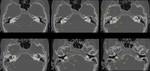
For the assessment of temporal fractures,
cranial CT is a fundamental initial diagnostic modality because of its speed and accessibility.
If a temporal fracture is suspected,
we have to perform multi-planar reconstructions with the bone window.
ANATOMY OF THE TEMPORAL AREA
Temporal bone has a complex anatomy,
divided into five bony divisions,
which include the squamous part,
the petrous bone,
the tympanic part,
the mastoid process,
and the styloid process.
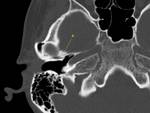
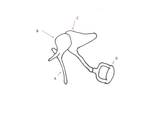
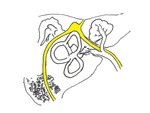
Internal anatomy (Fig.
01)
It comprises various structures,
such as:
- Cranial nerves: CN V (semilunar ganglion,
or Gasser's ganglion),
VI,
VII and VIII;
- Vascular structures: jugular bulb and the carotid canal;
- Auditory and vestibular structures: external auditory meatus (EAM),
eardrum (tympanic membrane),
auditory ossicles,
cochlea,
vestibular organs and the internal auditory canal or meatus (IAM).
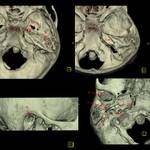
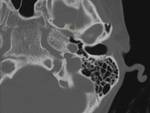
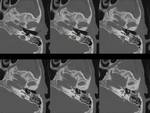
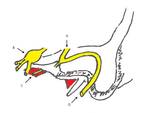
External anatomy (Fig.
02)
Temporal bone is a pyramid-shaped structure at the base of the skull,
with its apex (the petrous apex) pointing anteromedially and its base located posterolaterally.
The external part is composed of the auricle and the external opening of the EAM.
On the superior wall there is a relief,
the arcuate eminence,
which represents the protrusion of the underlying superior semicircular canal,
while the semilunar ganglion (of Gasser) is located towards the apex.
On the posteromedial wall,
there is the opening of the IAM and the cochlear and vestibular aqueducts.
The inferior wall contains the styloid process,
the jugular fossa,
the external opening of the carotid canal and the stylomastoid foramen,
the exit point of the facial nerve.
Attention! Pitfalls!
As it is a complex structure consisting of five segments joined by sutures,
these sutures can confuse the physician and lead to the diagnosis of pseudo-fractures.
To distinguish them,
it is usually sufficient to remember that the sutures have a zig-zag pattern and sclerotic borders. In any case,
we will clarify what kind of sutures can easily lead to errors.
Extrinsic sutures
They unite the temporal bone with the other cranial bones:
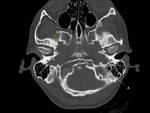
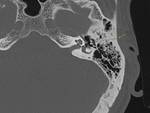
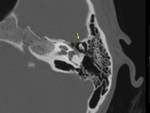
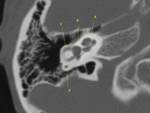
- Occipitomastoid suture (Fig.
03): Given the variability that exists in the formation of this area during development,
the occipitomastoid suture may be asymmetric or even bifid.
In order not to confuse us,
we have to follow its course from the postero-inferior segments,
where it adopts a zig-zag pattern.
- Sphenosquamosal suture (Fig.
03): It is formed between the greater wing of the sphenoid bone and the squamous part of the temporal bone,
easily recognizable because it is located laterally to the foramen spinosum.
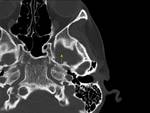
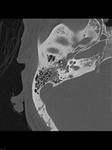
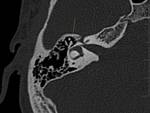
- Sphenopetrosal suture (Fig.
04): It is located between the posterior margin of the greater wing of the sphenoid bone and the petrous apex,
posterior to the foramen ovale and the bony part of the Eustachian tube.
Intrinsic sutures
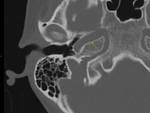
- Tympanosquamous (Fig.
05): It is located in front of the EAM and continues in the antero-medial direction as the petrotympanic suture.
- Petrotympanic suture (Fig.
