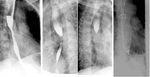
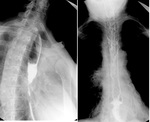
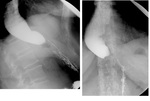
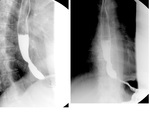
This contrast-enhanced imaging technique enables visualization of different parts of the gastrointestinal tract.
- Technique:
Patient preparation: [2]
- upper GI fluoroscopy: 6-8 hours fasting,
avoiding smoking or chewing gum.
- lower GI fluoroscopy: 6-8 hours fasting,
using commercially available prepackaged liquid diet.
- lower GI fluoroscopy to evaluate the anastomotic disruption after resection and before restoration of bowel continuity: no patient preparation is required.
Contrast agents: [3]
- barium sulfate- available in different densities,
it is contradicted if perforation is suspected.
- gastrografin- iodine-based,
hypertonic solution,
it is contradicted if risk of aspiration is suspected because it might cause prompt pulmonary edema if accidentally introduced into the tracheobronchial tree.
- non-ionic low-osmolar contrast media (for example Visipaque®)- iodine-based,
suggested in patients who are at risk of aspiration.
Oral administration of intravenous contrast media can improve patient comfort due to the better taste and provide the same opacification in comparison to conventional oral contrast media.
At present,
their use is limited to individual cases due to the higher costs.
[4]
Contradictions: [5]
- upper GI fluoroscopy: pregnancy,
breast-feeding,
allergies,
difficulty swallowing,
drug interactions.
- lower GI fluoroscopy: pregnancy,
breast-feeding,
allergies,
difficulty swallowing,
drug interactions,
inability to turn quickly/effectively,
generalized peritonitis,
toxic megacolon.
Radiation dose:
Radiation dose delivered during fluoroscopy is highly dependent on the operator,
however,
most manufacturers install a variety of tools on fluoroscopy equipment to help personnel adhere to the ALARA (as low as reasonably achievable) principle.
No roentgenogram should be taken at random.
Each image should answer ”yes” or ”no” to the diagnostic question since images giving ”maybe” are useless,
even if they are numerous.
Positioning:
Examinations of the esophagus,
stomach and duodenum can be carried out entirely with most patients in the upright position,
as opposed to Computed Tomography scan when the patient is scanned in the supine position.
The screen is centered at the esophagogastric junction and the patient is told to drink a cup of barium suspension.
The contrast agent fills and then coats the lining of the intestinal tract making the esophagus,
stomach and duodenum visible.
All images are obtained at different angles through the chest and abdomen.
Barium examination of the small intestine is more time-consuming.
The consistency of contrast medium is chosen so that it would pass out of the stomach at a fairly rapid and uniform rate and be of sufficient consistency to pass evenly,
and preferably very slowly,
through the small intestine.
All the images are taken,
mostly in the prone position,
one half hour after the upper gastrointestinal tract examination and then at two,
four,
and six hours.
The time interval is varied according to the rate of gastric emptying.
The time taken for the barium to reach the caecum should be always recorded.
Single-contrast barium enema is a method of imaging the colon with fluoroscopy.
The colon is filled with a contrast material which is done by pouring the contrast material through a tube inserted into the anus.
Patient is asked to turn to different positions (sides,
front,
and back).
The table may be tilted slightly to help the barium flow through your colon and to take images from different directions.
When the test is finished the enema tube is removed.
[6]
2.
Common oncological abnormalities:
Esophageus: [7][8][9]
- Esophageal cancer: Esophageal cancer is the eighth most common cancer,
and the sixth most common cause of cancer related deaths worldwide.
Squamous Cell Carcinoma (SCC) is the most common type of esophageal cancer worldwide.
The two most common histological types of esophageal carcinoma include SCC and adenocarcinoma.
- Esophageal sarcomas
- Esophageal lymphomas
Stomach and duodenum: [10]
- Gastric cancer: Gastric cancer is the fourth most common cause of cancer-related death in the world, and it remains difficult to cure in Western countries,
primarily because most patients present with advanced disease.
Adenocarcinoma is the most common type of gastric cancer worldwide.
- Gastric lymphomas
- Gastrointestinal stromal tumors
Small intestine/ large intestine: [11][12]
- Colorectal cancer: Colorectal cancer is the third leading cause of in both men and women and arise from the inner wall of the large intestine or rectum.
