Keywords:
Abdomen, Gastrointestinal tract, Interventional non-vascular, Ultrasound, CT, MR, Drainage
Authors:
T. Peachey, J. Smith, H. Nathani, F. Lee; Sheffield/UK
DOI:
10.1594/ecr2018/C-2008
Results
During the three year study period,
151 patients underwent cholecystostomy insertion. Thirty-eight were performed in 2014 (25%),
61 performed in 2015 (40%) and 52 performed in 2016 (34%).
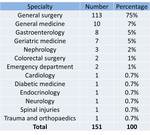
General surgery referred 113 patients (75%). The remaining 38 (25%) were referred from a variety of hospital specialties: ten (7%) from general internal medicine; eight (5%) from gastroenterology; seven (5%) from old age medicine; three (2%) from renal medicine; two (1%) from colorectal surgery; two (1%) from the emergency department. Six specialities each referred one patient (4% of all referrals): cardiology; diabetic medicine; endocrinology; neurology; spinal injuries; trauma and orthopaedics (table 1).
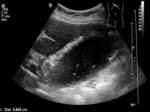
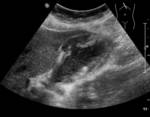
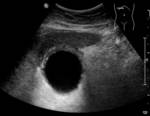
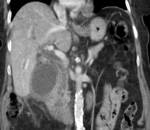
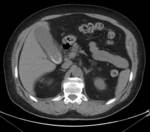
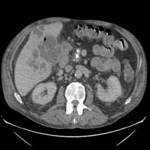
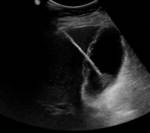
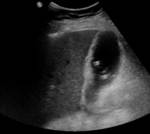
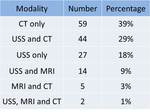
The most common imaging investigation prior to cholecystostomy was CT alone (39% of cases). The next most common was ultrasound followed by CT (29% of cases). Less than one in five patients had an ultrasound alone (18%). Further breakdown of imaging investigations performed is provided in table 2. There were a variety of imaging findings (figures 1 - 6),
the most common was an oedematous gallbladder which was seen in two thirds of cases. Eighty cases (53%) demonstrated gallstones,
53 (35%) had a perforated gallbladder,
18 (12%) had biliary dilatation and 12 (8%) had a liver abscess (table 3).
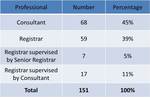
A consultant radiologist performed or supervised 85 (56%) of cholecystostomies (table 4). The cholecystostomy was recorded as direct (avoiding liver) in 37 cases (24%),
22 (15%) were recorded to be inserted through the liver parenchyma (transhepatic,
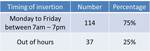
figure 7). The route was not stated in 92 cases (61%). Figure 8 is an example post-procedural image demonstrating the pigtail catheter to be within the gallbladder. Cholecystomies were performed within normal working hours in 114 cases (75%). Normal working hours were considered to be Monday to Friday between 7am and 7pm. Thirty-seven cholecystostomies (25%) were performed outside normal working hours (table 5). 65% (24/37) of the cholecystostomies performed out of hours were at the weekend.
Analysis of patients from 2016 found that 14/52 (27%) had severe cholecystitis,
37/52 (71%) had moderate cholecystitis,
and 1/52 (2%) had mild cholecystitis according to the Tokyo guidelines (table 6). Forty-one (79%) had an organism cultured on bile samples taken at the time of cholecystostomy insertion. A variety of organisms were cultured. The most common organism was escherichia coli (24 cases,
46%),
three cases grew klebsiella pneumoniae (6%). A variety of other organisms were grown including enterococcus and anaerobes. Only one case (2%) was suspected to have been contaminated.
Post-procedural outcome analysis was carried out on the 2015 cohort. Relevant post-procedural blood tests were not available on every patient. In those available,
86% (36/42) had a significant or complete normalisation of white cell count,
81% (34/42) had a significant or complete normalisation in c-reactive protein.