain.
On it,
on the posterosuperior corner of L3,
an hypointense on T1 with heterogeneous SI on T2 and hyperintensity on T2 Fat sat with insufflation of the posterior vertebral cortex appeared; on the OP sequence,
there was a drop of the signal intensity.
The biopsy confirmed the absence of neoplastic cells ( Fig. 12 ,
Fig. 13 ,
Fig. 14 ).
Hemangiomas are slow growing benign neoplasms that are commonly found in the vertebral bodies.
Typical hemangiomas have a characteristic behaviour of signal intensity which is determined by the presence of fat and vessels,
hyperintense on T1 and T2WI,
hypointense on fat-supressed sequences and show a drop of signal intensity on the OP sequence ( Fig. 15 ).
In some hemangiomas with a fatty component predomination,
they may not show a drop in signal intensity because there are few or no nonlipid elements (Fig. 16).
If the vascular component of the atypical hemangioma predominantes,
it leads to an hyperintensity on the fat-supressed sequences,
and makes a differential diagnosis with malignancy on the oncohematological patient to be considered.
Atypical hemangiomas which contain only small or microscopic quantities of fat,
may demonstrate the utility of CSI MRI because they will lose signal intensity on OP images (9).
DEGENERATIVE SPONDILOARTHROPATHY.
A 38 years old female with a breast cancer in treatment underwent a MRI because of back pain.
MRI showed an alteration of the SI of exclusively the superior end-plate of L4 consistent with hypointensity on T1 and hyperintensity on T2 fat-sat sequences associated with dehydratation.
On the IP/OP sequences,
there was a signal drop on the OP which suggested that the edema was secondary to type I Modic changes.
The patient improved with nonsteroidal antiinflammatory drugs and conservative treatment for pain.
On the follow-up MRI performed two months later,
a small disc herniation and posterior annular fissure was depicted,
findings that helped in the diagnosis of degenerative discovertebral disease.
( Fig. 17 ,
Fig. 18 ,
Fig. 19 ).
Degenerative espondilosis can lead to edema in the normal fat marrow of the vertebral endplates (type I Modic changes).
It generally does not creat diagnostic difficulties,
even though on patients with malignancies,
they can propose the differential diagnosis with tumoral infiltration,
above all if the alteration is extense or has a a pseudonodular morphology.
The signal intensity drop on the out of phase indicates the presence of normal hematopoietic marrow,
wich prevents from an innecesary biopsy (3).
OSTEOPOROTIC VERTEBRAL FRACTURE.
An 86 years old male with chronic obstructive pulmonary disease and an operated vesical neoplasm was in study for fever and mechanical back pain of several days.
On the conventional radiography,
multiple vertebral fractures were observed.
The MRI showed an heterogeneous alteration of the SI of the whole spine with some fat pads and a loss of height in multiple vertebral bodies in relation with chronic osteoporotic fractures.
On T9,
a minimal loss of height and a a diffuse alteration of the signal intensity,
was depicted.
The OP sequence did not show signal drop on the quantitative or qualitative assessment.
As the patient improved with conservative management,
a biopsy was not performed,
and the lesion was diagnosed of subacute osteoporotic fracture ( Fig. 20 ,
Fig. 21 ,
Fig. 22 ).
An important diagnostic dilemma in the oncohematologic patient is to differentiate a benign acute fracture from a pathologic one.
Not always do the osteoporotic fractures show the typicall semiology such as the horizontal band edema or the presence of a cystic inside it (Kümmel cyst) ( Fig. 23 ).
Both bening and malignant fractures are hypointense on T1 and hyperintense on fluid-sensitive sequences,
and when typical features of benignity are not present,
many authors conclude that the signal drop on the OP compared with the IP sequence is an indicative of bening fracture.
A SIR < 0.8 (>20% signal drop) is characteristic of a non pathologic fracture.
However,
false positives may occur on benign fractures with no signal drop on the OP sequence: in acute posttraumatic vertebral compression with massive bone marrow edema that do not show signal drop on the OP sequence due to abundant water; also in patients who had a previous history of radiotherapy for vertebral metastases,
do these lesions not show a drop in signal on OP images,
as the marrow is now dominated by fat,
and water and fat no longer co-existed in such lesions (10); another possible cause of pitfall is the presence of fibrosis (6).
SPONDYLODISCITIS / OSTEOMYELITIS.
A 74 years old female with a quiescent multiple myeloma and a posttraumatic fracture on L1 suffers from sever back pain and fever.
With the suspected diagnosis of spondylodiscitis,
an MRI with the conventional sequences and fat-sat T1 contrast-enhanced sequence,
showed collapse of the anterior part of the inferior endplate of L1 with a pseudonodluar area of bone edema and enhancement in the anterior middle of the vertebral body which extended minimally to the pre and paravertebral soft-tissues; on the out of phase sequences,
this area showed no signal loss. The blood culture revealed growing of a streptococcus agalactie.
The patient was then diagnosed with vertebral osteomyelitis and treated with antibiotherapy,
with significant improvement of the symptoms.
( Fig. 24 ,
Fig. 25 ,
Fig. 26 ).
Treatment with chemotherapy and/or radiotherapy for oncohaematological disorders may cause complications owing to drug toxicity and/ or immunosuppression,
including osteomyelitis / spondylodiscitis by opportunistic pathogens.
As in this acase,
not always do the infectious lesion presents with the typical alteration of SI of the endplates and discs or the presence of paraespinal or intradiscal colections ( Fig. 27 ),
which makes differentiation with a malignant lesion very difficult.
The IP/OP sequence may be useful to characterize ostemyelitis even though its use has been less studied than in other pathologies.
However,
massive bone marrow edema in osteomyelitis may result in a lack of signal drop between IP/OP images; the SIR may be >0.8 when marrow is replaced by pus or intramedullary abscesses are present,
which are marrow replacing processes.
It has been described that the SI on this sequence varies depending on the grade of severity and time of evolution of the disease; on early osteomyelitis,
bone marrow water content results in an SIR <0.8,
but as the process worsens,
signal drop may diminish due to the formation of pus or abscess in the medullary canal (3).
Therefore,
complicated osteomyelitis could be an example of false positive of the IP/OP on the oncohematological patient (11).
MEDULLARY RECONVERSION.
A 55 years old with a colon neoplasm in treatment with chemo- and radiotherapy presented with acute onset of severe pain on the left hip irradiated to the knee and associated loss of sensibility in the pelvis.
A difficulty to wound was also present.
On the MRI study of the lumbar spine,
a decrease of the signal intensity in all the sequences from D12 to L4 with increase of fat on L5 and sacrum atributted to radiotherapy was observed ( Fig. 28 ).
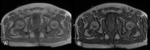
In the pelvis and proximal femurs,
there was also a diffuse alteration of the signal intensity,
with some hypointense punctate on the FSE T1 sequence not visible on the STIR sequence and with signal drop on the out of phase ( Fig. 29 ).
The patient was therefore diagnosed of medullary reconversion secondary to treatment.
The hip pain was attributed to an extraforaminal righ hernia L4-L4 that was seen in the MRI.
Red marrow can be activated secondary to treatment with growth factor,
marrow transplant,
or in response to anemia or other comorbidities of malignancy (3).
On FSE T1WI,
hematopoietic marrow is differenciated from tumoral infiltrative marrow according to its ill-defined borders and the superiority of the signal to that of the muscle; however,
when the red marrow is abundant,
this differentiation may be difficult.
In these cases,
the red marrow may have a SI similar or inferior to that of the muscle.
CSI pulse sequences are therefore helpful,
as a marked signal drop on the OP sequence compared with the IP sequence occurs.