Acquired vertebral collapse in children can be caused by a wide range of causes which can be categorized as traumatic,
infective,
neoplastic and miscellaneous.
NORMAL IMAGING APPEARANCE
At birth,
the quantity of red (haematopoietic) marrow is higher.
During skeletal maturation,
hematopoietic marrow is converted into fatty marrow.
On MRI,
red marrow has T1 and T2 signal equal to or higher than muscle,
but less than fat.
Fatty marrow has a higher T1 signal and a lower T2 signal.
In neonates,
hematopoietic marrow usually has T1 signal intensity slightly lower than muscle,
reflecting the larger percentage of cellular marrow.
After the neonate period,
a signal intensity lower than normal muscle is always pathologic.
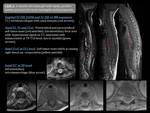
IMAGING ASSESSMENT
First step: AP and lateral standing radiographs of the spine.
It enables to perform an initial evaluation.
Second step: Magnetic Resonance (MR). The standard protocol includes sagittal and axial T1Wspin echo (SE) and T2WFSE sequences.
The fat-suppressed sequence (STIR or fat-suppressed T2W FSE) is relevant to evaluate neoplastic,
infective or inflammatory disorders.
The presence of marrow edema is best assessed with STIR and fat-saturated T2 images.
The administration of intravenous gadolinium is indicated if spinal osteomyelitis/discitis or tumor is suspected.
Third step: Sometimes is essential to evaluate the rest of the skeleton (discontinuous or multifocal affectation).
In these cases,
it is indicated to perform a whole-body bone scintigraphy,
bone series or whole-
body MR.
Fourth step: The use of CT should be minimized (only used if we need additional information).
When indicated,
imaging should be restricted to the smallest FOV necessary.
VERTEBRAL COLLAPSE: DIFFERENTIAL DIAGNOSIS:
Integrity of the vertebral body depends on its outer cortex and trabecular bone/bone marrow.
Destruction of any of these components causes loss of vertebral height,
which can be caused by a wide range of pathological conditions,
including trauma.
Vertebra plana is defined as a vertebral body reduced to a dense sclerotic band (often with preservation of disc spaces).
The question is if there is a congenital or acquired alteration.
In case of deformed bones,
we must think of dysplasia,
bearing in mind that the infrequent manifestations of acquired diseases are more frequent than osseous dysplasia.
We review the typical imaging findings of the more common pathological processes,
highlighting the differential features of each one.
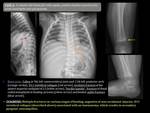
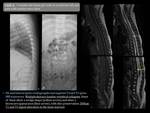
TRAUMATIC CAUSE: Fig. 1
Differential diagnosis between a post-traumatic (accidental or non-accidental) and pathological fracture is difficult,
but of key importance.
Clinical history is an important clue in differentiate both.
Thoracolumbar fractures are more common in older children and adolescents,
while cervical fractures are more common in younger children.
There are some imaging findings in support of a traumatic origin:
- Similar appearance to fractures in adults: Burst or wedge shape fractures.
- Bone marrow edema involving mainly the upper aspect of the vertebral body and with residual fatty marrow.
- No pedicles involvement.
- Posterior and superior retropulsion of the outer cortex.
- Absence of surrounding soft tissue mass.
Sometimes it is difficult to differentiate non-accidental injuries from osteogenesis imperfecta,
especially in young children who suffer multiple,
repeated and unexplaied fractures (with or without antecedent of a minor trauma).
Therefore osteogenesis imperfecta is a paramount differential diagnosis in this clinical setting.
Osteogenesis imperfecta (OI) is a heterogeneous group of genetic disorders.
There is a qualitative and /or quantitative abnormality of type I collagen,
which conditions an increase in bone fragility,
a low bone mass density and extraskeletal manifestations involving connective tissues and bones.
OI is categorized in 7 types.
In practice,
cases diagnosed before or at birth are usually severe forms.
By comparison,
cases diagnosed after birth tend to be less severe forms.
These milder forms are much more difficult to diagnose and may be sometimes confused with non-accidental injury.
