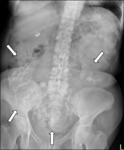
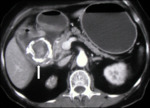
Findings and differential diagnosis?

Fig. 1
References: Courtesy of Elena Klusch, MD. Department of Radiology, Hospital Privado Universitario de Cordoba. Cordoba, Argentina.
ENCRUSTATED PYELONEPHRITIS
Chronic inflammatory process caused by crystal deposits from urea-producing organisms.
Corynebacterium urealyticum is the most common associated organism.
Risk factors:
- Transplanted/ immunocompromised patients.
- Urological surgery/ damaged urothelial mucosa.
- Previous antibiotic therapy.
Imaging findings:
Most affected anatomic regions: the trigone,
ureters,
and bladder neck.
Abdominal plain film
- Calcification in the wall of the collecting system,
ureter or bladder.
- Staghorn calculus association.
CT
- Non-contrast CT is the most sensitive diagnostic tool for urothelial calcifications (Fig. 2).
Ultrasound
- Thickened and calcified urothelium (kidney,
ureter or bladder).
Differential diagnosis:
- Staghorn calculi
- Renal Tuberculosis
- Schistosomiasis (bladder wall calcification)
- Calcified renal cell carcinoma
- Amyloidosis
Treatment: Antibiotics and urine acidification.
Complications: Chronic kidney disease and renal transplant graft lost [3,4].
SCLEROSING PERITONITIS S/P (Cocoon Syndrome)
Acquired chronic inflammatory condition of the peritoneum.
Categorized based on etiology into primary (idiopathic) and secondary (peritonitis,
peritoneal dialysis,
abdominal surgery,
tuberculosis and sarcoidosis).
Peritoneal dialysis is the most common etiology of secondary SP (prevalence among these patients of 1.4–7.3%).
However,
meconium peritonitis is the most common cause of peritoneal calcification.
Imaging findings:
Abdominal plain film
- Air-fluid levels and dilated small intestine from obstruction.
- Cauliflower sign or accordion pattern of conglomerated intestinal loops (Fig. 3).
CT
- Peritoneal and mesenteric thickening with mural or peritoneal calcification (Fig. 4).
- Nodal calcification is more related with a malignant origin.
- Sheet-like calcification is more commonly associated with a benign etiology.
- Conglomerated small intestine encased by dense capsule.
Ultrasound
- Dilated intestinal loops encased by a dense fibrous membrane and thickened peritoneum.
Differential diagnosis:
- Primary peritoneal malignancy (primary papillary serous peritoneal carcinoma)
- Secondary peritoneal malignancy (ovarian,
gastric,
colon,
squamous lung cancer,
melanoma,
renal cell carcinoma)
- Peritoneal tuberculosis
- Previous meconium peritonitis (microscopic and macroscopic deposits)
- Peritoneal amyloidosis (omental and peritoneal thickening with nodular calcification)
- Peritoneal mesothelioma (diffuse or nodular calcification)
- Pneumocystis carinii infection (small nodular calcifications)
- Post-surgical heterotopic ossification
Treatment: surgical resection.
Complications: Intestinal obstruction,
entero-cutaneous fistula,
small intestinal necrosis,
and malnutrition [2,5].
BOUVERET SYNDROME
Gastric outlet obstruction secondary to an impacted gallstone in the distal stomach or proximal duodenum.
The gallstone gain access to the gastrointestinal tract through a biliary-gastric or biliary-duodenal (most common) fistula.
Gallstone ileus is very rare,
however its mortality rate ranges between 12-27%.
Bouveret Syndrome is a very rare form of gallstone ileus,
accounting for only 1-3%.
Imaging findings:
Abdominal plain film
- Rigler’s Triad (pneumobilia,
ectopic gallstone and dilated small bowel loops) seen in 10-50% of the cases (Fig. 5).
- Two air-fluid levels in the right upper quadrant (duodenal bulb and gallbladder).
- Stomach dilation.
- Demonstrates migration of prior documented gallstones.
CT
- Oral contrast increases CT sensitivity.
Contrast can be seen within the gallbladder or surrounding the gallstone
- Localization of the stone and fistula (Fig. 6).
About 25-30% of gallstones are not visualized due to isoattenuation to fluid and bile.
Ultrasound
- Pneumobilia and stomach dilation.
MRI
- Distinction between iso-attenuated stone and fluid and better fistula localization.
Differential diagnosis: Other causes of GI obstruction should be rule out (GI neoplasm).
