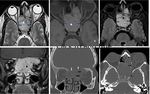
- We present the imaging features of some of the cases of paranasal sinus tumors from a case series comprising of 35 cases imaged over a period of 4 years in a tertiary centre.
- All of them underwent a CT scan of paranasal sinuses while some of them also had additional contrast enhanced CT and MRI for further assessment.
- All cases were correlated with histopathology. Of the 35 cases,
20 were benign tumors,
7 were malignant tumors and the rest comprised of antrochoanal polyp (2),
sinonasal polyposis (5) and indeterminate granulomatosis (1).
Inverted papilloma (5),
fibrous dysplasia (4) and osteoma (4) were the common benign tumors in our case series whereas sinonasal carcinoma (2) was the most common malignant tumor.
Neurogenic tumors (3),
aneurysmal bone cyst (1),
juvenile nasopharyngeal angiofibroma (3),
chondrogenic osteosarcoma (1),
lymphoma (1),
neuroendocrine tumor (1),
solitary intramedullary plasmacytoma (1) and metastatic deposit(1),
were the other lesions we encountered.
- CT is the best modality to evaluate bony changes such as cortical erosion,
destruction,
remodelling,
sclerosis and thickening of bone.
Reconstruction with both a bone and soft tissue algorithm,
slice thickness of 1 mm,
reformatting in three planes and post contrast imaging are important for optimal evaluation of tumor extent.
- The basic MR protocol in imaging sinonasal tumors is unenhanced T1 and T2,
post contrast T1 with fat saturation in order to characterize the soft tissue components of the tumour and to evaluate the extent of tumour invasion beyond the bony sinus walls.
DWI is valuable in differentiating recurrent tumor from surrounding edema.
MR is superior to CT with regard to orbital,
dural invasion and perinural spread.
- 18F fluoro deoxyglucose (FDG)-positron emission tomography (PET)/CT imaging is not recommended for routine diagnosis and staging of head and neck cancer in most guidelines[4],
however,
it has been shown to be useful for imaging of residual and recurrent tumor[5],
in monitoring treatment response[4],
to measure tumour volume [6],
and to select patients who may benefit from oxygenation modifying treatments[6].
BENIGN TUMORS:
OSTEOMA:
Os Osteomas are the most common benign sinonasal tumor and are usually incidental findings at paranasal sinus CT.
The frontal sinus bone is the most common location,
followed by the ethmoid and maxillary sinus bone [7].
At CT,
osteomas may demonstrate both dense cortical bone and groundglass appearance [Fig.
1 (A,B)] and mimic fibrous dysplasia.
FIBROUS DYSPLASIA:
Craniofacial involvement may occur both as true craniofacial fibrous dysplasia,
considered a form of monostotic fibrous dysplasia (despite multiple cranial bones being affected) or as part of polyostotic fibrous dysplasia.
The radiological findings show three patterns: pagetoid,
sclerotic and cystic; the pagetoid form [Fig.2 (A,B)],
with bone expansion and mixed areas of sclerosis and cystic areas,
is the most common.
CT usually shows a characteristic ground glass pattern but on MR imaging the metabolically active fibrous tissue may enhance markedly at contrast-enhanced T1and therefore can be misinterpreted as a malignant tumor[8].
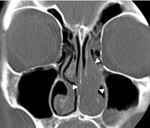
INVERTED PAPILLOMA:
Inverted papillomas (IP) are the second most common benign sinonasal tumor; however they are still rare,
accounting for only 0.5–4.0% [9] of primary sinonasal tumors. Unlike nasal polyps,
IPs are almost always unilateral lesions,
and a common CT feature is advanced unilateral ethmomaxillary sinus opacification that remodels or demineralizes the bone and with medial bulging into the nasal septum.
The site of origin of an IP may be detected as focal hyperostosis on the sinus wall at CT (Fig.
3E,F) [10].
