Subjects
A cohort of 40 patients with LRTI was recruited from the emergency department of a general hospital (Centro Hospitalar do Baixo Vouga,
Aveiro,
Portugal) and randomly assigned to conventional pharmacotherapy plus respiratory physiotherapy (EG – Experimental Group,
n=21; average age 57.0 years; σ=19.8) or conventional pharmacotherapy only (CG – Control Group,
n=19; average age 52.8 years; σ=17.6) for 3 weeks.
Patients of the two groups were diagnosed in accordance to figure 1.
The study received full approval from the Ethics Committee of the hospital (2010-4-14).
Before their enrolment,
patients were informed about the study and its goals.
Signed informed consent was then obtained.
Intervention
The intervention consisted of conventional medical treatment (i.e.
antibiotherapy,
bronchodilators and rest,
according to Woodhead et al.,
2011 [1]) for both CG and EG.
In addition,
patients of the EG underwent respiratory physiotherapy three times per week for three weeks (nine sessions) [1].
Each session,
which lasted approximately 60 minutes,
included three main components: breathing techniques,
exercise training and education [2,3].
Lung function and Imaging protocol
Patients performed thoracic CT scans and spirometry before and after the intervention.
Spirometry (i.e.,
Forced Expiratory Volume in the first second - FEV1,
Forced Vital Capacity- FVC and ratio FEV1/FVC) was acquired with a spirometer (MicroLab 3535,
CareFusion,
Kent,
UK) according to the international guidelines [4].
Thoracic CT scans were acquired on a Toshiba Aquilion 64 slices CT scanner using a reduced dose protocol,
with dose modulation.
Image reconstruction was performed with different slice thicknesses and kernels.
Segmentation
Segmentation was performed over the volume obtained with lung kernel,
1mm slice thickness,
using a customized region growing method implemented using the rapid prototyping platform MeVisLab (MeVis Medical Solutions AG [5]) to obtain the airway volume in the TBT.
The airway segmentation method started with the manual definition of one or more seed points in the trachea and 3D region growing,
using as initial inclusion condition the interval [-1300HU,
-925HU].
The process was repeated changing the upper threshold in 5HU steps,
until the optimum value for the threshold was found.
The optimum value for the threshold is the maximum value that allows to maximize TBT segmentation without extra-luminal leakage (misclassification of parenchymal voxels as being part of the TBT,
figure 2) [6,
7,
8].
The final TBT segmentation was obtained with a morphological operation (closing with kernel size 3) allowing to obtain a dense object.
Figure 3 shows the TBT segmentation of the same patient in the two CT exams (before and after intervention).
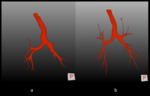
Using MeVisLab module ROIselect,
a blocking volume with arbitrary high value was placed on the distal part of the trachea at the Carina level (figure 4 - a) allowing to separate the Right Bronchial Tree (RBT) from the Left Bronchial Tree (LBT) and the segmentation process was repeated for the two sides (figure 4 - b).
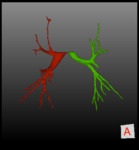
At the end of the segmentation process,
air volume in the TBT,
RBT,
LBT and BT (=LBT+RBT,
figure 5) were obtained.
In this study,
only BT volume was considered.
Data analysis
Descriptive statistics were undertaken to describe,
lung function (FEV1,
FVC and FEV1/FVC) and volumetric data (BT).
Comparisons between data obtained before and after intervention for the two groups were explored using a 2-way repeated measures ANOVA.
Analysis was performed using Statistical Package for the Social Sciences Version 22.0 (IBM Corp.,
Armonk,
NY,
USA).
The level of significance was set at 0.05.

![Fig. 2: HU interval settings for region growing. Leakage appears when inclusion condition is [-1330HU, -840HU] interval (a and b), therefore, final inclusion interval is set to [-1300HU, -845HU] interval (c and d). References: School of Health Sciences of the University of Aveiro, Aveiro, Portugal](https://epos.myesr.org/posterimage/esr/ecr2018/145655/media/769318?maxheight=150&maxwidth=150)