Main modifications in the updated Head and Neck TNM classification with relevance to radiologist:
-
Separate classifications for clinical and pathological neck nodes
-
New classification for high-risk human papillomavirus-associated cancer of the oropharynx (Oropharynx p16+).
-
T or N modifications: .Oral cavity .Nasopharynx .Inclusion of extranodal extension
NEW CLASSIFICATION OROPHARYNX P16+.
The key update is the new staging for high risk human papillomavirus (HPV)-related oropharyngeal cancer distinguishing it from oropharyngeal cancer due to other causes.
The incidence of HPV-HNC has risen radically in the last decades,
in contrast with the incidence of HPV-negative HNC,
which is typically associated with tobacco and alcohol abuse.
Among all papillomaviruses,
HPV-16 is the most frequent one involved in oropharyngeal cancer.
Several studies have demonstrated that HPV+ carcinomas are associated with better prognosis and smaller risk of lymph node metastasis.
Usually HPV+ cancers are well differentiated; they show better response to treatment; better long- term survival and lower risk of death and relapse.
(2)That’s why it was indispensable to have a new staging system for HPV-related oropharyngeal cancer,
and in the 8th Edition of the TNM Classification for Head and Neck Cancer,
the Pharynx tumors have been divided in 3 chapters: Nasopharynx; Oropharynx HPV p16 positive; and Oropharynx HPV p16 negative and hypopharynx.
The diagnostic test to differentiate the two types of cancer of the oropharynx is based on detecting by immunohistochemistry,
the overexpression of the protein tumor suppressor p16.
Changes in oropharyngeal HPV-p16 positive cancer. Table 1, Table 2 and Table 3.
Between the main changes in the T staging of Oropharynx p16 positive tumors,
it should be noted that the p-16 positive classification doesn’t include carcinoma in situ (Tis),
and the T4b category has been removed because the survival curves of the T4a and T4b were identical.
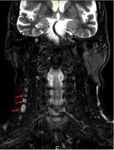
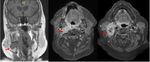
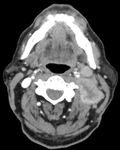
Among the N category,
there are changes in the size of the lymph nodes; It has been proven that unilateral nodes smaller than 6 cm in size have the same impact on survival,
so if there are unilateral metastasis in lymph node(s),
all 6 cm or less in greatest dimension they are considered as N1.
If there are contralateral or bilateral metastasis in lymph node(s),
all 6 cm or less in greatest dimension,
they are considered as N2; and if the lymph node(s) are greater than 6 cm in greatest dimension,
as N3 Fig. 1 and Fig. 2.
MODIFICATIONS IN T CATEGORY: Include nasopharynx and oral cavity.
ORAL CAVITY
The new edition of the TNM Classification for Head and Neck Cancer includes the Depth of invasion (DOI),
that differs from tumor thickness.
Although tumor thickness and depth of invasion are often used synonymously,
they are different terms.
Tumor thickness refers to the thickness of the entire tumor mass,
and DOI means the extent of cancer growth into the tissue beneath an epithelial surface.
(3) More recent data suggest that DOI is a better predictive parameter than tumor thickness as it differentiates between superficial or exophytic tumors and those that are more invasive.
(4) DOI reflects more accurately the proximity of the injury to the blood and lymphatic vessels,
and predicts more precisely the risk of hematogenous or lymphatic spread.
In cases in which the epithelium is destroyed or the tumor is exophytic,
some studies draw a surface line in the CT or MR and measure the DOI from this line Fig. 3 .
In the 8th TNM edition,
T category of the oral cavity cancer considers DOI and greatest dimension of the tumor Table 4 .
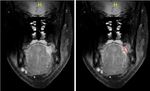
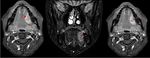
A depth of invasion of 5 mm has been used as the “cutting point”,
so tumors of 2 cm or less in greatest dimension and 5 mm or less of DOI are staged as T1,
tumors between 2 and 4 cm and/or DOI between 5 mm and 10 mm are staged as T2; and for sizes greater than 4 cm or DOI higher than 10 mm,
T3 Fig. 4 and Fig. 5 .
DOI can be measured on MRI and CT,
but the lack of precision in the definition and the lack of clear criteria to measure it in the imaging techniques limit its use.
It is important to further investigate to reach consensus among institutions regarding a precise definition of DOI,
and unify the criteria to measure it from the radiological approach.
NASOPHARYNX
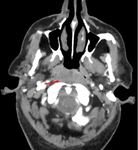
The main changes in the Nasopharynx category in the 8th edition of TNM focus on a more accurate anatomical description for staging Table 5 : The terms “infratemporal fossa” and “masticator space” are replaced by a specific description of the anatomical structures involved.
Medial and lateral pterygoid muscles involvement changes from T4 to T2 and prevertebral muscle involvement is also staged as T2 Fig. 6 .
MODIFICATIONS IN N CATEGORY: extranodal extension and nasopharynx.
EXTRANODAL EXTENSION.
Another significant change in the updated TNM edition is the inclusion of the extranodal extension (ENE) with separate classifications for clinical and pathological ENE.
The new criteria are incorporated to the N category of oral cavity,
Oropharynx p16- and Hypopharynx and Larynx.
In Oropharynx p16 + and nasopharynx they are not included.
ENE has been added as a prognostic variable for regional lymph node metastases in addition to the number and size of metastatic lymph nodes Table 6 .
(4)
Although there are not many studies done on extranodal extension,
it’s thought that current imaging modalities have limitations in their ability to identify ENE,
and that radiologic evidence alone is not enough (5).
Therefore,
the clinical evidence for ENE includes only unambiguous ENE,
as determined by physical examination (invasion of skin,
infiltration of musculature/dense tethering to adjacent structures,
or dysfunction of a cranial nerve,
the brachial plexus,
the sympathetic trunk,
or the phrenic nerve),
and supported by radiological evidence.
New revisions have demonstrated that CT findings suggesting ENE predicts treatment response and prognosis,
and could be used to determine the treatment modality for HNC.
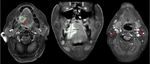
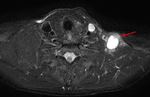
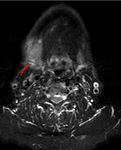
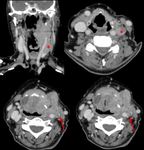
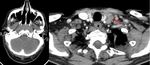
(5) The criteria that can help us to identify extranodal extension on radiological imaging studies are: enhancement,
thickening and irregularity of nodal rim; blurred border and/or infiltration of the adjacent fat or other soft tissue planes; as infiltration of the sternocleidomastoid muscle,
internal jugular vein,
or carotid artery (6).
Therefore,
in N category,
extranodal extension will be taken into account,
in addition to the size of the lymph nodes,
defining the N3b staging as the one which presents extranodal extension Fig. 7,
Fig. 8, Fig. 9 and Fig. 10 .
NASOPHARYNX
The term supraclavicular fossa is replaced,
so lymph nodes are classified according to whether they are located above or below the inferior border of the cricoid cartilage.
Additionally,
there is no separation between stage N3a and N3b.
Table 7 and Fig. 11 .