Keywords:
Neuroradiology brain, CNS, CT, MR, Education, Education and training
Authors:
T. V. P. Morais, C. Pinheiro, C. T. F. Perry da Câmara, M. C. Diogo, C. Conceição; Lisbon/PT
DOI:
10.1594/ecr2018/C-2466
Results
An educational review of pitfalls often encountered in the reading of neuroradiological examinations is presented.
Cases include anatomical variants mistaken for pathological findings,
misinterpretation of abnormal findings and other miscellaneous pitfalls.
In the first category,
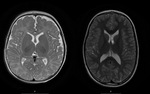
we show the brain MRI of neonatal vs.
a child with age above 2 years old.
In the neonatal brain,
unmyelinated white matter has a low signal intensity on T1 weighted images and high intensity on T2 weighted images.
As myelination proceeds,
the water content of white matter decreases,
causing a reduction in signal intensity on T2 weighted imaging.
There is a corresponding increase in glycolipids,
cholesterol and proteins,
which causes an increase in signal intensity on T1 (Fig 1).
Also in the first category,
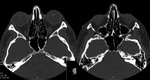
we show the difference between a osseous suture and a fracture.
In the bone evaluation,
the knowledge of the appearance of normal sutures is essential to avoid misinterpretation.
The sutures are found in typical anatomical locations and are characteristically jagged in appearance.
Sutures have corticated edges whereas the edge of fractured skull bones are not corticated.
(Fig 2)
The misinterpretation of abnormal findings included pseudosubarachnoid hemorrhage,
subacute hematoma for tumor and the presence of intracranial fat.
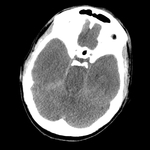
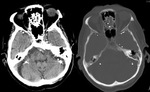
Pseudosubarachnoid hemorrhage is a sign related to apparent increased attenuation within the basal cisterns which simulates a true subarachnoid hemorrhage.
The most common cause is cerebral edema where there is a decrease in parenchymal attenuation and engorgement and dilatation of the superficial venous structures due to an increased intracranial pressure.
The pseudosubarachnoid hemorrhage is usually seen in CT as a symmetrical density confined to the basal cisterns (i.e.
no sulcal density) with a density of 30-40 HU (compared with true acute subarachnoid hemorrhage ~ 60HU).
The clinical context is also essential to help to differentiate between pseudosubarachnoid hemorrhage and true acute subarachnoid hemorrhage.
(Fig 3)
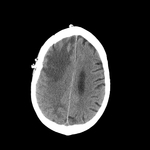
In order to differentiate a tumor from a sub-acute hematoma,
the clinical history and review of previous examinations is essential,
especially in the presence of a hypodensity with surrounding edema in CT.
Also the MRI can help in this differential diagnosis.
(Fig 4)
In the last category,
we included images showing the presence of lipiodol contrast in the basal cisterns.
Lipiodol is an oil-based radio-opaque contrast agent used in the late years that appears as a hyperdensity in CT scans and should not be mistaken with pathologic findings.
(Fig 5)
Normal 0 21 false false false PT X-NONE X-NONE