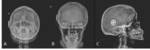
INFECTIOUS-INFLAMMATORY LESIONS
Several inflammatory conditions may affect the temporal bone.
The inflammatory diseases of the temporal bone are generally classified
according to the site of origin: external ear,
middle ear and mastoid,
petrous apex and inner ear.
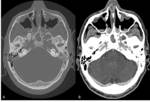
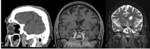
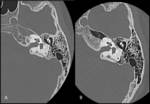
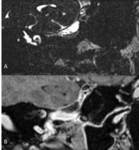
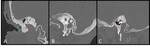
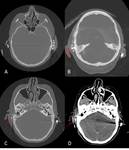
Necrotizing or malignant otitis externa occurs most commonly in elderly diabetic patients and other patients in immunocompromised states,
as an infection usually caused by Pseudomonas aeruginosa high mortality rate.
The patients present with severe otalgia and otorrhea.
Infection can then spread via fissures of Santorini into the soft tissues beneath the skull base,
leading to skull base osteomyelitis.
On images,
soft-tissue thickening in the external canal is noted,
often with bone destruction and inflammatory changes in the mastoid.
MR and CT are complementary modalities for evaluation of this entity,
with the bone windows at CT showing the destructive process to greater advantage,
and MR imaging better demonstrating associated soft tissue complications.(Figg.
7,
8,
9,10,11)
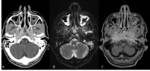
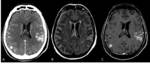
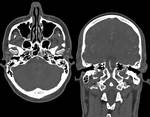
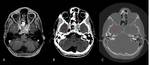
Acute otitis media (AOM) and mastoiditis are primarily diseases of infants and young children,
defined as infectious processes of the middle ear,
involving a variable portion of the mastoid air cell system.
Patients present with fever,
otalgia,
and a red bulging tympanic membrane.
AOM is often subsequent to a viral upper respiratory infection disrupting the mucosal barrier,
thus allowing bacterial inception and growth.
Reflux of infected secretions from the nasopharynx to the eustachian tube allows bacteria to reach the middle ear.
Imaging is usually not necessary in uncomplicated acute otitis media,
but plays a crucial role in evaluation of intratemporal or intracranial complications.
Noncontrast CT scan shows opacification of the middle ear cavity and mastoid air cells with possible fluid levels; nonspecific debris is seen in acute uncomplicated otitis and mastoiditis.
The integrity of osseous structures,
including the ossicles,
mastoid cortical bone,
and mastoid trabeculae,
is preserved.
Contrast-enhanced CT and/or MRI are performed when a complication is suspected,
including the whole head in the field-of-view.(Figg.12,13,14,15)
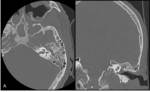
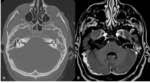
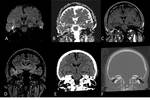
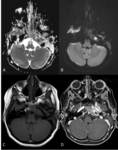
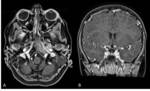
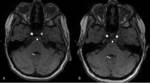
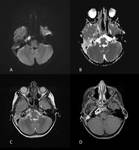
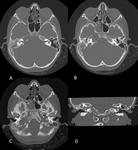
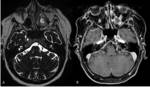
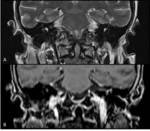
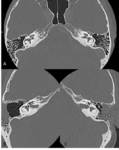
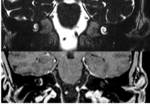
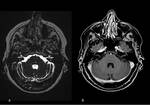
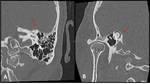
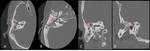
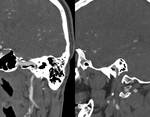
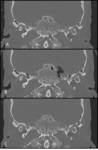
Petrous apicitis is an infectious process that occurs in the setting of a pneumatized petrous apex (present in 30% of the population),
caused by medial extension of acute otitis media.
It is characterized by septal and cortical destruction,
osteitis,
and adjacent meningeal inflammation.
Patients usually present with an acute febrile illness and some or all of the symptoms of the classic Gradenigo triad (ear pain,
palsy of the sixth cranial nerve,
and facial pain).
Possible complications of petrous apicitis include meningitis,
cerebral abscess formation,
and venous sinus thrombosis.
Because the petrous apex cannot be directly visualized,
imaging evaluation is mandatory and often critical for patient care,
as treatment approaches depend on the specific disease process and the nearby structures involved.
(Figg.16,17,18,19,20,21).
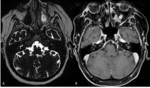
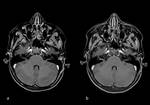
Labyrinthitis refers to inflammatory disease of the perilynphatic spaces of the inner ear that results in secondary changes withic the endolymphatic spaces (membranous labyrinth).
It can occur as a result of infections (viral or bacterial) or may be autoimmune.
The most common symptoms are SNHL and vertigo.
The evolution of labyrinthitis is characterized by three stages: acute,
fibrous,
and ossification.
In the acute stage,
the CT scan is normal,
while contrast- enhancement of the inner ear may be noted on T1-weighted MR images; this enhancement is typically faint.
In the intermediate fibrous stage there is loss of fluid signal intensity on heavily T2-weighted sequence images with persisting gadolinuim enhancement,
while the CT scan may still appear normal.