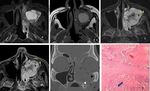
Follow-up MR imaging demonstrates the characteristic mucosal infoldings,
described as a “convoluted cerebriform pattern” on both T2 [Fig.3(C,D)] and contrast-enhanced T1 sequences [11] ,
differentiating tumor from the surrounding mucus and thickened mucosal lining.
INVERTED PAPILLOMA WITH SINONASAL CARCINOMA:
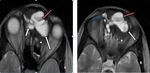
Sinonasal carcinoma may arise in IPs [Fig.4(A-D)] ; it is more prevalent in males,
non-keratinising squamous cell carcinoma is the most common ( 10) % histological variety and tumors originating in frontal sinus or frontal recess are most frequently associated [12].
Malignant degeneration of IP and smoking are associated with increased risk of recurrence after surgical resection [13].
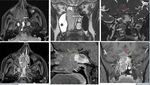
JUVENILE NASOPHARYNGEAL ANGIOFIBROMA:
Juvenile nasopharyngeal angiofibroma (JNA) is a benign,
but locally aggressive tumor and arising from testosterone-sensitive cells at the pterygoid plates in the pterygopalatine fossa and therefore these tumors are only seen in adolescence males.
From its origin in the pterygopalatine fossa,
the tumors grows in all directions,
medially through the sphenopalatine foramen into the nasal cavity,
laterally through the pterygomaxillary fissure,
and cranially to the inferior orbital fissure into the orbital apex and then continues through the superior orbital fissure and into the middle cranial fossa[15].
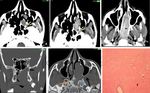
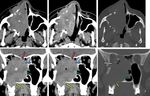
The characteristic imaging pattern at CT is broadening of the pterygopalatine fossa [Fig.5 (B,E)] with enlargement of the sphenopalatine foramen medially and the vidian canal posteriorly [Fig.5 (E)].
At MR imaging,
due to the high vascularity,
the tumor shows typical flow voids and intense enhancement on T1 after gadolinium injection.
SCHWANNOMA:
Sinonasal schwannomas are benign,
usually solitary,
slow-growing nerve sheath tumors.
Although rare,
they should be considered in the differential diagnoses.
The lesion most commonly arises in the ethmoid and maxillary sinuses,
with two cases having been reported in the sphenoid sinus.
There are no reported cases of frontal sinus schwannoma. They can arise both from the ophthalmic or maxillary branches of the trigeminal nerve,
fila olfactoria beyond the level of olfactory bulb or from autonomic nerves.
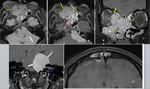
At CT,
schwannomas are sharply delineated expansile lesions that remodel bone.
If large,
they can invade vital structures.
At MR imaging,
they have high signal intensity at T2 and at T1 they are isointense to muscle with a low-signal capsule.
After intravenous contrast medium,
strong homogeneous enhancement is usually seen [Fig.
6 (B,C,D)]
ANEURYSMAL BONE CYST:
Aneurysmal bone cyst may be seen in the maxilla,
ethmoid,
sphenoid bone and periorbital region.
It appears as an expansile,
multi-locular “soap bubble” (honey comb) radio-lucency,
causing expansion of the bony cortex.
MR imaging commonly shows cystic spaces with internal septa and septal contrast enhancement.
Fluid-fluid levels [Fig-7 (A,B)] of varying intensities is characteristic but should not be considered diagnostic,
as this finding might be present in giant cell tumor,
telangiectatic osteosarcoma,
and chondroblastoma .
AMELOBLASTOMA:
Ameloblastomas are locally aggressive benign odontogenic tumors that arise from the mandible,
or,
less commonly,
from the maxilla. They are expansile,
radiolucent uni or multilocular with characteristic soap bubble appearance at panoramic radiography or CT.