06): We can identify it following the tympanosquamous suture,
or locate it anterior to the bony part of the Eustachian tube
CLINICAL SIGNS AND SYMPTOMS
The signs and symptoms that may manifest in temporal fracture are hemorrhagic or cerebrospinal fluid otorrhea,
hemotympanum,
perforation of the tympanic membrane,
vertigo,
hearing loss,
facial paralysis and nystagmus.Battle's sign, a retro-auricular ecchymosis,
may be present due to the rupture of a mastoid emissary vein.
CLASSIFICATION
Classical classification
The classical classification of temporal bone fractures was devised in 1926 by Ulrich et al.,
and it continues to be the most widely used.
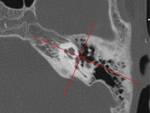
It divides fractures into longitudinal and transverse,
taking the longitudinal axis of the petrosal pyramid as a reference (Fig.
07).
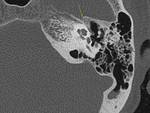
Longitudinal fractures
They are the most frequent (80-90%) type and are usually the result of temporoparietal trauma.
The fracture line extends from the lateral to the medial aspect,
parallel to the long axis of the petrous bone.
The otic capsule is infrequently compromised because the fracture line usually proceeds by way of lesser resistance towards the petrous apex,
anterior to the labyrinthine structures,
towards the middle cranial fossa (Fig.
08).
Fractures posterior to the otic capsule are less frequent,
they advance towards the jugular fossa and the posterior cranial fossa.
The most commonly associated complications are: impairment of the EAM,
hemotympanum,
tympanic membrane rupture,
blood or CSF otorrhea,
and lesions of the auditory ossicles (Fig.
09).
Hearing complications are related to conductive hearing loss.
Although less likely,
the facial nerve may also be affected in its tympanic and mastoid segments.
Transverse fractures
They are linked to severe fronto-occipital trauma and are less frequent (10-20%).
In this case,
the fracture line proceeds perpendicular to the long axis of the petrous bone,
from the jugular fossa to the middle cranial fossa.
There are two types of fractures: the medial ones at the arcuate eminence, which are more commonly related to the injury of the IAM, and the lateral ones that can cross the bony labyrinth, damage the base of the stirrup and cause a perilymphatic fistula.
Both are connected with sensorineural hearing loss (Fig.
10).
Facial paralysis is more common in this fracture type,
and it may be immediate and complete.
This classification was reinforced by a series of works by Grudjan et al.
in 1940s and has established itself as the most widely used. That said,
however,
these studies were performed on cadavers in the laboratory,
in a controlled environment very different from real-life traffic accidents.
This classical classification has limitations since most temporal bone fractures have elements of both patterns. In addition,
it has not shown a good correlation with the clinical signs and symptoms and potential complications.
In 1992,
Ghoraleb and Yeakley tried to complete it by introducing the concept of a mixed or oblique fracture (Fig.
11),
which,
although it allows for a more accurate anatomical description,
does not resolve the gaps in the clinical correlation.
New classifications
New classifications followed later on.
The one with the best clinical correlation was proposed by Kelly and Tamy in 1994.
Otic capsules-violating and otic capsule-sparing fractures
This classification is complementary to the previous ones and depends on the compromise of the bony labyrinth (cochlea,
vestibule and semicircular canals) (Fig.
12).
Fractures that do not injure the otic capsule are much more common (94-97%).
They are the result of the temporoparietal trauma and associated with a higher incidence of conductive hearing loss due injury of the chain of auditory ossicles.
Fractures that injure the otic capsule are less frequent (3-6%).
They usually occur secondary to occipital blows and have a higher incidence of sensorineural hearing loss,
facial paralysis and CSF fistula formation.
POSSIBLE AFFECTED STRUCTURES AND COMPLICATIONS
Although we know that the classification of fractures is a useful tool for predicting possible complications and planning their treatment,
simply categorizing them is not enough.
It is also necessary to include a detailed description of the structures involved.
When we do not see any fracture lines,
we must look for the indirect signs,
such as the opacification of mastoid cells or tiny peritemporal air bubbles.
