Type:
Educational Exhibit
Keywords:
Bones, Anatomy, Musculoskeletal bone, Conventional radiography, CT, MR, Education, Education and training, Metabolic disorders
Authors:
A. N. Pérez Pérez1, A. P. Marrero González2, J. R. Ortiz-Cruz1, J. Lugo-Rosado2, E. Trullenque1, J. Vidal1; 1San Juan, PR/US, 2San Juan, Puerto Rico/US
DOI:
10.1594/ecr2018/C-2151
Findings and procedure details
1.
SPINE
-
Diagrammatic overview
-
See Fig. 1 and Fig. 2 for an overview of spine ossicles
-
Pictorial review
-
Nuchal ligament sesamoid ossicles
-
-
Prevalence: Overall 7.4%,
with male predilection (11.3% males,
3.5% females)
-
Location: Varies,
with 80% occurring either at C5/C6 or C6/C7 levels
-
Overview: An anatomical variant that is typically asymptomatic and may be misdiagnosed as an avulsion fracture or myositis ossificans.
[1]
-
Radiographic characteristics: Seen usually as a single,
well-defined and corticated,
round or ovoid opacity on lateral plain films,
and as cortical bone with central bone marrow within the nuchal ligament on computed tomography (CT) scans.
-
See Fig. 1 for diagram and Fig. 3 for case
-
Accessory ossicle of the anterior arch of the atlas
-
-
Prevalence: Unknown,
as it has been described in very few articles
-
Location: Articulates with the inferior aspect of the anterior arch of the atlas
-
Overview: Typically asymptomatic.
Relatively large ossicle,
roughly triangular (but may vary in morphology and size) that sits immediately below the anterior arch of the atlas that may articulate with the inferior aspect of the arch.
[2]
-
Radiographic characteristics: Well-corticated,
rounded ossicle beneath the anterior arch of the atlas,
best seen on lateral views of the spine.
-
See Fig. 1 for diagram and Fig. 4 for case
-
Persistent ossiculum terminale
-
-
Prevalence: Exact frequency unknown
-
Location: On superior aspect of odontoid process,
above the transverse alar ligament
-
Overview: Also known as terminal ossicle,
or Bergman’s ossicle,
and is due to the persistence of an unfused odontoid tip ossification center (which appears around age 3 and typically fuses by age 12).
[3] Usually asymptomatic and fairly stable.
May rarely present with neck pain.
May mimic a Type I dens fracture,
especially if fracture is chronic.
[4]
-
Radiographic characteristics: Smooth,
separate,
corticated ossicle at the tip of the dens,
with the dens usually of normal size.
-
See Fig. 2 for diagram and Fig. 5 for case
-
Os odontoideum
-
-
Prevalence: 0.7% in recent study,
though exact frequency may be unknown
-
Location: Ossicle situated superiorly to shortened dens base
-
Overview: May be misdiagnosed as a Type II dens fracture in the posttraumatic setting,
hence it is useful to seek common associated findings: shortened dens base and hypertrophied C1 anterior arch.
Most cases are asymptomatic and incidental.
Instability,
and associated symptomatology,
due to abnormal mobility of the dens with respect to the axis (C2),
however,
has been documented.
This may lead to central canal stenosis at the craniocervical junction with associated cord compression,
which may necessitate urgent surgical management.
[3-5] This ossicle has been classified into two types:
-
-
Orthotopic: Ossicle situated at expected anatomic location (superior to dens base); may articulate with the anterior arch of the atlas (C1) and is noted by a wide gap between the ossicle and the axis (C2).
Most common variant.
-
Dystopic: Ossicle is not in the expected anatomic location; often fused to the basion and termed os avis.
This variant has increased risk of instability.
-
Radiographic characteristics: Smooth,
well-corticated ossicle superior to a hypoplastic dens
-
See Fig. 2 for diagram and Fig. 6 for case
-
Oppenheimer’s ossicle
-
-
Prevalence: 1-7%,
with male predominance (6:1)
-
Location: associated to inferior (less commonly,
superior) articular process of the lumbar spine
-
Overview: Due to failure of union of ossification centers for the inferior (or superior) articular processes of lumbar vertebrae.