Treatment: Percutaneous,
endoscopic or surgical removal of the impacted gallstone (relieve obstruction) (Fig. 7).
Subsequent cholecystectomy is not always indicated.
Complications: Necrosis,
perforation,
bleeding,
acute pancreatitis,
gallbladder cancer,
and recurrent cholecystitis.
In 16% of the cases there is another gallstone in the GI tract [6,7].
HYDATYD CYST
Parasitic zoonosis infection caused by larvae of tapeworm particularly in South America,
Africa and Asia.
Mainly caused by E.
granulosus (most common) and E.
multilocurais.
Human is the intermediate host and get infected by ingestion of contaminated water or food or through contact with the definitive host (dog).
- Affect any organ: brain,
lungs,
heart,
liver,
spleen,
kidneys,
peritoneum and muscles.
In 90% of the cases affects the liver and lungs.
- Usually is asymptomatic (symptoms will depend on cyst’s size and localization).
Imaging findings:
At later stages,
calcium deposition increases,
which suggest decreased cyst viability,
therefore a completely calcified cyst is assumed to be death.
Abdominal plain film
- Calcifications in 20-30% of cases.
Curvilinear or ring-like peri-cyst calcification pattern (Fig. 8).
CT
- Evaluation of extra-hepatic hydatid disease,
disease extension and complications.
- Cyst wall and internal septa calcification.
High attenuation of cyst wall is characteristic of HD (even without been calcified).
- Daughter cysts are rounded peripheral vesicles with lower attenuation than maternal cysts.
- Double-contour thick wall appearance is better delineated with contrast-CT (Fig. 9).
Ultrasound
- Multi-loculated cystic appearance and curvilinear internal septa.
- Cyst wall with double echogenic lines separated by a hypo-echogenic layer (Fig. 10).
- Multiple floating internal echogenic foci (hydatid sand).
Snowstorm sign.
Calcified cyst wall or internal matrix.
MRI
- Internal cysts content and cyst wall defects.
- Low T2 signal-intensity rim (Rim sign correlates with the parasitic membranes and pericyst).
- Daughter cysts attached to the germinal layer are hypo-intense in T1 and hyper-intense in T2-weighted images relative to the intracystic fluid.
- Collapsed parasitic membranes (internal twisted linear structures).
Differential diagnosis: based on disease localization.
Treatment:
- Cyst <5 cm and uniclocular: Albendazole.
- Cyst >5 cm: Albendazole + surgical/percutaneous drainage.
- Spillage of contents may be avoided (can lead to anaphylactic shock and increases the risk of recurrence).
Complications: Cyst rupture and/or infection,
anaphylactic shock (most serious),
biliary invasion,
exophytic growth,
seeding and hematogenous dissemination [8,9].
Infant with a calcified lesion in right upper quadrant.
Differential diagnosis?

Fig. 11
References: Courtesy of Carlos Gimenez, MD. Ochsner Medical Center, Louisiana, USA.
FETUS IN FETU (FIF)
FIF is the result of an abnormal embryogenesis characterized by the presence of a monochorionic,
monozygotic fetus localized inside the body of its normally developed twin.
- Usually is a single FIF.
- Very uncommon (1/500,000 live births)
- Male predominance.
- Diagnosed before 18 months of age.
- Clinical presentation due to mass effect.
- Retroperitoneum is the most common site of presentation.
- Other anatomic regions: spine,
extremities,
central nervous system,
gastrointestinal tract,
vascular structures,
genitourinary tract and scrotum.
Imaging findings:
Abdominal plain film
- Visualization of vertebral column and bony structures.
CT
- Fat and calcified content visualized as a central bony structure surrounded by a lipomatous mass (Fig. 12).
Ultrasound
- Cystic retroperitoneal or abdominal lesion.
Differential diagnosis:
- Well-differentiated teratoma (absence of vertebral bodies and limbs)
- Meconium peritonitis
- Mesenchymal hamartoma
- Neuroblastoma
- Adrenal hemorrhage
- Viral infection
Treatment: surgical resection.
Complications: hemorrhage and malignant transformation [10,11].
What do you think about this calcification in this 31 year old woman? Nephrolithiasis?

Fig. 13
CALCIFIED OVARIAN TERATOMA
Germ cell tumor,
classified in mature,
immature and specialized teratoma.
A teratoma is as a neoplasm with little malignancy potential composed of multiple tissues foreign to the anatomic part in which they arise. Mature teratoma is the most common benign neoplasm in young women.
Imaging findings:
Abdominal plain film
- Scattered calcifications or mural calcified nodules (Fig. 14).
