I. Epidemiology
The patients recruited for the study had a median age of 47,
with extremes ranging from 13 to 74 years old.
The distribution of the population of our study by sex has shown a clear prevalence of NPC in men (n = 94) compared to women (n = 49) with a sex ratio of 1.92.
We noted that the ganglionic syndrome is the most frequently observed at the time of diagnosis,
found in 76.3% followed by rhinologic syndrome in 74.9%,
then otological syndrome in 66.5% and in the last position comes the neurological syndrome found in 57.4%.
UCNT was the predominant histologic type with 62.3%,
followed by poorly differentiated carcinoma of the Nasopharynx in 37% then well differenciated carcinoma in 0,7%.
II. Imaging
A. CT of the nasopharynx
A nasopharyngeal CT scan was performed in 119 patients,
or 83.2%.
It allowed specifying the tumoral extension,
to classify it as well as to evaluate the cervical lymph nodes involvement.
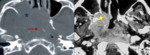
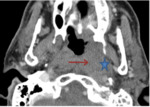
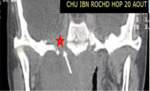
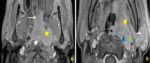
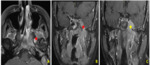
1. Tumor site (fig.
1)
The thickening of the walls of the nasopharynx was noted in 70.5%.
The imaging revealed the presence of a nasopharyngeal tumor process that affected the posterior wall (n = 63/ 52.3%),
the left lateral wall (n = 46/38.2%),
lateral right (n = 35/29.1%),
superior wall (n = 25/20.8%) and all the walls (n = 2/1.7%).
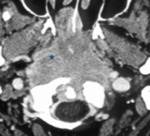
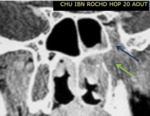
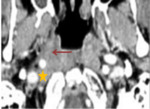
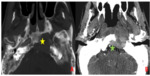
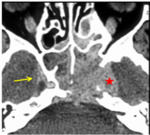
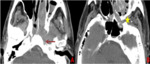
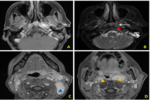
2. Local tumor extension (fig.2-4)
The tumor was confined to the nasopharynx (n = 27 so 22.5%).
3. Lymph nodes invasion
The supraclavicular involvement was noted in 11 patients or 7.7%,
whereas the retro-pharyngeal involvement was objectified in 09 patients or 6.3%.
The lymph node involvement was unilateral in 35 patients,
24.5% and bilateral in 58 patients (40.6%).
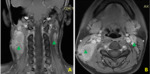
B. MRI:
MRI was performed in 32 patients (22.4%).
1. Tumor site
The thickening of the nasopharyngeal walls was present in 18 patients (12.6%).
The imaging revealed the presence of a tumour that affected the posterior wall (n = 14),
the left lateral wall (n = 12),
the upper (n = 9),
the right lateral wall (n = 9) and all the walls (n = 3).
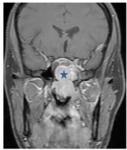
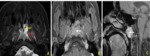
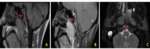
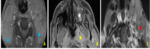
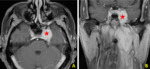
2. Local tumor extension (fig.
5)
The tumor was confined to the nasopharynx (n = 5) or 3.5%.
3. Lymph nodes invasion
It was noted that the most affected lymph nodes chain was chain III in 17 cases,
followed by the chain IIa-IIb noted in 16 cases,
the chain IV in 13 cases,
the chain V in 8 cases,
the chain Ia in 4 case,
then the chain Ib and VI found in only one patient.
The retro-pharyngeal involvement was noted in 7 patients,
supraclavicular involvement in 4 patients.
The involvement was bilateral in 15 patients (10.5%) and unilateral in 11 patients (7.7%).
