Type:
Educational Exhibit
Keywords:
Education and training, Education, MR, CT, Conventional radiography, Musculoskeletal bone, Bones, Anatomy
Authors:
A. N. Pérez Pérez1, A. P. Marrero González2, J. R. Ortiz-Cruz1, J. Lugo-Rosado2, E. Trullenque1, J. Vidal1; 1San Juan, PR/US, 2San Juan, Puerto Rico/US
DOI:
10.1594/ecr2018/C-2377
Findings and procedure details
HIP AND KNEE
-
Diagrammatic overview
-
Fig. 1 and Fig. 2
-
Pictorial review
-
Os acetabuli
-
-
Prevalence: 3%[1]
-
Location: Adjacent to the acetabular rim
-
Overview: Or os acetabulare,
an unfused secondary ossification center at the acetabular rim.
Also thought to represent a rim fracture fragment secondary to a cam type femoroacetabular impingement (FAI).
[2,3] Studies have proposed that “true” os acetabuli have cartilagenous growth plates more parallel to the joint surface,
whereas FAI acetabular rim fragments growth plates are more perpendicular to the joint surface.
[2,4] May be misdiagnosed as a fractured osteophyte,
acetabular chondro-ossification or prior acetabular fractures.[1]
-
Radiographic characteristics: Usually rounded with a concave lateral border and convex medial border.
May be bilateral and/or fused to the acetabulum.
AP pelvis,
false profile and Dunn views of the hip are recommended to fully characterize the femoral and acetabular anatomy.[5]
-
*See Fig. 1 for diagram and Fig. 3 for case
-
Os fabella
-
-
Prevalence: 10-30%; 63-85% bilateral; [6] higher rates in Asian population (66-87%).[7]
-
Location: Lateral head of the gastrocnemius (rarely in the medial head) articulating with the lateral or medial femoral condyle.
[6,8]
-
Overview: Bilateral,
bipartite,
tripartite or double.
May cause posterolateral femoral pain exacerbated by direct pressure,
known as fabella syndrome, due to friction between the fabella and the posterolateral femoral condyle.
[1,2] Has been shown to present with common fibular nerve palsy.
[7] May be misdiagnosed as a loose body.
-
Radiographic characteristics: Elliptical or circular in shape and may vary in size,
from 3.5-13.5 mm in length,
2-9 mm in width and 1.5-10 mm in depth.[6] Best visualized in lateral radiographs of the knee.
-
*See Fig. 2 for diagram and Fig. 4 for case
-
Cyamella
-
-
Prevalence: Extremely infrequent in humans
-
Location: Within the popliteus tendon,
at the popliteus myotendinous junction.[1,9]
-
Overview: Also known as the popliteal fabella,
or fabella distalis.
Articulates with the posterior surface of the lateral femoral condyle.[6] Considered to be a sesamoid bone,
as it lies within the popliteus tendon.[2,6] Seen in approximately 84% of dogs,
100% of cats and decreases in prevalence in higher primates and humans.[10] Rarely shown to cause symptoms,
with one case report citing sesamoiditis with pseudo-locking and clicking.
May be misdiagnosed as an intra-articular loose body,
a fabella,
or heterotopic ossification.[2,9]
-
Radiographic characteristics: Best seen on AP radiographs of the knee,
most commonly found within the lateral femoral groove.
[3] On T1,
T2 and T2*-weighted MR images,
the cyamella appears as an ossicle with low signal intensity along its borders.
[9]
-
*See Fig. 2 for diagram and Fig. 5 and Fig. 6 for case
-
Meniscal ossicle
-
-
Prevalence: 0.15%.[3]
-
Location: Posterior horn,
within medial meniscus[6]
-
Overview: Three theories as to its origin: it is an anatomical variant,
it is a post-traumatic result of heterotopic ossification,
or it is the product of mucoid degeneration.[2] Composed of mature lamellar and cancellous bone,
surrounded by hyaline cartilage.[6] Usually incidental and asymptomatic,
but may produce diffuse pain and a locking sensation,
mimicking a torn meniscus or an intra-articular loose body.[3] Should not be confused with an avulsion of the PCL.
-
Radiographic characteristics: Best seen on AP radiographs.
Lateral views have shown that the ossicle moves with the tibia during knee rotation.[6] MR imaging is useful in differentiating it from common misdiagnoses, exhibiting marrow intensity on all sequences,
with a surrounding peripheral rim of low signal intensity,
corresponding to its cortex.[2,3]
-
*See Fig. 2 for diagram and Fig. 7 for case
FOOT
-
Diagrammatic overview
-
Fig. 8
-
Pictorial Review
***See Table 1 and Table 2 for complete poster summary***

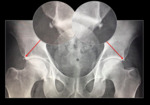
![Fig. 1: 3D reconstructions of the hip in AP [a] and oblique [b] positions. Highlighted by red and yellow arrows are graphic representations of bilateral os acetabuli. Ossicles drawn by Dr. Alexandra Pérez Pérez.
References: Alexandra Pérez Pérez; Modified from University of Puerto Rico School of Medicine](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750020?maxheight=150&maxwidth=150)
![Fig. 2: 3D reconstructions of the knee in AP [a] and lateral [b] positions. Graphic representations of os cyamella [yellow], meniscal ossicle [light blue] and fabella [red] have been drawn, highlighting their typical locations. Ossicles drawn by Dr. Alexandra Pérez Pérez.