May be unilateral (20%) or bilateral (80%) and typically involves L2 or L3,
though L1 and L4 involvement may also be seen.
Very rare in L5.
Generally asymptomatic,
though may present with low back pain due to canal stenosis and cord compression (more common if bilateral).
May be misdiagnosed as a facet fracture,
especially in the posttraumatic setting.
[6]
-
Radiographic characteristics: Well-corticated,
round,
oval or triangular ossicle,
typically 0-1 mm in size,
on the inferior articular process of the lumbar spine.
-
See Fig. 1 for diagram
2.
SCAPULA:
-
Diagrammatic overview
-
See Fig. 7 for overview of scapula ossicles
-
Pictorial review
-
Os acromiale
-
-
Prevalence: Between 1.3-15%,
with male and African ethnicity predominance
-
Location: Anterior acromion
-
Overview: Due to a failure of fusion of one of three acromial ossification centers.
It may be unilateral or bilateral (30-60%).
Usually asymptomatic,
though may cause shoulder pain and scapulalgia in 10% of cases and thus must be identified to avoid unnecessary treatment with acromioplasty.
When symptomatic,
the pain is described usually on anterior elevation and abduction at the shoulder joint.
Symptomatic os acromiale is typically managed medically,
but may be surgically stabilized if intractable.
There are three anatomical subypes: [3,7]
-
-
Pre-acromion: in front of acromioclavicular (AC) joint
-
Mesoacromion: behind AC joint; symptomatic os acromiale is usually of this variant
-
Meta-acromion: at the base of the acromion
-
Radiographic characteristics: Unfused,
well-corticated anterior acromial ossicle,
best seen on axillary plain film views,
CT and MRI.
-
See Fig. 7 for diagram and Fig. 8 for case
3.
ELBOW:
-
Diagrammatic overview
-
See Fig. 9 for overview of elbow ossicles
-
Pictorial review
4.
WRIST:
-
Diagrammatic overview
-
See Fig. 11 for diagram of wrist ossicles
-
Pictorial review
-
Os styloideum
-
-
Prevalence: General prevalence of approximately 19%.
Of these 2% are isolated form,
3.5% are fused to capitate,
0.5% are fused to trapezoid and 94% are fused to the base of the second or third metacarpals; higher incidences have been noted in hockey players.
One of the six most common wrist ossicles
-
Location: On dorsal surface of second or third metacarpal base
-
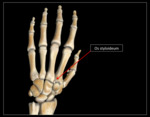
Overview: A bony structure at the dorsum of the second or third metacarpal,
also known as a congenital carpal boss.
The ossicle may or may not be fused to the adjacent metacarpal.
Its etiology may be either degenerative or congenital.
May be misdiagnosed as a fracture.
Generally asymptomatic,
but may sometimes cause dorsal wrist pain,
wrist rigidity or clinically simulate a ganglion cyst.
[3,11,12]
-
Radiographic characteristics: Smooth,
rounded ossicle next to the second and third metacarpal bases,
best seen on lateral radiographs.
May or may not be fused to the adjacent metacarpal.
-
See Fig. 11 and Fig. 12 for diagram and graphic representation
-
Os hamuli proprium
-
-
Prevalence: Not documented; one of the six most common wrist ossicles
-
Location: Lower section of palmar surface of hamate bone
-
Overview: Also known as an unfused hamulus,
a secondary ossification center of the hook of the hamate that is not fused with the body.
May be unilateral or bilateral.
Unilateral cases are more easily misdiagnosed as an avulsion fracture of the hook of the hamate.
[3,13]
-
Radiographic characteristics: Small,
rounded and discrete ossicle with corticated margins that may be associated with a hypoplastic hamate hook.
-
See Fig. 11 and Fig. 13 for diagram and graphic representation
-
Lunula
-
-
Prevalence: Exact prevalence unknown,
but thought to be between 0.3-1.6%; one of the six most common wrist ossicles.
