(The results of our study are shown in figure 1).
Our study included a total of 62 patients,
with a mean age of 71 years old (standard deviation 11 years).
The male-to-female ratio was 1,8:1.
Forty patients had smoking history (64,5%),
with a median of 40 pack-years.
Life-limiting comorbidities (cancer,
ischemic cardiopathy,
stroke,
degenerative disease,
history of a high-risk surgery) were present in 21 patients (33,8%).
Functionally,
the patients had preserved FVC (mean of 93,3% of the expected value) and mild-to-moderate decrease of DLCO (65,8%). Exercise condition was also preserved,
with a mean of 433 meters in the 6 minute walking test and a mean of minimum oxygen saturation of 94%.
At initial chest HRCT,
only 6 patients (9,7%) presented UIP pattern,
classically described as the presence of reticulation and honeycombing in a subpleural and basal distribution,
and absence of features inconsistent with UIP.
Possible UIP and inconsistent with UIP pattern were present respectively in 15 (24,4%) and 41 patients (66,1%).
Emphysema at CT was described in 16 patients (25,8%).
Lung biopsy was performed in 24 patients.
The most common method used was surgical biopsy,
followed by cryobiopsy and percutaneous (tru-cut).
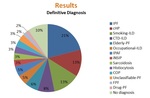
Definitive diagnosis was achieved in the 90,3% (56) of cases,
being the remaining 9,7% of cases of unknown diagnosis when this review was written.
The diseases diagnosed by frequency order were (fig.
2):
- Idiopathic Pulmonary fibrosis (IPF): 21%
- Chronic Hypersensitivity Pneumonitis (cHP): 13%
- Smoking-related ILD: 13%
- Connective Tissue Disease (CTD) – ILD: 8%
- Elderly Pulmonary Fibrosis (Elderly PF): 6%
- Occupational ILD: 5%
- Interstitial pneumonia with autoimmune features (IPAF): 5%
- Idiopathic Non-Specific Interstitial Pneumonia: 3%
- Sarcoidosis: 5%
- Histiocytosis: 3%
- Cryptogenetic Organizing Pneumonia: 3%
- Unclassifiable PF: 3%
- Familiar PF: 2%
- Drug-related PF: 2%
Fibrotic ILD
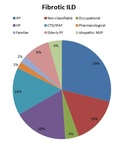
Fibrotic ILD was diagnosed in 45 patients (72,6%).
By frequency order,
the fibrotic diseases were (fig.
3):
- IPF: 29%
- cHP: 18%
- CTD-related ILD/IPAF: 16%
- Non-classifiable: 16%
- Elderly PF: 9%
- Idiopathic NSIP: 4%
- Occupational: 4%
- Pharmacological: 2%
- Familiar: 2%
Autoimmune - related ILD (fig.
4) included four cases of CTD - related ILD (2 rheumatoid arthritis and 2 scleroderma) and three interstitial pneumonia with autoimmune features,
according to recent diagnostic statements [1].
Elderly Pulmonary Fibrosis was diagnosed in four patients.
In this group,
the mean age was significantly higher (85 y.o.),
with milder alteration on PFT.
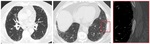
On figure 5,
an example of a 78 year old man with a mild interstitial pattern,
asymptomatic and without significant alteration of PFT.
An initial CT performed in 2014 shows a fine subpleural reticular pattern,
with some septal thickening but no superimposed bronchiectasis [2].
A CT performed in 2016 showed radiologic stability.
Chronic Hipersensitivity Pneumonitis (cHP) was diagnosed in 8 patients (18%).
Practically all cases presented a pattern inconsistent with UIP at initial HRCT,
most of them with centrilobular nodules,
ground-glass opacities,
air-trapping and ‘UIP-unlike’ fibrosis (non-peripheral and with upper zone predominance) [3].
One patient showed possible UIP pattern (subpleural reticulation with basal predominance,
but without bronchiectasis or honeycombing).
See on figures 6 and 7 different radiologic appearances of cHP.