References: Alexandra Pérez Pérez; Modified from University of Puerto Rico School of Medicine](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750021?maxheight=150&maxwidth=150)
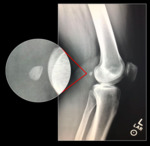
![Fig. 5: AP [a] and lateral [b] views of the right knee of a male patient with a unilateral cyamella. Best seen on AP view
References: Dr. Javier Pérez-Andreu, Private Practice, Fajardo, Puerto Rico](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750024?maxheight=150&maxwidth=150)
![Fig. 7: T1W sagittal MR view of the left knee [a] demonstrating a meniscal ossicle seen within the posterior horn of the medial meniscus [yellow arrow]. Lateral plain film of the left knee [b] of the same patient with visible bony structure, representing meniscal ossicle. References: Dr. Elizabeth Trullenque, Radiology Department, San Juan VA Hospital](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750025?maxheight=150&maxwidth=150)
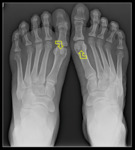
![Fig. 8: Lateral [a] and AP [b] views of the left foot reviewing some common foot accessory ossicles: (1) os trigonum, (2) os vesalianum pedis, (3) os peroneum, (4) os subtibiale, (5) calcaneus secundarius, (6) os intermetatarseum, (7) os supratalare, (8) hallux sesamoids, (9) os supranaviculare(10) os tibiale externum, (11) os subfibulare References: Alexandra Pérez Pérez; Modified from University of Puerto Rico School of Medicine](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750026?maxheight=150&maxwidth=150)
![Fig. 9: Symptomatic os trigonum with associated edema seen in lateral MR images of foot, STIR [a] and T1W [b] sequences. Os trigonum seen at the posterior process of the talus in lateral radiograph of foot [c]. Present in approximately 7% of adults. References: University of Puerto Rico, School of Medicine](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750027?maxheight=150&maxwidth=150)
![Fig. 10: Right foot oblique [a] and DP [b] views of a 27-year-old male patient presenting with right foot pain. Os vesalianum (pedis) visualized as ossification next to the base of the fifth metatarsal bone. References: Dr. Elizabeth Trullenque, Radiology Department, San Juan VA Hospital](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750028?maxheight=150&maxwidth=150)
![Fig. 11: Lateral [a] and AP [b] radiographs of the right foot with an os peroneum, seen in 26% of the population. References: Dr. Elizabeth Trullenque, Radiology Department, San Juan VA Hospital](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750029?maxheight=150&maxwidth=150)
![Fig. 12: 3D oblique [a] and frontal [b] models of the left foot, depicting the typical location of the os subfibulare beneath the tip of the fibula. Ossicles drawn by Dr. Alexandra Pérez Pérez. References: Alexandra Pérez Pérez; Modified Essential Anatomy 2nd Edition models](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750030?maxheight=150&maxwidth=150)
![Fig. 13: 3D oblique [a] and frontal [b] models of the left foot, depicting the typical location of the os subtibiale beneath the tip of the medial malleolus. Ossicles drawn by Dr. Alexandra Pérez Pérez. References: Alexandra Pérez Pérez; Modified Essential Anatomy 2nd Edition models](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750031?maxheight=150&maxwidth=150)
![Fig. 14: 3D oblique [a] and lateral [b] models of the left foot, depicting the typical location of the os calcaneus secundarius, at the anteromedial border of the calcaneus, cuboid, talar head and tarsal navicular bones. Ossicles drawn by Dr. Alexandra Pérez Pérez. References: Alexandra Pérez Pérez; Modified Essential Anatomy 2nd Edition models](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750032?maxheight=150&maxwidth=150)
![Fig. 15: Bilateral os intermetatarseum, seen freestanding in left [a] lateral foot radiograph and articulating in right [b] lateral foot radiograph. Most commonly located superiorly between the bases of the first and second metatarsals, with an incidence of approximately 4% in the general population. References: Dr. Elizabeth Trullenque, Radiology Department, San Juan VA Hospital](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750033?maxheight=150&maxwidth=150)
![Fig. 16: 3D oblique [a] and lateral [b] models of the left foot, depicting the typical location of the os supratalare, at the dorsal aspect of the talar neck. Ossicles drawn by Dr. Alexandra Pérez Pérez. References: Alexandra Pérez Pérez; Modified Essential Anatomy 2nd Edition models](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750034?maxheight=150&maxwidth=150)
![Fig. 18: Os supranaviculare [yellow arrow], seen in only 1-5% of people, and os trigonum [orange arrow] in a lateral radiograph of a male patient’s right foot. References: Dr. Vidal-Font, Hospital Pavia-Santurce](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750036?maxheight=150&maxwidth=150)
![Fig. 19: Os tibiale externum (accessory navicular or os naviculare accessorium). Oblique view of unilateral accessory navicular, type I [a], accounting for approximately 30% of cases. Different male patient with bilateral ossicles seen in DP view; type II [b] , accounting for approximately 60% of cases, and type III [c], accounting for the remaining 10%. References: Dr. Elizabeth Trullenque, Radiology Department, San Juan VA Hospital](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/750037?maxheight=150&maxwidth=150)

![Fig. 6: MRI [a] and lateral plain film [b] of the right knee of a different patient, demonstrating a unilateral cyamella, seen with low signal intensity borders on MRI. Note the location at the popliteus myotendinous junction. References: Dr. Elizabeth Trullenque, Radiology Department, San Juan VA Hospital](https://epos.myesr.org/posterimage/esr/ecr2018/142096/media/770795?maxheight=150&maxwidth=150)