-
Location: Between the tip of the ulnar styloid process and the triquetrum; within the meniscal homologue
-
Overview: An ossification center at the tip of the ulna that is found within the triangular fibrocartilage complex.
It is typically unfused,
but may also be found fused to the ulnar styloid process,
making this structure appear elongated.
May be misdiagnosed as an avulsion injury of the ulnar styloid.
-
Radiographic characteristics: Small,
rounded,
well-defined ossicle found distally at the tip of the ulnar styloid; if fused to ulnar styloid process,
may make this structure appear elongated.
[3,10]
-
See Fig. 11 for diagram and Fig. 14 and Fig. 19 for cases of lunula and persistent ulnar styloid
-
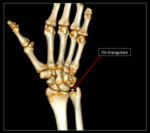
Os triangulare
-
-
Prevalence: 1% on right hand,
0.9% on left hand; one of the six most common wrist ossicles
-
Location: Just distal to the ulnar fovea,
between the ulnar styloid,
lunate and triquetrum
-
Overview: Also known as the os intermedium antebrachii or os triquetrum secundarium,
this ossicle is similar in appearance to the lunula,
but is located more radially to the ulnar styloid process.
May be unilateral or bilateral.
May be misdiagnosed as an ulnar styloid fracture or confused with a lunula.
[12,13]
-
Radiographic characteristics: Small,
rounded,
well-defined ossicle typically found distal to the ulnar fovea.
-
See Fig. 11 and Fig. 15 for diagram and graphic representation
-
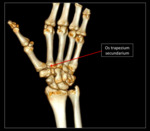
Trapezium secundarium
-
-
Prevalence: 0.5% on right hand,
2.1% on left hand; one of the six most common wrist ossicles
-
Location: At the superomedial aspect of the trapezium,
between the distal margin of the trapezium and the ulnar base of the first metacarpal
-
Overview: Develops as a separate bony appendage to the tubercle of the trapezium.
May be misdiagnosed as a fracture or confused with the hamulus.
[14]
-
Radiographic characteristics: Small,
rounded and well-defined ossicle between the trapezium and the first metacarpal bones.
-
See Fig. 11 and Fig. 16 for diagram and graphic representation
-
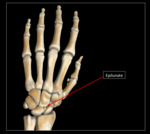
Epilunate
-
-
Prevalence: 1.6%; one of the six most common wrist ossicles
-
Location: At the dorsum of the hand,
in the angle between the scaphoid,
the lunate and the capitate.
-
Overview: Located distally between the scaphoid and the lunate,
it may projects into the joint,
simulating a loose body.
Typically asymptomatic,
but may also present with atraumatic wrist pain (unilaterally or bilaterally),
in which case surgical excision is usually curative.
[15]
-
Radiographic characteristics: Well-defined,
spherical,
bony protuberance found at the dorsal aspect of the lunate.
May be integrated into the scapholunate ligament.
-
See Fig. 11 and Fig. 17 for diagram and graphic representation
-
Os paratrapezium
-
-
Prevalence: 0.3% on right hand,
0.9% on left hand
-
Location: Between the disto-radial aspect of the trapezium and the radial base of the first metacarpal
-
Overview: May be unilateral or bilateral.
May be misdiagnosed as a loose body due to degenerative disease of the trapeziometacarpal joint (ex.
osteoarthritis) or trauma (fracture).
[3,14]
-
Radiographic characteristics: Well-defined,
rounded ossicle at its expected location.
-
See Fig. 11 and Fig. 18 for diagram and graphic representation
-
Os radiostyloideum
-
-
Prevalence: Exact frequency unknown,
but thought to be between 0.3-1.6%
-
Location: Adjacent to the radial styloid process and lateral to the mid-portion of the scaphoid
-
Overview: Also known as a persistent radial styloid.
Although generally asymptomatic,
it may present with dull wrist pain,
leading to misdiagnosis of fracture or skeletal injury.