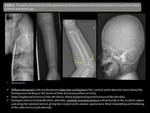
Radiographic findings (OI):
Osteopenia: Radiographs reveal cortical bone thinning and an increase in transparency of trabecular bone.
Bone fractures: It is manifested by multiple,
repeated and unexplaied fractures (with or without antecedent of a minor trauma).
Fractures usually involves the long bone diaphyses,
the spine and the apophyses.
Apophyseal avulsion fractures are less common
Typical spinal findings are: Multiple compression thoraco-lumbar fractures,
L5 spondylolysis with or without spondylolisthesis,
and elongation of the pars interarticularis of L5.
Other skeletal manifestations depend on the severity of the disease and may include short stature and progressive deformities of the spine (kyphosis,
scoliosis),
the rib cage or the lower limbs.
INFECTIVE CAUSES:
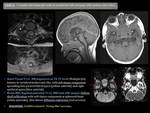
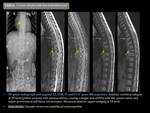
Pyogenic osteomyelitis Fig. 1 Fig. 2
Pyogenic osteomyelitis is a bacterial infection of vertebrae and intervertebral disc.
In children,
the bacterial inoculation is through the persisting vascular channels in the disc space and pyogenic discitis may occur after bacteraemia.
The most common location is the lumbar spine,
followed by thoracic and cervical spine.
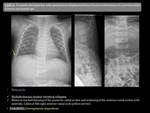
Radiographic findings:
Radiographs could be negative up to 2-8 weeks after the onset of symptoms.
It is frequently located at the anterior column of the vertebral body and is characterized by loss in vertebral body height,
endplate bone erosions and paraspinal soft tissue mass.
MR findings:
- Ill defined hypointense (T1) and hyperintense (T2FSE or STIR) vertebral marrow signal with avid enhancement after gadolinium administration.
- Loss of endplate definition and vertebral collapse.
- Disc space narrowing with post-gadolinium enhancement,
and erosions in adjacent endplates.
- Paraspinal and/or epidural soft tissue swelling or abscess: isointense to muscle on T1 and hyperintense on T2 with post-gadolinium enhancement.
Tuberculous osteomyelitis
It refers to a tuberculous infection of the spine and adjacent soft tissues.
The most common location is the mid-thoracic or thoraco-lumbar spine.
The spread of infection is subligamentous beneath the anterior longitudinal ligament,
leading to irregularity of the anterior vertebral endplate (early sign),
which can give rise to anterior vertebral collapse with anterior wedging,
and secondary kyphosis.
The infection usually spares the posterior elements and often involves multiple levels.
Generally,
there is an affectation of two or more contiguous vertebrae.
But sometimes there are multiple inconsecutive levels affected.
In this case,
a whole-body MR is indicated.
Radiographic findings:
- Endplate irregularity (most common anterior) and osteolysis leading to loss in vertebral body height).
Vertebra plana.
- Diffuse vertebral sclerosis.
- Fusion across disc space in late stages.
MR findings:
- T1 hypointense and T2/ STIR hyperintense bone marrow signal.
- Relative discal preservation at the beginning.
In advanced stages,
a loss of disc height can occur that shows hyperintense T2/STIR signal.
- Large dissecting paraspinal/subligamentous and psoas abscesses with peripheral enhancement (Differential diagnosis with pyogenic osteomyelitis that usually demonstrates diffuse enhancement).
There are some features more suggestive of tuberculous spondylitis:
- Well defined paraspinal involvement.
- Abscess with peripheral/ring and thin enhancement.
- Subligamentous extension affecting three or more vertebral levels.
NEOPLASTIC CAUSES:
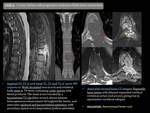
Ewing sarcoma Fig. 5 Fig. 6
Ewing sarcoma is the second most common malignant primary spinal tumour in children.
Typically arises unilaterally in the neural arch with secondary involvement of the vertebral body (It rarely originates in the vertebral body).
Generally on debut,
it manifests as a large extraosseous mass,
with extension into the spinal canal in a 90% of cases,
causing secondary neurological symptoms.