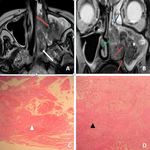
AT MRI they demonstrate a mixed solid and cystic pattern [Fig.8 (A,B)] ,
with a thick irregular wall,
often with vividly enhancing solid components [Fig.8 D]
MALIGNANT TUMORS:
SINONASAL CARCINOMA:
Squamous cell carcinoma is the most common malignant sinonasal tumour (80%),
followed by adenocarcinoma and undifferentiated type.
Squamous cell carcinomas most often originate from the maxillary sinuses and demonstrate low signal intensity at T2.
Intestinal and low grade non-intestinal type adenocarcinomas have a higher tendency to affect ethmoid sinus and nasal cavity,
whilst high grade non-intestinal type adenocarcinomas more frequently affect the maxillary sinuses.
Undifferentiated sinonasal carcinomas also most frequently arise from the ethmoid sinus and superior nasal cavity.
These tumors are usually large at presentation with aggressive bone destruction [Fig.9( C,F)],
isointense on T1,
variable signal intensity at T2 and show heterogeneous contrast enhancement on post contrast T1 images.
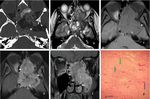
CHONDROSARCOMA:
Chondrosarcoma is the most common sarcoma affecting the paranasal sinuses.
At CT,
the tumour is seen as a multilobulated,
heterogeneous lesion consisting of a chondroid matrix with peripheral and scattered central calcifications.
Using MR imaging,
the high water content of the chondroid matrix presents with high signal on T2 [Fig.
11(b)] and low signal on T1; calcifications of the chondroid matrix cause signal voids at all sequences.
The intra-tumoral septum shows low signal at both T1 and T2 with heterogeneous pattern at post contrast study due to septal enhancement,
but the avascular chondroid matrix is unchanged [Fig.
11(c)].
CHONDROGENIC OSTEOSARCOMA:
Fewer than 10% of osteosarcomas arise in the craniofacial bones with most such tumors developing in the mandible and maxilla,
osteosarcoma arising from sphenoid sinus is very rare.
Most commonly they involve medullary cavity rather than bone surface.
Chondrogenic osteosarcoma is a histological subgroup characterized by immature chondroid tissue with lacy osteoid matrix.
On CT,
most often there is lytic bone destruction with soft tissue infiltration and mineralization of osteoid matrix lFig.12A],
rarely the bone margin may remain intact (low grade),
may show sclerosis (osteogenic) or sunburst (radiating mineralized tumor spicules pattern).
On MRI,
they are of low to intermediate signal on T1W and high signal on T2W [Fig-12B] images with variable contrast enhancement [ Fig.12 (D,E)].
LYMPHOMA:
Lymphomas in the sinonasal cavities have worse outcome than lymphomas in other regions.
Lymphomas can be classified into Hodgkin and non-Hodgkin’s type,
the latter again subclassified by the group of dominating cells into B,
T,
NK cell lymphoma .
B-cell lymphomas are most common in the maxillary sinus and have a better prognosis than T-cell lymphomas,
which more often originate from the nasal septum.
Lymphoma may present as chronic indolent tumor mimicking invasive fungal sinusitis.
At CT and MR imaging,
lymphomas can present with diffuse tumour infiltration along the walls of the nasal cavity or as large bulky masses on both sides of the sinus wall,
with remodelling or erosion of the adjacent bone [Fig.
14(a–d)].
Lymphomas are isodense to muscle at CT,
and at MR imaging,
the signal is isointense to muscle on T1 and moderate to high on T2.
Both at CT and MR imaging,
the contrast enhancement of lymphomas can be variable and not discriminated from other malignancies,
e.g.
squamous cell carcinoma.
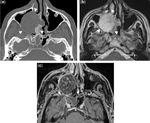
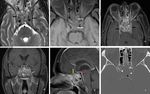
NEUROENDOCRINE TUMORS:
Olfactory neuroblastoma (esthesioneuroblastoma) is the the most differentiated histological phenotype of neuroendocrine tumors and ,
most commonly arises at the superior nasal fossa with bimodal age distribution.