EXTERNAL AUDITORY MEATUS
The external auditory meatus is an "S"-shaped structure pointing in the antero-superior direction.
Its outer third is cartilaginous and deformable,
while the two internal thirds are osseous.
Its front wall forms the back wall of the glenoid fossa,
the point of articulation of the mandibular condyle.
In trauma involving the jawbone,
we must pay particular attention to the possibility of the compression of the condyle,
which can in turn lead to anterior wall rupture.
Auditory ossicles
The chain of ossicles is comprised of the malleus,
incus and stapes.
The handle of the malleus is immersed within the tympanic membrane and its head articulates with the body of the incus,
which branches into two branches (the short and the long branch).
The long branch of the incus articulates with the stapes,
whose base communicates with the oval window,
thus closing the sound transmission circuit.
(Fig.
13)
The incus has a rather poor ligament support,
which is why its joints dislocate more frequently.
The most frequent lesion of the ossicles is the incudo-malleolar dislocation,
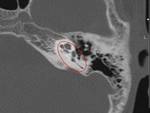
followed by complete dislocation of the incus. In the axial CT,
the configuration of the incudomalleolar articulation resembles the shape of an ice-cream cone (Fig.
14),
the ice cream corresponding to the malleus head and the cone to the body and short process of the incus.
The loss of this form indicates a lesion of the auditory ossicles (Fig.
15).
Carotid canal
The petrous apex of the temporal bone contains the petrous segment of the internal carotid artery (c2),
which enters the skull through the carotid foramen.
Patients presenting with carotid canal impairment are at risk of injury to the internal carotid artery,
with complications such as arterial dissection,
pseudoaneurysm,
complete severance,
as well as arteriovenous occlusion or fistula.
Whenever a fracture affects the carotid canal,
an angio CT should be performed to assess the carotid artery (Fig.
16).
Facial nerve
It originates just before the vestibulocochlear nerve (CN VIII) in the anterior part of the protuberance and accompanies it through the pontocerebellar angle and IAM to the petrous bone.
Once inside the temporal bone,
it follows an anterolateral course and bends abruptly into the geniculate ganglion,
the point of exit of the greater petrosal nerve,
and heads in the posteroinferior direction,
passing through the angle formed by the lateral and superior semicircular canals,
and entering the mastoid and passing vertically to exit the facial canal (and the cranium) via the stylomastoid foramen (Fig.
17).
Along its long course within the temporal bone,
it can be injured mainly in fractures affecting the otic capsule.
Transverse fractures more frequently injure its geniculate and labyrinthine segments,
while the longitudinal fractures tend to damage the mastoid segment. The lesion does not always directly affect the nerve; it can also be damaged by edema or bleeding of the surrounding area.
Other cranial nerves: CN VI and CN VII (Fig,
18)
The trigeminal ganglion (or Gasser's ganglion) occupies the anterosuperior part of the petrous apex.
Hence,
it can be damaged in fractures of the petrous bone.
The external oculomotor nerve is introduced in the lateral cavernous sinus into ICA and continues its path towards the orbit.
It can be damaged by fractures that affect the cavernous sinus.
Cochlea (Fig.
19)
It is located in the anterior part of the otic capsule,
shaped like a spiral.
It is easily distinguished by the high density of the surrounding bone.
Injury to the cochlea,
cochlear nerve or cochlear nuclei can cause sensorineural hearing loss.
In patients with sensorineural hearing loss without evidence of a fracture, the hearing loss may also be due to cochlear contusion.
Vestibule and semicircular canals (Fig.
19)
The vestibule is the central organ of the bony labyrinth,
communicating with the cochlea at the anterior aspect and with the semicircular canals at the posterior aspect.
It contains the utricle and the saccule,
the organs of equilibrium related to linear acceleration.
There are three semicircular canals – they display an orthogonal configuration (lateral,
superior and posterior) and are involved in angular acceleration.
Injury to any of these structures,
the aqueduct or the vestibular nerve,
will cause vertigo.
If a fracture line cannot be identified in patients presenting with vertigo,
we must also think about the possibility of a perilymphatic fistula,
cupulolithiasis or labyrinthine contusion.