Ewing sarcoma most commonly affects the spine as metastatic disease from a primary tumor elsewhere in the body but can also present as a primary osseous lesion that is centered in the vertebral body,
in the posterior elements,
or in the sacrum.
Radiographic/CT findings:
- Expansile predominantly lytic lesion (a minority of cases show a mixed appearance) of vertebral body or sacrum.
- Permeative/moth eaten pattern.
- Cortical thickening and destruction.
Tiny perforations of cortex rather than extensive loss of cortical bone.
- 50 % of cases have extraosseous noncalcified soft-tissue mass.
MR findings:
T1 hypointense signal compared to normal bone marrow.
On T2 images it varies from intermediate to hyperintense.
It presents moderate enhancement after administration of gadolinium with internal areas of necrosis
Aneurysmal bone cyst Fig. 7
Aneurysmal bone cyst (ABC) is an expansile,
benign neoplasm containing thin-walled,
blood-filled cavities.
Although often ABC has a primary origin (up to a third of cases).
It can be also secondary to an underlying lesion (osteoblastoma,
giant cell tumor,
chondroblastoma or fibrous dysplasia).
ABC arises in neural arch,
affecting the posterior elements unilaterally and often extending to the vertebral body,
where they produce partial collapse or vertebra plana.
Radiographic/CT findings:
- Ballon-like expansile remodeling of bone (centered in neural arch and extending into vertebral body)
- Cortical thinning with an “eggshell appearance”
- Asymmetric vertebral collapse.
- Typical sign: Absence of the ipsilateral pedicle.
- The degree of collapse determines the severity of structural scoliosis.
MR findings:
- Multi-loculated neural arch +/- vertebral body mass with heterogeneous signal on T1 and T2 images.
It contains cystic spaces of varying sizes with fluid-fluid levels due to blood products).
ABC may be surrounded by a hypointense T2 rim.
- It can associate epidural extension,
with secondary spinal cord compression
Fibrous dysplasia
Fibrous dysplasia (FD) is a developmental defect of osteoblastic differentiation and bone maturation of unknown origin.
It may affect the skeleton either in isolation or in variable combination with endocrine and cutaneous abnormalities.
It mainly affects the thoraco-lumbar region.
Fibrous dysplasia of the spine may be monostotic or polyostotic.
The polyostotic form is typically associated with spinal deformity,
and will also affect other parts of the skeleton.
In particular,
involvement of the adjacent rib is a highly suggestive feature.
The monostotic form is extremely rare and not commonly associated with collapse.
Radiographic findings: Ground glass appearance in both the body and posterior elements.
CT findings: Optimal technique.
A focal lesion may have a thick sclerotic margin.
MR findings: Hypointense signal in T1 and T2 images due to fibrous component +/- cystic areas in relation with cystic degeneration.
Osteosarcoma
Osteosarcoma is a malignant bone tumor which may be primary or secondary (post-radiotherapy) in origin.
It is an aggressive lesion forming immature bone.
Typically it arises in posterior elements,
with secondary extension into the posterior vertebral body giving rise to vertebral collapse.
Radiographic/CT findings:
- Permeative/Moth-eaten appearance,
cortical breakthrough and soft tissue mass.
- 80% of osteosarcomas have a mineralized matrix secondary to the deposit of osteoid.
This may be extensive,
producing an “ivory vertebra” appearance.
- 20 % of cases are purely lytic.
MR findings:
- Mineralized tumors demonstrate T1 and T2 low signal intensity.
- Non-mineralized tumors and soft tissue mass demonstrate T1 low-intermediate signal and high T2 signal.
- Frequent extension into the spinal canal.
Acute lymphoblastic leukaemia/lymphoma
It is a rare cause of vertebral collapse.
Acute lymphoblastic leukaemia (ALL) is the most frequent malignant disease in the pediatric age.
Spinal leukemia may involve either single or multiple vertebral bodies,
but the most common presentation is multiple compression fractures.
Radiographic/CT findings: Diffuse vertebral osteopenia with multiple vertebral fractures +/- lytic spinal lesions.