At CT and MR imaging ONB may present as a homogeneous,
solitary nasal polyp that remodels rather than destroys the bone [Fig.
15( A–F)].
The MR signal is intermediate on both T1 and T2,
and after intravenous contrast medium,
there is intermediate to high enhancement of the tumour.
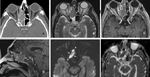
Sinonasal neuroendocrine carcinoma (SNEC),
sinonasal undifferentiated carcinoma (SNUC),
and small cell undifferentiated carcinoma (SmCC)[ Fig.16 ( A-E)] [15] are the other aggressive phenotypes with bone erosion similar to that of squamous cell carcinoma,
and the correct diagnosis can only be done by immunohistologic examination[15].
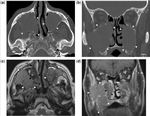
SOLITARY INTRAMEDULLARY PLASMACYTOMA:
Solitary intramedullary plasmacytoma occurs more commonly in the sphenoid sinus and the maxilla with male preponderance.
It is a fairly well defined expansile lesion with contrast enhancement [Fig.17 ( A-E)].
It exhibits low signal intensity on T1-weighted images and high or mixed signal intensity on T2-weighted images with marked contrast enhancement that may simulate meningioma.
SALIVARY GLAND TUMORS:
Adenoid cystic carcinoma (ACC) is the most common salivary gland tumor with its origin usually in the maxillary or ethmoid sinuses.
Low-grade ACC may present as an ethmoid polyp that remodels bone and mimics a simple polyp [Fig.
18] at both CT and MR imaging; high-grade ACC may present as a large irregular mass with bone destruction and irregular density and signal at CT and MR imaging.
ACC is well known for its predisposition to perinural spread along the cranial nerves that can proceed into the skull base which is best appreciated at contrast enhanced MR imaging.
MUCOSAL MALIGNANT MELANOMA:
MMM is an aggressive tumour with high rate of recurrence and most commonly arises from nasal septum.
At CT,
MMM can be seen as a polypoid lesion in the nasal cavity with bony remodelling or erosion [Fig.19 ( A,B)] and usually there is bright post contrast enhancement.
At MR imaging,
the lesion is homogeneous,
and may demonstrate characteristic high T1 and low T2 signals due to presence of melanin and/ or hemorrhage.
METASTASIS:
Metastasis is uncommon in paranasal sinus.
Renal cell carcinoma is the most frequent tumor to metastasize to the paranasal sinuses whilst maxillary sinus is the most frequently involved.
Metastasis may appear as a localized,
well-defined radiolucent slow growing lesion,
or it may be highly aggressive with cortical destruction [Fig.20 ( E,F)],
osteoblastic in breast cancer or mixed lytic or sclerotic in patients with prostate cancer.
They may exhibit low signal intensity on T1-weighted images,
high signal intensity on T2-weighted images [Fig.20A] with heterogeneous post contrast enhancement [Fig.20 (C,D)].

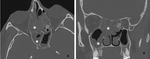
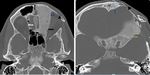
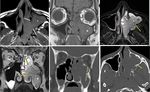
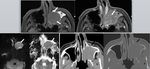
![Fig. 19: (a) Coronal CT demonstrates advanced sinonasal opacification with erosion of the right olfactory fossa and lateral lamella (arrow) due to mucosal malignant melanoma. (b) Coronal CT after surgical treatment still shows bilateral advanced opacification and (c) coronal [18F]FDG-PET/CT confirmed residual or recurrent tumour in the right anterior ethmoid sinus (arrow). Notice also physiologic FDG uptake in the brain and in the lateral and inferior eye muscles. References: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3362868/](https://epos.myesr.org/posterimage/esr/ecr2018/143212/media/762812?maxheight=150&maxwidth=150)