[16]
-
Radiographic characteristics: Small,
well-corticated,
rounded bony structure adjacent to the lateral aspect of the radial head and distal pole of the scaphoid,
with normal trabecular pattern
-
See Fig. 11 for diagram and Fig. 19 for case
-
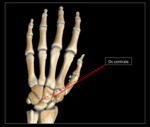
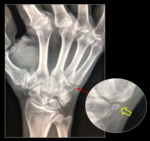
Os centrale
-
-
Prevalence: 0.3-1.6%
-
Location: Between the scaphoid,
capitate and trapezoid.
May also be found between the lunate,
triquetrum and hamate dorsally on the hand
-
Overview: A secondary ossification center thought to be due to failure of fusion between a small,
cartilaginous nodule and the scaphoid,
which typically fuses by 8 weeks of gestation.
May be unilateral or bilateral and may be fused with the scaphoid.
The majority of cases are asymptomatic,
though few cases present with intermittent pain,
clicking,
crepitus and limited mobility.
Symptomatic cases may be misdiagnosed as a scaphoid fracture.
May be unilateral,
bilateral or duplicated.
[17-19]
-
Radiographic characteristics: May be fused to the adjacent scaphoid,
capitate or trapezoid,
yet may also be radiographically occult,
presenting as a large gap between the scaphoid and the capitate.
Typically round and dense,
lacking internal trabecular pattern.
-
See Fig. 11 and Fig. 20 for diagram and graphic representation
-
Os vesalianum carpi
-
-
Prevalence: 0.1%
-
Location: Between the hamate and the fifth metacarpal.
May also be found in the second and third metacarpals and between the trapezium and capitate bones.
[3,19]
-
Overview: First described by Vesalius in 1543,
then 300 years later by Gruber.
May be misdiagnosed as a fracture.
-
Radiographic characteristics: Small,
rounded bone at the lateral aspect of the carpus adjacent to the fifth metacarpal and hamate.
-
See Fig. 11 for diagram and Fig. 21 for case
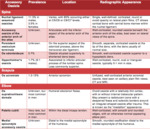
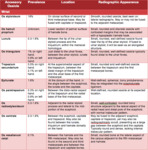
**See Table 1 and Table 2 for poster summary**

![Fig. 1: 3D models of the cervical [a] and lumbar [b] spine, highlighting the typical locations of the accessory ossicle of the anterior arch of the atlas [yellow], the nuchal ligament sesamoid ossicle [light blue] and Oppenheimer’s ossicle [red] at the inferior articular process of L2. Dashed lines represent other common locations of the respective ossicles. Ossicles drawn by Dr. Alexandra Pérez Pérez.
References: University of Puerto Rico, School of Medicine](https://epos.myesr.org/posterimage/esr/ecr2018/142067/media/746918?maxheight=150&maxwidth=150)
![Fig. 2: 3D models of the cervical spine, frontal views, depicting a persistent ossiculum terminale [a] and an os odontoideum [b]. Ossicles drawn by Dr. Alexandra Pérez Pérez.
References: Alexandra Pérez Pérez; Modified Essential Anatomy 2nd Edition models](https://epos.myesr.org/posterimage/esr/ecr2018/142067/media/746919?maxheight=150&maxwidth=150)
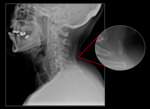
![Fig. 5: Sagittal [a] and coronal [b] CT images demonstrating a persistent ossiculum terminale, or Bergmans’s ossicle. Due to failure of fusion with odontoid process (normal in size). Typically asymptomatic and should not be confused with a type I odontoid fracture.
References: University of Puerto Rico, School of Medicine](https://epos.myesr.org/posterimage/esr/ecr2018/142067/media/746922?maxheight=150&maxwidth=150)
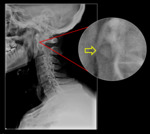
![Fig. 6: Coronal [a] and sagittal [b] CT reconstructions demonstrating an os odontoideum, seen as a smooth bony, well-corticated, structure superoanterior to the base of the dens. The most common developmental anomaly of the odontoid process, not to be confused with a type 2 odontoid fracture.