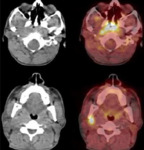
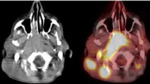
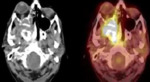
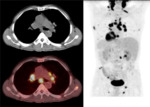
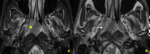
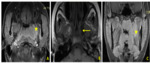
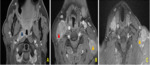
C. PET scan (fig.
6-9)
In our series,
23 (16.1%) patients underwent PET scans,
and 22% (95.7%) of these patients had cavernous hyper-metabolism.
Extension sites were: skull base (n = 12/52.2%),
endocranium (n = 5/21.7%),
parapharyngeal fat (n = 4/17.4%),
sphenoid bone (n = 4/17.4%),
choanes (n = 3/13%),
oropharynx (n = 3/13%),
nasal cavities (n = 2/8.7%),
orbit (n = 2/8.7%),
maxillary sinus (n = 2).
According to the UICC TNM classification,
the tumor was classified as follows:
T1: 34.8%,
T2: 4.3%,
T3: 39.1%,
T4: 21.7%.
Lymph node invasion was found in 19 patients,
ie 13.3%.
We noted that the most affected lymph node chain was the chain II in 17 patients,
followed by the chain III and IV noted in 14 cases,
the chain V in 06 cases,
then the chain Ia in 02 patients,
the chains Ib and VI have not been found in any patient.
The lymph node involvement was bilateral in 78.9% and unilateral in 21.1%.
No retro-pharyngeal lymph node involvement has been objectified.
According to the UICC TNM classification (Appendix 3),
lymphadenopathies were classified as follows:
N0: 17.4%,
N1: 17.4%,
N2: 52.2%,
N3: 13%.
A distant extension was noted in 14 patients (9.8%),
it was bone (n = 7),
pulmonary (n = 5),
mediastinal (n = 4) and hepatic (n = 2).
III. TNM classification and UICC / AJCC stadification
A.
TNM classification (fig.
10-26)
After the clinical,
pathological and para-clinical study,
our patients were classified according to the TNM classification adopted by the UICC 7th edition.
1. Tumor
The majority of the patients found in our series were classified T2 in 53 cases,
T3 in 41 cases,
T1 in 28 cases and T4 in 21 cases.
T1 (n=28),
T2 (n=53),
T3 (n=41),
T4 (n=21).
2. Nodes
With regard to lymph node involvement,
56 patients were classified N2,
41 patients classified N1,
27 patients classified N0,
15 patients classified N3b and 04 patients classified N3a.
N0 (n=27),
N1 (n=41),
N2 (n=56),
N3 (n=19).
3. Metastasis
98 patients had no secondary locations (M0),
23 patients were classified positive metastases (M1),
while in 22 patients the metastatic status was not specified (Mx).
Mx (n= 22),
M0 (n=98),
M1 (n=23).
B.
Classification in stages
In our series,
58 patients consulted at stage III of their disease,
45 stage IV patients,
31 stage II patients,
while only 09 patients consulted at stage I of their disease.
IV. Concordances
The number of patients who had CT,
MRI (n = 08),
and PET scanner (n = 10) at the same time is unrepresentative and can not be used to draw meaningful conclusions about comparison between its different modalities.
A.
CT / MRI
08 patients in our series benefited from an MRI and a CT scan.
For the T: We took MRI as a reference
- A good concordance of 78.3% in T1 and T3,
a moderate concordance of 57.7% in T2.
- TDM overestimated T3 and underestimated T2.
For the N: We took MRI as reference
- A very good concordance of 88.6% in N0 and N3,
a good concordance of 76% in N1 and N2.
- CT underestimated N1,
N2 and N3.
B.
IRM / PET SCANNER
In our series 10 patients underwent an MRI and a PET scanner.
For the T: We took MRI as reference
- A very good agreement of 90% in T1 and T2,
a good concordance of 75% in T3.
- PET overestimated T1 and T2 and underestimated T3 and T4.
For the N: We took pET scan as reference
- A good agreement of 78.6% for all N.
- MRI underestimated N2 and N3.