Pathologic conditions involving the falciform ligament
Related to the ligament content
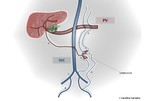
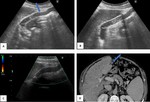
Paraumbilical veins as portosystemic collateral pathway in portal hypertension
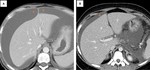
Paraumbilical veins contained in the falciform ligament establish communication between portal and systemic venous systems,
particularly between left portal vein and epigastric veins (Fig. 3).
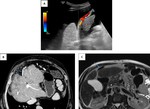
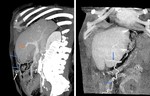
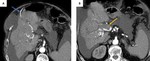
In portal hypertension,
a variable number of paraumbilical veins,
usually tiny and collapsed,
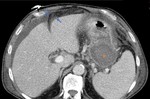
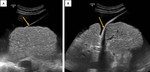
may enlarge to accomodate an hepatofugal flow in order to decompress the portal venous system (Fig. 4, Fig. 5,
Fig. 6). In this case,
they usually drain into a superior or inferior epigastric vein.
Paraumbilical collateral vessels may also drain into abdominal wall varices [7-10].
Cysts of the falciform ligament
Cysts of the falciform ligament are a rare entity whose etiology is unclear,
although in most cases it is thought to be congenital[2].
They can also be secondary to infection,
trauma or tumors with cystic changes.
Its presentation is variable,
ranging from asymptomatic to pain in the right upper abdominal quadrant,
dyspepsia or a palpable mass.
Ultrasonography or CT may suggest the diagnosis depicting a cystic mass near the fissure for ligamentum teres,
although the definite diagnosis is surgical and pathological[11].
Infarction of the falciform ligament
Torsion of the falciform ligament or of a fatty appendage of the falciform ligament leading to fat infarction is a rare cause of acute abdomen pain.
Similarly to torsion and/or infarction of omentum and epiploic appendages,
it is considered a form of intra-abdominal focal fat infarction (IFFI).
It presents with localized peritonism and often with normal laboratory tests.
Ultrasonography may show a heterogeneous and hyperechoic mass in the point of maximal abdominal tenderness.
CT usually depicts an area of fat density with slightly increased attenuation,
surrounded by inflammatory changes in the adjacent fat planes [12,13].
Related to the peritoneal nature of the ligament
Peritoneal mesothelioma
Peritoneal mesothelioma is a primary neoplasm of the peritoneum.
It is a very rare condition,
typically associated with asbestos exposure and affecting middle-aged men.
Disease may be localized and considered benign,
or disseminated along the peritoneal surfaces and,
thus,
malignant.
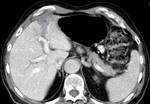
CT features of malignant mesothelioma include nodular peritoneal thickening and/or relatively well-defined masses revealing some enhancement and occasionally associated with focal calcifications.
These findings are mostly seen in the anterior parietal peritoneum,
with which the diaphragmatic edge of the falciform ligament is continuous and thus can be involved [14,15].
Pseudomyxoma peritonei
Pseudomyxoma peritonei is a condition that results from intraperitoneal rupture of mucin-producing tumors,
usually with origin in the ovary or the appendix.
It is characterized by accumulation of mucinous,
gelatinous material in the peritoneal cavity and its recesses,
whereby the falciform ligament may be involved [4,15].
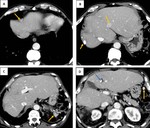
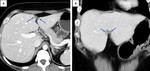
CT features include multiple hypoattenuating intraperitoneal masses of variable sizes that typically cause scalloping of the visceral surfaces,
particularly the liver (Fig. 8).
This latter feature is useful in the distinction from simple ascites,
as well as the presence of septations within the mucinous material.
Calcifications are frequently present and may display a curvilinear morphology that indicates the diagnosis.
In ultrasonography,
this condition manifests as hypoechoic intraperitoneal masses [14,15].
Peritoneal carcinomatosis
Peritoneal carcinomatosis corresponds to the malignant tumoral seeding of the peritoneum.
Most frequently it arises from primary carcinomas of the stomach,
colon,
ovaries,
gallbladder and uterus.
CT imaging studies may demonstrate a diffuse or nodular peritoneal thickening with variable enhancement.
Lesions may range from barely recognizable small nodules to bulky masses.
A common associated finding is the presence of ascites.