CT
- Calcification and fat attenuation within an ovarian cyst is pathognomonic of mature ovarian teratoma (Fig. 15).
Ultrasound
- Echogenic cystic mass with some attenuation due to fat,
hair,
or calcified contents within the mass.
MRI
- Sebaceous components have high signal intensity on T1-weighted imaging.
Complications: Teratoma rupture,
torsion,
and malignant transformation [11,12].
Treatment: surgical resection.
CALCIFIED ADRENAL CARCINOMA
Uncommon endocrine neoplasm accounting to 0.2% of all cancer deaths in the United States.
Most commonly metastasizes to lungs,
lymph nodes,
liver and bones.
Calcification in adrenal carcinoma is very rare and it is secondary to necrosis of the tumor.
Calcification seen in an adrenal mass,
not always mean a malignant process,
however,
carcinoma must be rule out.
Adrenal cyst is the most common calcified adrenal mass in adults.
Imaging findings:
Abdominal plain film
- Coarse calcifications in the territory of the adrenal gland (Fig. 16).
CT
- Large heterogeneous soft-tissue mass.
- Heterogeneous enhancement due to hemorrhage,
necrosis and calcifications.
High-density centrally located coarse or microcalcification.
(Fig. 17).
MRI
- Hypointense adrenal mass on T1-weighted images and hyperintense on T2.
- Internal hemorrhage is high-signal intensity on T2-weighted images.
Differential diagnosis:
- Previous tuberculosis,
hemorrhages or parasitic disease
- Calcified adrenal cyst (peripheral calcification)
- Neuroblastoma (most common calcified adrenal mass in children)
- Pheochromocytoma
- Myelolipoma [13]
Treatment: surgical resection.
JUVENILE RENAL CELL CARCINOMA
Renal cell carcinoma (RCC) is the most common cancer of the kidney.
It has a male predominance and is extremely rare in population younger than 50 years old. Calcification of renal lesions is a common finding,
however,
only 30% of RCC present some calcification.
Imaging findings:
- On abdominal plain film and CT imaging,
calcifications are dense,
small punctuate or linear opacities (Fig. 18).
Diffuse calcified RCC is very unusual.
- On CT,
calcified RCC are hypovascular masses with necrotic foci and calcifications in the interstitium.
There is heterogeneous enhancement on contrast-CT (Fig. 19).
- On MRI T1-weighted imaging are seen as heterogeneous,
masses due necrosis,
hemorrhage and solid components.
Calcifications are difficult to identify by MRI.
Differential diagnosis: Complex renal cyst,
renal abscess,
adrenal tumors.
Treatment: surgical resection [14].
CALCIFIED DIFFUSE CARCINOMATOSIS FROM ADENOCARCINOMA OF COLON
Peritoneal carcinomatosis is the dissemination of any malignancy into the peritoneal cavity.
Most frequently arising from colorectal,
gastric and ovarian tumors. The peritoneum is the second most common affected site after the liver from colorectal cancer recurrence.
Peritoneal carcinomatosis is considered a preterminal stage due to its poor prognosis.
Imaging findings:
Abdominal plain film
- Peritoneal metastases are not usually visualized on plain films,
however they can be seen as coarse scattered calcifications in the peritoneal wall (Fig. 20).
CT
- Nodular invasion of the greater omentum.
“Omental caking” (Fig. 21).
- Malignant ascites is seen on CT.
- Calcification of invasive nodules.
Ultrasound
- Anechoic free fluid from malignant ascites (present in 70% of the cases).
- Echogenic nodules infiltrating the omentum.
Differential diagnosis:
- Peritoneal tuberculosis (necrotic and calcified lymph nodes)
- Mesothelioma (asbestos exposure)
- Pseudomyxoma peritonei
- Sclerosing peritonitis [2,15]
RECURRENT CHONDROSARCOMA INVADING THE INFERIOR VENA CAVA
Malignant tumor arising from cartilaginous tissue.
They are categorized as central or peripheral depending if they arise from the medulla or from the surface,
respectively.
- More common in older males.
- Account for 25% of all primary bone cancers.
- More commonly affects long bones,
followed by the pelvis,
ribs and spine.
Most chondrosarcomas are low-grade tumors with low risk of metastatic disease.
However,
they have a high rate of local recurrence.
Metastases or invasion to the IVC from chondrosarcomas is extremely rare.
Imaging findings:
Abdominal plain film
- Lytic lesions (50% of the cases).
- Ring-like or popcorn calcifications within the lesion (Fig. 22).
