Series selection
Our series was collected between March 2015 and July 2016.
We performed 19 procedures (9 men and 10 women) in patients with skeletal metastases (Hip,
femur,
tibia and spine) from breast (12),
lung (4),
colon (2) and prostate (1) cancer.
All procedure was performed with multislice CT-guide with or without fluoroscopy.
Lesion diameter ranged from 2,0 – 9,0 cm.
Patients mean age 68 y; range 53-78 y.
In our series,
all treated lesions were osteolytic.
Patient selection
Patient selection was performed by a multidisciplinary team consisting of an anesthesiologist,
an orthopaedic surgeon and a radiologist.
Indications and contraindications were verified at two levels of selection: a first clinical level and a second radiological level.
The first level of selection,
carried out by the anesthesiologist and orthopaedic surgeon,
identified patients with bone metastases accompanied by pain not sufficiently responsive to medical therapy.
All patients were administered the following assessment scales to verify clinical eligibility for the procedures: 10-point visual analogue scale (VAS) (10 worst ever pain; 1 no pain) for pain assessment and 3-point analgesic use scale (3 complete daily coverage; 2 partial daily coverage; 1 occasional coverage) for analgesic use evaluation.
Data from the above assessments were collected in a questionnaire.
The second level of selection involved imaging studies and was the responsibility of the radiologist.
All patients underwent pre-procedural radiographic assessment and contrast-enhanced CT scans to determine patients’ anatomical compatibility.
Materials
Biopsies were performed with Synthes Bone Access Needles (Moller Medical GmbH,
Wasserkuppenstrabe 29-31,
36043 Fulda,
Germany) with the 8-10 gauge calibre biopsy needle.
All biopsies were done under CT guidance (GE Light Speed H16,
GE Healthcare Medical Systems Italia S.p.a.
,
via Galeno 36,
20126 Milano,
Italy).
Maximum attention was addressed to the patient’s comfort.
The lesion was localized,
and the point of entry on the skin was marked in accordance with the biopsy technique.
Percutaneous microwave ablation was performed using a 2.45 GHz microwave generator (AMICA-GEN,
HS Hospital Service,
Aprilia,
Italy) delivering energy via a 14- or 11-gauge,
minichoked,
water-cooled,
interstitial antenna (AMICA-GEN).
For Cementoplasty we used Synthes Vertecem V+ system (Synthes GmbH,
Elimattstrasse 3,
4436 Oberdorf,
Svizzera) composed of needles with bevel or diamond tip,
12-,
10- and 8-gauge calibre and 12- to 14-cm long,
stop-cock 1-2 ml syringes for the aspiration/injection of acrylic cement.
Methods
To minimise the risk of infection,
patients received antibiotic prophylaxis 1 days before and 2 day after the procedure.
The procedures were performed in local anesthesia under conscious sedation or in general anesthesia,
according with tumore site or with patient condiction to ensure as much comfort as possible and to facilitate needles access to the lesion.
The patient’s vital signs should be continuously monitored.
Procedure start with biopsy.
A radio-opaque skin marker may be placed to help determine the entry point at the patient’s skin.
Following preliminary axial CT scanning,
the most appropriate slice is selected to plan the most ideal route for directing the needle into the lesion.
The selected slice is surface marked on the patient’s skin with a surgical marking pen.
The surgical field was prepared by accurately sterilising the skin and delimiting the needle entry point with large sterile drapes to minimize risks of infection.
After administration of local anaesthesia (1% lignocaine),
a small skin incision is made and the biopsy needle is directed into the lesion under CT guidance.
8 G-11 G cutting needles may be used to obtain material for cytology,
culture,
and histopathological examination.
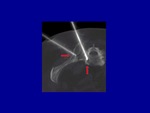
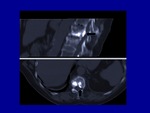
After biopsy,
under CT guidance,
a 14- or 11-gauge antenna is advanced into the target lesions without using a coaxial introducer (fig.
1).
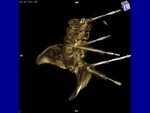
Upon completion of the desired ablation,
we retract the device and the cementoplasty needle is placed into the tumor (fig.
2).
Preparation of the acrylic cement is done after having placed the needle into the lesion to have the optimal viscosity.
To monitoring the cement injection we use radiofluoroscopic guidance that check its distribution and identify possible leakages.
The amount of acrylic cement injected in each lesion ranged from 3 cc to 10 cc.
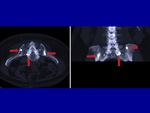
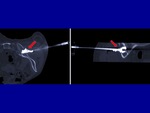
After the procedure we obtained a series of MPR CT scans to evaluate and document distribution of the cement,
possible leaks and soft tissues haematomas (fig.
3- 4- 5).
Patients rest in supine position for about 1-3 h after the procedure.
All patients were discharged from hospital within 24 h
Statistical analysis
Statistical analyses werw performed using IBM SPSS Statistics version 17.0 for Windows (Microsoft,
Redmond,
WA).
Differences between the average VAS score and analgesic-use score at baseline,
24h,
1 week and month 1 post-procedure were evaluated using Student's t test,
for unpaired data.
p<0.05 was considered statistically significant.