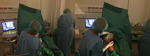
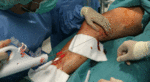
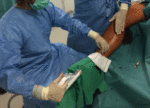
Patients are put in the reversed Trendelenburg position.
An ultrasound is perfromed to better demonstrate the target vein for access,
the saphenofemoral junction,
perforators,
tributaries,
diameter and treatment length ( Fig. 5 ).
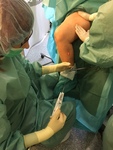
First,
a micropuncture access with a 4 Fr introducer sheath is obtained under an ultrasound and flushed with a saline liquid ( Fig. 6 ). When using a 4 Fr sheath,
the incision wound is small enough,
that no infiltrative local anesthesia and cutaneous suturing afterwards is needed.
The infusion catheter is then inserted through the sheath and the distal tip of the wire positioned 1 or 2 cm proximal from the saphenofemoral junction (SFJ) or saphenopopliteal junction (SPJ),
or 0.5 cm below the superficial epigastric vein ( Fig. 7 ),
using an ultrasound guidance.
Afterwards,
the patient is put into a flat position.
An iron wire inside the infusion catheter with an extending small iron ball through an opening at the tip of the catheter is activated and starts to rotate within the lumen of the vein at approximately 3500 rpm,
abrading the intima and prompting a venospasm. For this,
the patient feels only a slight vibrations.
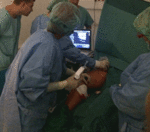
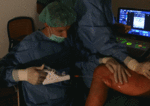
Simultaneously,
the sclerosant is infused into the vein,
while the catheter is being pulled back steadily at the pace of 1.0 and 2.0 mm/second.
A 1,5 – 2.0% liquid sodium tetradecyl sulphate (STD - Sotradecol©) or polidocanol (Aethoxysklerol©) is used as a sclerosant,
which is delivered to the distal end of the catheter,
near the rotating angulated wire,
via syringe attached to the handle ( Fig. 8 , Fig. 9 , Fig. 10 ).
This combined mechanism of action enchances coagulation by mechanical damage of the endothelium,
reduces vein diameter by creating a vasospasm,
increases the action of sclerosant by an increase in surface and evenly distributes the sclerosant at the endothel wall,
which makes occlusion more efficient.
Vein diameter and treatment length are used to determined potential sclerosant volume,
although the total volume of actual injected sclerosant depends from the mechanical and chemical effect to cause occlusion,
which is continuously monitored by a duplex ultrasound during the procedure.
It is adjusted to each individual and must not exceed a 7 ml of total volume.
After the procedure,
a duplex ultrasound is performed to check for patency of the common femoral vein and the deep venous system.
A compression bandage from the foot to the groin and/or a full lenght compression stocking are applied to the treated limb,
which are then removed during the following 3 weeks [23,
25,
26].
Indications:
- C2–C6 varicose veins
- primary GSV or SSV incompetence
- GSV/SSV diameters of 3 mm to 12 mm in the supine position
Contraindications:
- acute deep vein thrombosis (DVT)
- immobility
- pregnancy
- lactating
- allergy to sclerosant
- previous truncal varicose vein treatment
- peripheral arterial disease (ABPI < 0.8)
- history of deep venous thrombosis
- previous thrombophlebitis
- anticoagulation with warfarin
- severely tortuous GSV or SSV (relative)
- GSV diameters > 12 mm (relative)
[23,
26].
Outcomes
Clinical trials have shown it to be safe and effective for both great saphenous vein and the short saphenous vein [24,
27],
as well as successfully performed and well tolerated bilateral procedures and multiple procedures on the same leg [23].
Reported occlusion rates range from 94 to 97%,
with notable improvement in quality of life [23,
25,
28].
There have been shown a significant better procedure times and intra/postprocedural pain scores than for RFA and EVLA [29,
30].
Possible complications
Since no heat or tumescent anesthesia are needed,
complications that occur in thermal ablative modalities,
such as pain,
hematoma,
induration and nerve injury,
are greatly reduced [23,
25,
26].
Recently,
a large study,
reviewing a current literature,
has found,
that in total of 1,334 recorded patients,
treated with MOCA, overal complications were few (P < .001).
Three patients developed deep vein thrombosis (0.2%),
two of them pulmonary embolism.
All were successfully treated with an anticoagulation therapy with no further complications.
The rate of minor complications was low (11.1%),
with thrombophlebitis (5.2%) and ecchymosis (2.2%) being the most common [31].
Potential seriuous complication a professional also has to consider,
is a paradoxical embolism of brain-supplying or the intracranial arteries (e.g.
the middle cerebral artery or ventricular artery),
higly assocciated in patients with patent foramen ovale (PFO).
There have been reported cases of neurological disturbances,
such as transient ischemic attack (TIA) and even stroke,
in patients,
followed by a liquid or foam sclerotherapy [32,
33].
A similar patophysiologic mechanism of emboli formation might be assocciated with the mechanochemical ablation,
although no such report has been published yet.