CT
- Soft-tissue mass with coarse scattered foci of calcification within the cartilage cap (Fig. 23).
- Most cases present matrix calcification.
- Heterogeneous enhancement on contrast-CT.
Ultrasound
- Evaluate IVC tumor thrombosis.
(also with contrast-CT and MRI).
MRI
- Low-intensity signal on T1-weighted imaging.
- High-intensity signal of non-calcified areas on T2-weighted imaging [16].
Treatment: chemotherapy and surgical resection.
CALCIFIED SPLEEN LYMPHANGIOMA
Very rare benign lymphatic malformation,
resulting in the dilation of thin-walled lymphatic vessels.
Can be localized to the spleen or affect multiple organs,
which is called systemic lymphangiomatosis.
- More common in pediatric population.
- Symptomatology depends on the size of the lesion and is related to compression of adjacent structures (left upper quadrant pain,
nausea,
vomiting,
abdominal distention and a palpable mass).
- Splenic lymphangioma can be associated with cystic hygroma of the neck.
Imaging findings:
Abdominal plain film
- Round masses with curvilinear peripheral wall calcifications (Fig. 24).
CT
- Low-attenuation thin-walled sub-capsular cystic lesions.
- Curvilinear peripheral mural calcifications.
- No arterial enhancement on CT.
Ultrasound
- Hypoechoic or anechoic cystic lesions with or without septations and/or internal debris.
Echogenic calcifications.
- On Doppler Color the vasculature along the cyst walls can be perceptible.
MRI
- On T1-weighted imaging,
cystic lesions are hypo-intense or hyper-intense if they contain hemorrhagic or proteinaceous material.
- On T2-weighted imaging the dilated lymphatic vessels are hyper-intense.
- Useful to distinguish solid content within the cyst to rule out malignant transformation.
Differential diagnosis: Hemangioma,
splenic epidermoid cyst,
mesothelial cyst and hydatid cyst.
Treatment:
- Small uncomplicated cyst: No treatment.
- Large symptomatic: complete or partial splenectomy.
Complications: recurrence,
rupture,
infection,
bleeding,
consumptive coagulopathy,
hypersplenism and portal hypertension [19].
Calcified lesion in right lower quadrant in this 58 year old man.
Differential diagnosis?

Fig. 25: Plain abdominal film shows a large round calcification in the right lower quadrant (circle).
DEDIFFERENTIATED LIPOSARCOMA with OSTEOSARCOMA DIFERENTIATION
Dedifferentiated liposarcoma (DDLS) is a combination of well-differentiated liposarcoma (WDL) and non-lipomatous malignant tumors.
Osteosarcomatous differentiation is extremely rare (less than 5% of DDL cases).
- Most common sites: retroperitoneum,
inguinal region and extremities.
- Calcifications are seen in 30% of cases and suggest tumor dedifferentiation.
- High risk of metastatic disease (17%).
Local recurrence rate is 41%,
within the first 2-years after surgical resection.
Imaging findings:
- Large septated lipomatous tumor with focal nodular non-lipomatous component greater than 1 cm and with coarse calcified components (Fig. 26).
- CT is preferred over MRI for tumor ossification identification,
which can be focal or extensive.
- MRI is better to identify the fatty component from the dedifferentiated element.
- On MRI,
the non-adipose regions are low to intermediate T1 and high T2 signal intensity.
Prognosis and treatment: Most important prognostic factor is anatomic location and the treatment of choice is surgical resection.
GASTROINTESTINAL STROMAL TUMOR
Most common primary mesenchymal tumor of the gastrointestinal tract and in most cases has a benign progression.
Calcification is a rare phenomenon of GIST tumors,
which can be secondary to tissue necrosis or degeneration.
- Expression of KIT (CD117).
- Male predominance and is seen usually in middle to older age.
- Most commonly arise in the stomach followed by small intestine and esophagus.
- High rate of recurrence and metastases (more common in the liver).
Imaging findings:
Abdominal plain film
- Spherical coarse calcified lesion (Fig. 27).
CT
- Large exophytic well-defined mass with a heterogeneous enhancing rim surrounding a necrotic center (Fig. 28).
- Calcified components may be seen as punctate calcification.
Heavily calcified are less common.
MRI
- On T1-weighted imaging the solid component demonstrates low-intensity signal,
also,
a peripheral enhancement due the necrotic center may be seen.
- On T2 the solid component is high signal intensity.
Differential diagnosis: Leiomyoma,
leiomyosarcoma,
lymphoma,
and carcinoid.
Treatment: surgical resection [20] (Fig. 29)