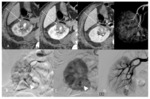
RVI and their imaging features
RVI after NSS include a variety of lesions that are generally isolated but which,
in some cases,
can be associated,
resulting in complex vascular lesions.
· Active arterial bleeding is the consequence of a direct vascular injury determining blood extravasation in the peri-renal space.
US usually shows an echoic collection close to the kidney but the direct demonstration of the vascular lesion is rare.
CT shows an area of contrast medium extravasation with irregular and variable morphology that is evident in the arterial phase and shows spread and expansion in the surrounding tissue on the delayed scan phases; a peri-renal hematoma is a typical finding and may be evident within or outside the Gerota fascia.
Direct bleeding may resolve spontaneously as suggested by the “incidental” asymptomatic and stable perirenal haematomas detected at follow-up investigations after NSS.
Nevertheless,
prolonged high output bleeding can lead to adverse consequences,
including vascular shock,
acute renal failure and death.
In these subgroup of patients,
treatment is mandatory and clinical status is conclusive on the indication to treatment: patients hemodynamically unstable will be treated surgically,
those that are hemodynamically stable will receive endovascular treatment.
(Fig.1)
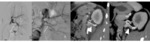
· Pseudoaneurysm is a focal rounded and well defined lesion,
within the renal parenchyma or in the surgical shear; US offers good sensitivity but poor specificity showing a hypoechoic lesion with the possible evidence of doppler signals inside.
CT is more accurate showing intense enhancement of the lesion,
that decreases (wash-out) similarly to that of the arterial blood pool; there is no incremental enhancement on delayed scan phases.
Pseudoaneurysms are defined as unstable lesions with a high risk of rupture,
especially if they show larger diameter > 2 cm or are symptomatic,
therefore require rapid intervention.
(Fig.2)
· Arteriovenous fistulas are anomalous connections between the arterial and the venous systems without an intervening capillary network.
At color doppler US renal AVF appears as a mosaic pattern with a speckling of perivascular soft tissue caused by tissue vibration,
reacting to a rapid flow rate.
At CT imaging,
AVF appears as a tortuous and markedly dilated venous branches,
with an early arterial enhancement in the post-contrast CT images.
The majority of AVFs are asymptomatic and frequently resolve spontaneously within 24 months after diagnosis.
AVFs are thus usually treated conservatively unless they are symptomatic or show persistent gross haematuria,
haemodynamic instability or deterioration of renal function.
Nevertheless,
some investigators advocate aggressive early treatment,
as AVFs can potentially enlarge over time and become high-flow lesions with potential consequences on cardiac function. (Fig.3)
Renal Artery Embolization technique
The majority of RAE procedures are performed through a common femoral approach,
using 4–6F sized arterial sheaths.
Catheterization of the renal arteries is performed using standard Cobra or Shepherd hookshaped 4–5F sized catheters.
These catheters are sufficient to perform selective embolization in the majority of cases.
Micro-catheters allow super-selective angiography and embolization and have been shown to reduce the morbidity and size of induced renal infarction; for these reasons,
if RVI are distal an attempt of super-selective catheterization is suggested.
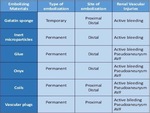
Types of embolization materials
The use of an appropriate technique and a safe and effective embolizing material is essential to obtain the best RAE outcome.
The choice of the embolic agent depends mainly on technical aspects,
lesion type,
site of the lesion and primary goals.
According to the type of occlusion induced,
embolizing materials may be considered as temporary (re-absorbable) or permanent (not absorbable).
The site of embolization may be both large (proximal embolization) or smaller (distal embolization) vessel.
(Fig.4)
Temporary embolization (proximal and distal)
· Absorbable Gelatine Sponges are absorbed within certain amount of time leading to recanalization of the arteries that is beneficial in minimizing normal tissue damage.
It is usually obtained in the form of a sheet that is manually cut into 1-3 mm pieces,
depending on its requirement and induce a temporary vascular occlusion for 3-90 days.
· Autologous clot
Permanent distal occlusion
· Inert Microparticles/Micropheres provide distal occlusion with tissue necrosis; the majority of particles are available in a size range of 40 to 1200 micron and are supplied in apyrogenic sterile sodium solution.
There are physical and mechanical difference between each type of particles that can significantly influence clinical outcomes.
For any given embolization procedure,
each type of microparticles differs in the size and angiograpic end point.
Usually,
they are suspended in non-ionic contrast material that serves as a carrier and provides radio-opacity for delivery speed and site control in order to avoid non-targeted embolization,
thereby minimizing the risk of reflux.