Adenocarcinoma is the most common type of colon cancer worldwide.
- Small intestine sarcomas
- Small intestine lymphomas
3.
Common indications for GI series and fluoroscopy in oncology patient:
Fluoroscopy enables not only morphologic assessment of GI tract disorders,
but also permits its functional evaluation.
Historically,
this method was used to detect malformations,
malpositions,
modification of shape and trajectory of organs,
motor and secretory functional disorders,
and also organic lesions.
Nowadays,
GI series are done mostly to the following indications:
Common esophageal indications: [13][14][15]
a.
pretreatment esophageal tumor evaluation:
- size of the tumor of the esophagus
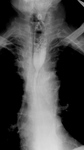
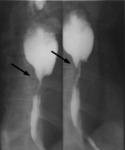
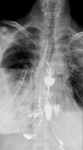
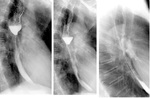
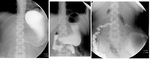
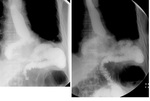
- esophageal patency: detection of esophageal stenosis and degree of contrast retention above the stenosis,
esophageal lumen narrowing,
esophageal lumen dilatation (Fig.1)(Fig.2)(Fig.3)(Fig.4)(Fig.5)(Fig.6)
- evaluation of esophageal rigidity
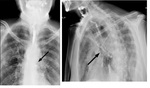
- tracheoesophageal fistulas,
esophagomediastinal fistulas and cancer ulceration (Fig.7)(Fig.8)
b.
posttreatment esophageal tumor response: surgery,
chemo-/radiotherapy:
- evaluation of esophageal patency: detection of esophageal stenosis and degree of contrast retention above the stenosis,
esophageal lumen narrowing,
esophageal lumen dilatation (Fig.9)
- evaluation of esophageal rigidity
- tracheoesophageal fistulas,
esophagomediastinal fistulas and cancer ulceration
- evaluation of esophageal stent placement (Fig.1)(Fig.2)
c.
evaluation of complications after oncological treatment: surgery,
chemo-/radiotherapy:
- evaluation of validity of esophageal tube
- tracheoesophageal fistulas and esophagomediastinal fistulas
- evaluation of esophageal stent displacement
Common gastric/ duodenal indications: [16][17]
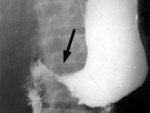
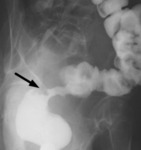
- evaluation of gastric/duodenal patency: gastric lumen narrowing,
gastric lumen dilatation, contrast retention (Fig.10)
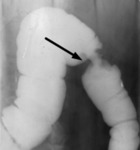
- evaluation of gastric rigidity: very useful in identification of primary gastric lymphoma and gastric linitis plastica,
which are characterized by a thickening and rigidity of the stomach wall.
In both cases,
lesions arise without destroying the architecture of the stomach wall making endoscopic diagnosis extremely difficult.
(Fig.11)
- evaluation of validity of gastro-esophageal anastomosis after subtotal gastrectomy and esophagojejunostomy anastomosis after total gastrectomy.
(Fig.12)
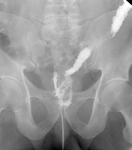
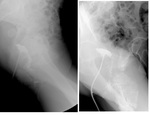
Common small intestine/ large intestine indications: [18][19]
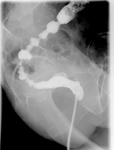
- evaluation of intestinal patency: intestinal lumen narrowing,
intestinal lumen dilatation (Fig.13)(Fig14)
- evaluation of intestinal rigidity
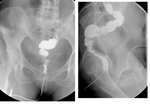
- evaluation of anastomotic disruption after resection
- evaluation of anastomotic disruption before restoration of bowel continuity(Fig.15)(Fig.16)(Fig.17)
- intestinal fistulas (Fig.18)
In 2017,
in Department of Radiology,
the Maria Sklodowska-Curie Memorial Cancer Center and Institute of Oncology in Warsaw,
were performed 156 examinations of the esophagus,
16 examinations of the small intestine and 13 lower GI tract examinations to evaluate the anastomotic disruption after resection and before restoration of bowel continuity.