Varicose veins are swollen,
deformed,
tortous veins,
that can occur anywhere,
but mostly they appear as branches of the great saphenous vein and small saphenous vein,
located in the subcutaneous tissues of the legs [1].
They are caused by a weakening of the vessel wall and incompetent valves,
which results in reflux of blood and venous hypertension [2].
They are a common problem in modern society,
affecting around one third of adults [2-5],
occuring more frequently in women than men [5,
6].
Although the age of onset varies,
the prevalence rises steadily with age,
with risk factors being prolonged standing or sitting,
pregnancy and sex [7].
Patients can present as asymptomatic, with only cosmetic complaints,
or with significant symptoms,
from aching,
pain,
discomfort,
itching or eczema,
to deep vein thrombosis (DVT) [2,
8].
Diagnosis and assesment
The diagnosis is made based on a clinical manifestation and ultrasound,
with duplex ultrasound considered as the gold standard for superficial venous incompetence.
It is used befor any therapeutic procedure to evaluate a patient for the venous insufficiency,
giving infromation about vein anatomy,
presence and location of a proximal obstruction,
vein valve function and venous reflux [1].
For more omptimal clinical managment,
a number of different venous severety assessment tools and QoLs can be used:
- clinical: Clinical,
Etiologic,
Anatomic,
and Pathologic (CEAP) classification,
Villalta scale,
and Venous Clinical Severity Score (VCSS)
- generic: the 36-Item Short Form Health Survey (SF-36) and EQ-5D questionnaires
- disease-specific: the Aberdeen Varicose Vein Questionnaire (AVVQ),
Chronic Venous Insufficiency Questionnaire (CIVIQ),
and VEnous INsufficiency Epidemiological and Economic Study on Quality of Life/Symptoms (VEINES-QOL/Sym) questionnaire [9].
Treatment options
Conventional surgery (high ligation,
stripping and phlebectomies) has been widely used for many years,
with the disadvantage of requiring general or spinal anesthesia,
recurrence rate up to 40% after five years [10,
11],
significant postoperative symptoms (especially pain and hematoma) and possible injury to the saphenous nerve [12,
13].
In the recent years,
a number of minimally invasive endovenous therapy techniques for axial incompetence (great saphenous vein (GSV),
small saphenous vein,
anterior accessory GSV,
etc.) have been developed,
which can be divided into thermal tumescent (TT) and more newely nonthermal nontumescent (NTNT) [14] ( Fig. 1 ).
Most widely used are radiofrequency ablation (RFA) and endovenous laser ablation (EVLA),
which in compare to conventional surgery stripping,
are associated to less pain,
discomfort,
reduced complications; such as wound infection and haematoma,
shorter return to work and overal they positively affect patient's quality of life [15-18].
However,
because of the thermal effect,
they can,
although rarely,
damage the surrounding tissues of the vein,
causing neuralgia,
skin burn and prolonged pain,
despite the use of tumescent anesthesia,
which can also cause complications at the point of puncture [19,
20].
Cyanoacrylate adhesive embolization and sclerotherapy (glue) has a reported saphenous vein closure rate of at least 94% at one year and causes a significant improvement in venous clinical severity score,
based on the recent studies [21,
22],
although further follow-ups are currently needed for more conclusive results.
In addition,
the lack of post-treatment compression may be appealing to patients,
but due to its tendency to cause deep venous occlusion,
it has to be handled carefully.
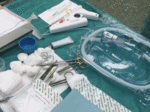
Mechanochemical ablation (MOCA),
with The ClariVein® Occlusion Catheter System (Vascular Insights,
Madison,
CT,
USA),
is one of the new generation nonthermal nontumescent endovenous ablation,
which induces closure by a combination of the mechanical damage and chemical injury ( Fig. 2 , Fig. 3 , Fig. 4 ).
It is used for the great saphenous vein (GSV),
the short saphenous vein (SSV) and the perforator veins [14,
23,
24].