There are different types of microparticles:
o Non-spherical PVA particles (nPVA) are the most commonly reported embolizing agents.
The weak point of nPVA particles are the variation in size of the particles and the general tendency to aggregate with possible micro-catheter obstruction and/or proximal vessel occlusion due to the unpredictable level of occlusion.
Moreover,
nPVA particles cause moderate perivascular inflammatory change and recanalization can occur after several months or years at the site of occlusion.
o Calibrated PVA microspheres (cPVA) show the principal advantage of a more predictable level of occlusion and a less tendency to aggregate in the micro-catheter lumen.
As nPVA,
cPVA are not absorbable and not compressible.
o Trisacryl-Gelatin Microspheres (TGMS) (Embosphere) are a relatively new not-absorbable,
hydrophilic,
collagen-coated particulate embolic agent.
They are compressible and therefore,
easy to deliver through micro-catheters and are less prone to aggregate in both vessels and catheters as demonstrated by various experimental and clinical studies.
Furthermore,
it seems that they are able to cause a more distal embolization when compared to PVA particles of the same size,
due to their compressibility.
· Liquid Embolic Agents have demonstrated high efficiency in generating permanent distal occlusion; however,
due to their high vascular navigation capability,
they must be used with caution to avoid reflux in non-targeted vessels.
There are different types of liquid agents:
o Glues derived from N-butyl-2-cyanoacrylate (NBCA),
are a fast and efficient not-absorbable,
not-radiopaque embolizing material.
Liquid monomeric cyanocrylate in converts to a solid long-chain polymer immediately after the contact with anionic substances such as plasma,
blood cells or endothelium.
The reaction proceeds so rapidly that the glue will solidify in a catheter unless a substance is added to extends the polymerization time.
The most commonly used agent is the Ethiodized oil (lipiodol,
Ethhiodol),
that has both the functions of carrier and visualization tool,
due to its radiopacity; according to the different cyanoacrylate to oil ratios (usually from 1:0.5 to 1:5) a different time of polymerization and penetration capability is obtained.
NBCA provokes a more intense inflammatory reaction and involve the wall of the vessel and the adjacent interstitial areas.
This inflammatory reaction ultimately leads to vessel necrosis,
fibrous ingrowth,
and permanent occlusion.
Risks of using NBCA include rapid polymerization and reflux resulting in proximal embolization,
with subsequent possible collateralization,
or not targeted embolization; catheter entrapment is theoretical but possible.
If the polymeralization time in too long,
the NBCA can pass into the venous circulation,
resulting in venous embolism.
o Onyx™ is a non-adhesive liquid agent composed of ethylene vinyl alcohol (EVOH) copolymer dissolved in dimethyl sulphoxide and mixed with micronized tantalum powder for radio-opacity.
Upon contact with blood,
it precipitates to form a cast that remains flexible for some minutes.
Consequently,
use of Onyx™ provides predictable embolization,
as compared with glue.
Permanent proximal occlusion
o Metallic coils exist in multiple combinations of shape (elical,
3D),
length and release mechanism (controlled or not controlled) and can be inserted either via regular catheters or micro-catheters.
They cause a proximal occlusion of the vessel,
but if smaller in side can be useful also for a distal vessel occlusion.
The correct choice of the coil is essential because larger coils can be unable to fit in small vessels and longer ones can retreat into not target vessels with the risk of an undesired occlusion.
o Vascular plugs comprise a detachable nitinol cage filled with thrombogenic polyester filaments.
Vascular plugs provide rapid embolization of large vessels and are ideal for high-flow situations.
Complications
RAE is generally considered a safe procedure,
with a relatively low complication rate compared to surgery,
but nonspecific and specific complications are described in literature.
Nonspecific complications
Complications not directly associated with the embolization procedure can occur as a result of endovascular manoeuvres,
such as groin haematoma/pseudoanerysm and arterial dissection or thrombosis.
Additional complications might occur as a consequence of exposure to radiographic contrast media,
such as contrast-induced nephropathy or anaphylaxis.
(Fig.5)
Specific complications
As already outlined inadvertent embolization of not targeted areas can result in extensive or minimal renal infarction,
as well as infarction to sites different from kidney such as adrenal glands and lower limbs.
The majority of these incidents were reported in the 1970s and 1980s,
when non-selective RAE was performed,
and are now considered rare due to the improvement of embolic agents and the increased awareness of the operators.
Due to their small size,
microparticles are contraindicated among patients with AVF because of the risk of induce venous embolism.