In the late ossific stage,
the normal cochlea,
vestibule,
and/or semicircular canals are replaced by bone attenuation on CT scans and appear as low-intensity signal on T2w MRI.(Figg.22,23,24,25,26,27,28)
IDIOPATHIC LESIONS
Bell's palsy refers to acute facial nerve paralysis with no identifiable cause. It was long thought to be idiopathic; strong evidence is now present to implicate reactivation of herpes simplex virus or varicella zoster virus (Ramsay Hunt syndrome) with latent infection in the geniculate ganglion.
Contrast-enhanced MRI may demostrates thickening and increased signal of the facial nerve in the fundal portion of the internal auditory canal or uniformly linear enhancing facial nerve.(Figg.29,30)
Perilymphatic fistulas (PLF) is an abnormal communication between the perilymphatic space of the inner ear and the air space of the middle ear,
most commonly occurring at either the round or oval window.
Patients with PLF have sudden hearing loss,
fluctuating sensorineural deficit,
vertigo,
tinnitus and headache.
When a PLF exists,
perilymph in the inner ear escapes,
driven by the hydrostatic pressure of the cerebrospinal fluid (CSF),
and is replaced by CSF.
This can also result in lower than normal levels of CSF fluid around the brain.
A PLF should be considered in pediatric patients with recurrent meningitis,
and the option of middle ear exploration should be pursued.
Imaging evaluation is performed to exclude other causes of associated symptoms.
At CT evaluation inner ear anomalies must be reported.
Demonstration of pneumolabyrinth is the most important sign,
expecially if associated to middle ear effusion; careful attention to the stapes superstructure is required,
in order to look for any anatomical variants.(Fig.31)
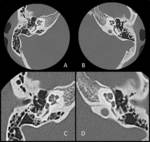
Semicircular Canal Dehiscence (SCD)
Superior semicircular canal dehiscence (SSCD):The SSCD syndrome was first described by Minor et al in 1998 and is characterized by the formation of a “third opening” or “third window” between the superior semicircular canal and the middle cranial fossa,
secondary to a bony defect in the canal,
with disruption of endolymphatic homeostasis particularly with loud auditory stimulations. It is characterized by vertiginous symptoms,
oscillopsia,
and rotatory and vertical nystagmus occurring in the setting of loud noises (Tullio phenomenon).
SSCD can be identified with CT,
demonstrating absence of bone forming the roof of the superior surface of the canal, best seen at high resolution 0.5 mm collimation and MPR in the plane of the superior canal (Pöschl views) and in a perpendicular plane to the same canal (Stenvers views).
The bone defects have been described at the level of the arcuate eminence or in the region of the superior petrosal sinus.
Studies have found that magnetic resonance imaging (MRI) is also very useful for diagnosing SSCD syndrome,
but it is usually not performed in the acute setting.(Figg.32,33)
Posterior semicircular canal dehiscence (PSCD) is rarely reported compared to SSCD,
and has been reported in association with a high jugular bulb or a aberrant arachnoid granulation. PSCD and SSCD may be associated on the same side and this suggests to be due to a congenital maldevelopment of the inner ear.(Figg.34,35)
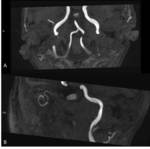
Spontaneous Petrous Carotid Artery Dissection
Spontaneous dissection of cervical vessels is a well-documented cause of ischemic stroke in young adults.
Spontaneous dissection can accour especially in patients with fibromuscolar dysplasia (FMD),
cystic medial necrosis,
intimal fibroelastic abberations or connective tissue disorders,
e.g.
Marfan syndrome.
Dissection is characterized by subintimal (subintimal dissection) or subadvential (subadvential dissection) penetration of circulating blood causing vessel narrowing and leading to thromboembolism,
pseudo aneurysm formation or both.
Non-contrast brain CT is insensitive for dissection but may demonstrate ischaemic changes within the brain.
CT Angiography (CTA) may demonstrate enlargement of the dissected artery and abnormal vessel contour.
Classical appearance is: narrowed eccentric lumen surrounded by a crescent-shaped mural thrombus and thin annular enhancement; intimal flap; dissecting aneurysm (pseudoaneurysm).
MRI shows: high signal crescemt sign within the wall of the vessel (best seen with T1 fat saturation or T2 weighted images),
absent flow-void,
abnormal vessel contour on MR Angiography (MRA) and evidence of cerebral ischaemia.(Figg.36,37)
MISCELLANEOUS
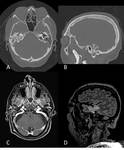
Petrous apex aerated lesion
In Fig.38 is reported the case of a young man who was admitted at the emergency department for left trigeminal palsy and headache,
with suspected cervical artery dissection; no significat trauma was referred.
CTA was negative for acute vascular lesions and brain stroke,
but the left petrous apex showed air bubbles (not present in a 2 years previuos CT examination),
which compress the left Meckel cave.
After 6 months,
next CT scan showed air resorption and resolution of trigeminal palsy.
Iatrogenic lesion
In Fig.39 is reported the case of a 15 years old boy with pneumococcic meningitis after middle cranial fossa hadrontherapy for recurrent/residual sellar lesion (previuosly surgically treated - pituitary macroadenoma).
Imaging demonstrate destruction of cortical bone of the right petrous apex which allowed intracranial bacterial spread from temporal bone and CSF leak into the middle ear,
found at clinical evaluation.
Surgical screws mobilization
In Fig.40 is reported the case of a 58 years old woman with right retroauricolar swelling who received cochlear implant 7 years before.
CT scan demonstrated subgaleal fluid collection of temporal and retroauricolar region on the right side,
with mobilization of surgical screws.
The Patient underwent surgical toilette of the fluid collection and cochlear implant reprise(Fig.41).