Tumoral implants are frequently seen in liver and spleen surfaces,
but scalloping is usually not so pronounced as it is in peritoneal pseudomyxoma [14,15].
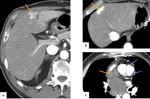
Metastatic implants may be seen along the falciform ligament,
particularly in its hepatic edge and near the fissure for ligamentum teres[14] (Fig. 9).
Splenosis
Splenosis is an acquired condition resulting from seeding of splenic tissue in the peritoneal cavity after an abdominal trauma or surgery involving the spleen.
The deposits of splenic tissue are usually small and grow on peritoneal surfaces[16].
As a peritoneal structure,
the falciform ligament can lodge splenosis foci (Fig. 10).
Related to direct extension from neighboring pathologic processes
Inflammatory processes such as pancreatitis and cholecystitis can extend directly by continuity to the falciform ligament (Fig. 11).
Pathologic conditions involving the falciform ligament region
Hepatic pseudolesions around the falciform ligament
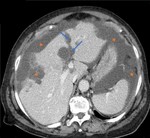
Hepatic pseudolesions around the falciform ligament are common and found in up to 20% of CT or MR imaging liver studies[17].
They are best visualized on contrast-enhanced portal venous phase images and appear as focal areas of low attenuation or signal intensity on CT (Fig. 12) or MR imaging studies,
respectively.
Initially they were thought to be related to focal fat infiltration,
but the signal intensity loss on opposed-phase MR images was demonstrated in only a minority of patients[18,19].
Currently,
the most supported hypothesis defends that these pseudolesions arise from hemodynamic changes related to an unusual venous drainage.
In addition to the normal hepatic dual blood supply – the hepatic arterial and the portal venous systems –,
some areas of hepatic parenchyma are also supplied by another venous system whose flow dilutes the portal perfusion at these locations,
originating pseudolesions.
In this specific case,
the “third blood inflow” is provided by the paraumbilical veins,
particularly branches from the inferior group of Sappey’s veins,
which drain venous blood from the anterior abdominal wall directly into the liver parenchyma near the falciform ligament.
These hemodynamic changes may also explain the metabolic changes occurring in some pseudolesions,
such as focal fat infiltration[6].
The “hot spot” hepatic pseudolesion in superior vena cava obstruction
In cases of chronic superior vena cava obstruction,
collateral pathways develop in order to preserve the venous drainage.
Although unusual,
some of them are cavoportal collateral pathways[20].
The superior vena cava and the portal vein may communicate via the internal thoracic vein,
the superior epigastric vein and paraumbilical veins (typically the superior group of Sappey’s veins)[6].
The blood deviation through this collateral pathway may lead to areas of increased blood flow to the liver,
particularly to the segment IV.
On nuclear medicine studies,
this may result in a focal area of increased radiopharmaceutical uptake in that hepatic segment,
known as the focal hepatic hot spot sign[20].
On contrast-enhanced CT studies,
the equivalent finding is a strong enhancement of the same area,
simulating an hypervascular hepatic lesion[17] (Fig. 13).
Conditions compromising the subphrenic spaces near the falciform ligament
Air or fluid occupying subphrenic spaces may outline a normal falciform ligament,
resulting in peculiar imaging features.
Pneumoperitoneum
Pneumoperitoneum is defined as free gas in peritoneal cavity and usually results from perforation of an intraperitoneal hollow viscus.
Free gas within the peritoneal space is frequently seen anterior to the liver[4] and,
therefore,
may outline the falciform ligament.
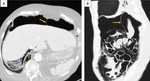
This finding may be easily depicted on CT imaging studies (Fig. 14).
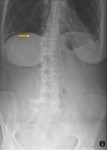
In the plain abdominal radiography,
if there is enough amount of air outlining the falciform ligament,
this structure may be individualized – it is called the falciform ligament sign,
also known as the Silver sign (Fig. 15).
Ascites
Ascites is defined as an abnormal amount of fluid within the peritoneal cavity.
It has diverse etiologies,
the most frequent being decompensated chronic liver disease,
followed by peritoneal carcinomatosis and cardiac failure [4].
The distribution of ascitic fluid is determined by peritoneal reflections,
body position and gravity[14].
Depending on its amount and origin,
ascitic fluid may be found in the perihepatic space outlining the falciform ligament,
a feature that US (Fig. 16),
CT (Fig. 17) and MR imaging studies may clearly display.