MR findings:
- Osteopenia can result in vertebral collapse in the absence of malignant marrow infiltration (Normal appearance on MRI).
- Bone marrow infiltration manifests as a diffuse alteration of signal intensity,
with a low T1 signal and increased T2W/STIR signal.
After treatment,
there is a restoration of the normal height of the vertebral body.
Lymphoma:
It can produce lytic or sclerotic lesions,
with involvement of the whole vertebra.
Metastases
Metastatic disease is less common in the paediatric population than in adults and has a different range of primary lesions.
The most common causes are: Ewing sarcoma,
neuroblastoma,
osteosarcoma,
rhabdomyosarcoma,
Hodgkin's disease,
soft tissue sarcoma and germ cell tumour.
Metastases are typically of low signal on T1W sequences replacing normal marrow and can be variable on T2 and STIR sequences.
Whole-body MRI has been shown to have greater sensitivity than conventional imaging for bony metastases
MISCELANEOUS CAUSES
Langerhans cell histiocytosis
The skeleton is the most commonly involved system in Langerhans cell histiocytosis (LCH) and is the most common location for a single-lesion ,
what is called eosinophilic granuloma (EG).
The most common location is the cervical spine.
It can involve a single vertebral body,
but sometimes affects at multiple levels,
producing anterior vertebral wedging and vertebra plana.
The posterior elements and disc spaces are usually spared.
Radiographic/CT findings: Poorly defined lytic lesions.
MR findings:
- Decrease in bone marrow signal on T1,
increase in T2 and STIR (signal intensity is lower if lesions are healing) and avid enhancement with gadolinium representing the hypervascular healing process.
- Adjacent soft tissue involvement may be present.
CT-guided biopsy is frequently used to aid diagnosis. Therefore,
in the setting of multilevel disease,
MRI can aid in deciding which vertebra to biopsy based on the presence of marrow edema at an active level.
Idiopathic osteoporosis
Idiopathic osteoporosis is an infrequent metabolic bone disorder of children and adolescents,
of unknown etiopathogenesis.
It is characterized by bone demineralisation.
The four main characteristics of the idiopathic osteoporosis are:
1) The beginning is usually before puberty.
2) Fractures of the vertebral bodies and metaphysis of the long bones.
3) Neo-formation of osteoporotic bone.
4) Gradual remission after puberty.
Imaging features:
- Generalized osteopenia with less frequent involvement of the skull.
- Spinal osteopenia causes vertebral collapse at multiple levels (thoracic and lumbar),
with a biconcave or wedge-shape appearance.
- The involvement of long bones is characterized by metaphyseal involvement.
Prevention of further vertebral fractures is the key to management,
as the condition is typically self-limited (usually recovery in 2-4 years).
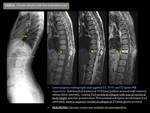
Chronic recurrent multifocal osteomyelitis Fig. 8 Fig. 9
Chronic recurrent multifocal osteomyelitis (CRMO) is a condition of unknown origin,
characterized by areas of sterile (non-bacterial) osteomyelitis.
The most frequent location of pathological fracture is the dorsal column,
arising in the vertebral bodies with or without extension to the posterior elements.
There is usually a multi-level involvement with a tendency to affect non-continuous vertebrae.
A feature that differentiates from bacterial osteomyelitis.
Vertebral collapse may lead to vertebra plana,
but unlike LCH,
this does not recover following treatment.
The absence of extra-osseous extension also aids in differentiation from LCH.
Radiographic/CT findings:
- Predominance of mixed lesions (lytic-sclerotic).
- Lytic vertebral lesions with sclerotic margins.
- Completely sclerotic lesion (possibly indicating an advanced stage of the disease).
- Irregular vertebral endplates.
- Secondary vertebral collapse
MR findings:
- Subchondral fracture parallel to the vertebral endplate with alteration of the bone marrow signal (decreased on T1 and increased on T2 in the acute phase).
- Affectation of perivertebral soft tissues is very uncommon.
- Highly suggestive feature: Vertebral collapse of new onset in the context multiple previous vertebral collapses.
Whole-body MRI is useful to identify further foci of disease,
follow-up and response to treatment evaluation.