Undetermined fibrotic ILD represented the 16% of patients,
currently without diagnosis.
Idiopathic fibrotic NSIP was diagnosed in two patients (4%).
On figure 8,
an example with extensive ground-glass opacities and septal thickening predominantly in the periphery,
and severe bronchiectasis [4].
Occupational fibrotic ILD was diagnosed in two patients (4%),
one with an inconsistent UIP pattern (air-trapping and reticulation),
and another with subpleural reticulation in a basal predominance,
but with extensive GGO and centrilobular nodules,
who had smoking history and exposure to aluminium and silica.
A lung biopsy showed combined pneumoconiosis with anthracotic predominance.
Pharmacological-related ILD was diagnosed in one patient (2%) with long-time exposure to amiodarone and a UIP pattern in HRCT (fig.
9).
One case of Familiar Pulmonary Fibrosis (2%) was diagnosed in a 60 year old woman,
who had two siblings who died of pulmonary fibrosis,
and proven telomere shortening at genetic tests.
At HRCT,
predominant GGO in association with bronchiectasis but without subpleural distribution or basal predominance configured a non-UIP pattern (fig.
10).
Lung biopsy disclosed a NSIP pattern.
The median time from the visit request to the first visit was of 2,2 months,
and that between the first visit and the diagnosis was of 4,6 months.
Forty patients (64,5%) received treatment (pharmacological or not),
including 9 cases who were provided with antifibrotic drugs,
18 with immunomodulation (42.5%) and other therapies (avoidance of smoking or known antigen) in 14 patients (35%).
4 of the patients (6,5%) included in the study died.
IPF group
Idiopathic Pulmonary Fibrosis is defined as a specific form of chronic fibrosing interstitial pneumonia without known cause,
occurring primarily in older adults.
The prognosis is poor,
with a mean survival of less than 5 years.
IPF is associated with a histological or radiological Usual Interstitial Pneumonia (UIP) pattern [5].
In our study,
13 patients received definitive diagnosis of IPF,
representing the 29% of all fibrotic ILD and the 21% of all patients included in this study.
The mean age in this group was 72 years.
The male-to-female ratio was of 12:1.
Life-limiting comorbidities existed in 2 patients,
one with severe ischemic cardiopathy and history of coronary surgery,
and another with concomitant lung cancer,
who died during the study.
Functionally,
this group presented similar values compared to those of the global of patients (FVC: 91,4%,
DLCO: 63,1%).
Exercise condition was also preserved (fig.
11).
Patterns observed in the initial HRCT were the following: 3 UIP,
7 possible UIP and 3 inconsistent with UIP pattern.
One patient with UIP pattern presented significant upper lobe predominant emphysema (fig.
12).
Initially,
this patient was diagnosed of Combined Pulmonary Fibrosis and Emphysema (CPFE) as functional tests were suggestive of (preserved FVC and VEMS/FVC - 121% and 75% respectively – and decreased DLCO – 46%-),
as described in some series [7,8].
However,
emphysema was not substantial enough,
and IPF was diagnosed in a patient with emphysema.
Lung biopsy was performed in 6 patients,
4 of which surgical and 2 cryobiopsy.
Histological samples were obtained in 4 cases with possible UIP pattern and in 2 cases with inconsistent with UIP pattern (fig.
13).
However,
only 4 of these cases received diagnosis due to histological results: in two of them,
the biopsy was inconclusive,
and the diagnosis was given according to the radiological or functional progression of the disease [6].
7 patients did not undergo lung biopsy (3 UIP,
3 possible UIP and 1 inconsistent with UIP pattern).
In those cases,
the diagnosis was established after multidisciplinary committee evaluation,
generally due to radiological or functional progression.
Antifibrotic treatment (Nintedanib,
Pirferidone) was indicated in 10 patients with IPF (76.9%), 9 of which underwent this therapy.
One patient rejected to start the treatment despite indication (fig.
14).
Of the remaining 3 patients,
2 presented contraindication to antifibrotic treatment due to pulmonary adenocarcinoma or advanced heart disease (fig.
15).