The temporal bones comprise the lateral skull base,
forming portions of the middle and posterior fossae.
Each temporal bone is composed of five osseous parts: the squamous,
mastoid,
petrous,
tympanic,
and styloid portions.
Temporal bone represents a crucial site of skull base: within temporal canals and foramina are located vascular and nervous structures (petrous internal carotid artery and 7th and 8th cranial nerves),
middle ear structures (tympanic membrane,
ossicles) and inner ear components (bony and membranous labyrinth,
perilymphatic spaces).
Temporal bone is also contigous to very important structures (i.e dural sinuses,
meninges,
cerebral lobes,
cerebellum): pathologic processes involving temporal bone may spread to these structures resulting in dangerous complications.
Non-traumatic acute temporal bone lesions represent a frequent indication for imaging after clinical evaluation,
especially to exclude intracranial,
potentially fatal,
disease or complications.
The most common clinical symptoms are: otalgia (with or without otorrhea),
sensorineural hearing loss,
facial nerve disorders,
vertigo and dizziness.
Sudden sensorineural hearing loss (SSNHL) is defined as sudden hearing impairment,
of at least 30 dB at three consecutive frequencies occurring over 3 days,
and its incidence has been estimated as 5±20/10,000 individuals per year.
Although the exact etiology of SSNHL is still debated (such that it is classified as idiopathic),
viral infections,
immunological diseases,
and impairment of the vascular microcirculation have been suggested as possible causes.
Because stroke,
malignancies and vestibular schwannoma can give rise to SSNHL,
as obvious potential causes they should be addressed in the initial and follow-up management course in all patients with SSNHL.
Vertigo is defined as a false sense of motion; vertigo may be persistent or episodic,with or without hearing loss.
Vertigo and dizziness can be symptoms of various diseases,
such as: labyrinthitis,
Meniere disease,
benign paroxysmal positional vertigo,
vestibular neuritis,
perilymphatic fistulas,
migraine,
stroke,
intracranial tumors. When imaging is performed the most important aim is to identify possible central cause.
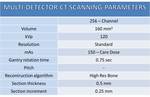
Computed tomography (CT) has revolutionized imaging of the temporal bone; multisection CT scanners allow acquisition of high resolution volumetric data that enable image reformation in any plane (multiplanar reconstruction,
MPR).
CT is an essential imaging test for the initial evaluation of temporal bone,
as a result of its high resolution (HR) for bone assessment and its short acquisition time.
CT is usually performed without contrast media administration; intravenous constrast media may be considered when infectious complications or neoplastic conditions are suspected.
CT is very useful because it quickly allows to extend the scan to the whole head (ie intracranial complications).
In many cases it is possible to reach a diagnosis or,
at least,
to reduce the range of pathological possibilities.
After antero-posterior and lateral topograms,
axial CT images are acquired through the temporal bones,
with scan excursion from the arquate eminence through the mastoid tip.
At our institution,
0.5 mm axial sections are then reprocessed and reformatted into magnified coronal and sagittal images and displayed at 0.25 mm intervals with overlap.(Figg.1,2,3)
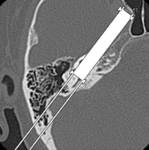
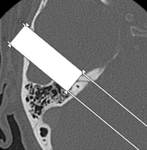
In addition to the traditional axial and coronal views,
it has become routine at our institution to also perform reformation in the Stenvers and Pöschl projections.
The Stenvers projection is the plane parallel to the long axis of the petrous bone,
and the Pöschl projection is the plane perpendicular to the long axis of the petrous bone.(Figg.4,5)
These additional planes are useful for evaluating the structures of the middle and inner ear,
which may not be as well seen in the standard axial and coronal planes.
Magnetic Resonance Imaging (MRI) is a second level modality to evaluate temporal bone.
It is superior to CT in differentiating soft tissue and represents the gold standard to evaluate the fluid-filled spaces of inner ear,
nervous structures (facial and vestibulocochlear nerves),
that pass through cerebellopontine angle (CPA) and the internal auditory canal (IAC),
and the brainstem.
MRI is also useful in differentiating soft tissue (ie cholesteatoma) in middle ear and mastoid,
petrous apex and external auditory canal (EAC).
MRI is performed using at least 1,5 Tesla magnet with iv gadolinium administration,
using sequences and parameters listed in Fig.6.
Axial thin-section heavily T2-weighted imaging sequences and constructive interference in steady state (CISS) MR imaging are obtained through the IAC and pons.
This sequence associates high signal with high spatial resolution,
thus obtaining excellent visualization of nervous structures lying in fluid spaces (liquor,
perilymph and endolymph).
CISS sequence allows MPR on coronal and parasagittal planes (perpendicular to IAC long axis).
Parasagittal images best demonstrate the facial nerve (CN7) and the vestibulo-cochlear nerve (CN8).
Non–echo-planar Diffusion-weighted imaging (DWI) sequences,
on axial and coronal planes, are superior to conventional echo-planar DWI in temporal bone evaluation,
since they minimize susceptibility artifacts at the skull base and increase sensitivity for detection of lesions as small as 2 mm.
DWI technique is indicated when an abscess is clinically suspected and to exclude brain stroke.
CT and MRI are complementary imaging modalities in the evaluation of temporal bone. Radiological approach usually comprises:
- CT for bone structures: external auditory canal,
middle ear,
osseous labyrinth,
osseous canal of cranial nerves
- MRI for soft/fluid structures: fluid flilled spaces of inner ear,
cranial nerves,
cerebellopontine angle,
brainstem and soft tissue in middle ear,
mastoid and petrous apex aerated cells.