References: University of Puerto Rico, School of Medicine](https://epos.myesr.org/posterimage/esr/ecr2018/142067/media/746923?maxheight=150&maxwidth=150)
![Fig. 7: 3D reconstruction of the scapula and shoulder joint, viewed from above, depicting the three common types of os acromiale: pre-acromion [red], mesoacromion [yellow], and meta-acromion [light blue]. Ossicles drawn by Dr. Alexandra Pérez Pérez.
References: Alexandra Pérez Pérez; Modified from University of Puerto Rico School of Medicine](https://epos.myesr.org/posterimage/esr/ecr2018/142067/media/746924?maxheight=150&maxwidth=150)
![Fig. 8: T1-weighted coronal image [a] demonstrating an os acromiale, resembling a normal AC joint. Axial proton density fast-suppressed FSE [b] clearly demonstrating the unfused anterior acromial ossification center, typical of the os acromiale. The os synchondrosis (hollow red arrow) can be clearly distinguished from the AC joint (dashed arrow). Found in approximately 8% of the population.
References: Elizabeth Trullenque, Radiology Department, San Juan VA Hospital](https://epos.myesr.org/posterimage/esr/ecr2018/142067/media/746925?maxheight=150&maxwidth=150)
![Fig. 9: 3D reconstructions of the right elbow in lateral flexion [a] and posterior [b] views, depicting elbow ossicles: os patella cubiti [red], os supratrochleare dorsale [yellow] and the medial epicondyle accessory ossicle [light blue].
References: Alexandra Pérez Pérez; Modified from University of Puerto Rico School of Medicine](https://epos.myesr.org/posterimage/esr/ecr2018/142067/media/746926?maxheight=150&maxwidth=150)
![Fig. 10: Lateral [a] view of the left elbow with a small, oval bony structure at the medial epicondyle, indicative of a medial epicondyle accessory ossicle. Oblique view [b] of the right elbow of a different patient with a slightly larger ossicle at the same location.
References: Dr. Javier Pérez-Andreu, Hospital Metropolitano las Lomas](https://epos.myesr.org/posterimage/esr/ecr2018/142067/media/746927?maxheight=150&maxwidth=150)
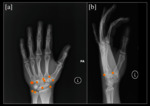
![Fig. 13: Radiograph of wrist ossicles [a] depicting the location of an os hamuli proprium [star]. 3D reconstruction of the left hand with graphic representation of an os hamuli proprium, seen in lateral [b] and palmar [c] views. Ossicles drawn by Dr. Alexandra Pérez Pérez.
References: Alexandra Pérez Pérez; Modified from University of Puerto Rico School of Medicine](https://epos.myesr.org/posterimage/esr/ecr2018/142067/media/746930?maxheight=150&maxwidth=150)
![Fig. 14: PA views of the right [a] hand of a patient with a persistent ulnar styloid, seen in the place of a normally contoured ulnar styloid. Left [b] hand of a different patient with a lunula ossicle, seen distal to the tip of the styloid.
References: Dr. Vidal-Font, Hospital Pavia-Santurce](https://epos.myesr.org/posterimage/esr/ecr2018/142067/media/746931?maxheight=150&maxwidth=150)
![Fig. 18: 3D reconstruction palmar aspect [a] and dorsal aspect model [b] of the left hand with graphic representation of an os paratrapezium, seen between the disto-radial aspect of the trapezium and the radial base of the first metacarpal. Ossicles drawn by Dr. Alexandra Pérez Pérez.
References: Alexandra Pérez Pérez; Modified from University of Puerto Rico School of Medicine](https://epos.myesr.org/posterimage/esr/ecr2018/142067/media/746935?maxheight=150&maxwidth=150)
![Fig. 19: Lateral [a] and PA [b] views of the left hand of a male patient demonstrating an os radiostyloideum adjacent to the radial styloid and lateral to the scaphoid. Incidentally noted persistent ulnar styloid is also visualized (yellow arrow). References: Dr. Vidal-Font, Hospital Pavia-Santurce](https://epos.myesr.org/posterimage/esr/ecr2018/142067/media/746936?maxheight=150&maxwidth=150)