Various imaging techniques can be used for diagnosis of PNSTs.
Ultrasonography is an easy and repeatable imaging modality,
useful in superficial lesions but unsuitable for deep lesions [8].
CT allows evaluation of bone involvement,
encasement of blood vessels and tumor staging.
MRI,
thanks to its high contrast resolution in characterization of different tissue properties,
is considered the modality of choice in the study of PNSTs.
Furthermore,
due to the absence of radiation exposure and the possibility to identify features associated with malignant transformation,
MRI can be used for follow-up of individuals with plexiform neurofibromas [9].
Typical features of PNSTs are the relationship to the nerve,
the fusiform shape with tapered end and the associated muscle atrophy [10].
BPNSTs
Benign tumors show an expansive growth pattern with regular margins and a tumor size < 5 cm,
schwannoma is an encapsulated tumor that grows eccentrically to the effected nerve while neurofibroma arises from the nerve fascicle,
is centrally located and is rarely encapsulated in fact it cannot be separated from the involved nerve [11].
On CT BPNSTs are hypodense relative to muscle (5-25 HU) because of the high lipid content of myelin from Schwann cells.
On MRI lesions are isointense relative to muscles on unenhanced T1-weighted sequences and have a signal higher than fat on T2,
T2-weighted sequences are particularly useful to identify:
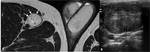
- “fascicular sign”: appearance of the fascicular bundles with multiple hypointense ring-like structures within the hyperintense lesion (Fig. 1).
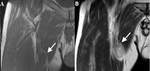
- “target sign”: a low signal intensity centrally and high signal intensity peripherally,
corresponding to central fibrous components and peripheral myxomatous elements; central enhancement is related to the presence of target sign (Fig. 2) [11,12].
The “split fat sign” is a rim of fat that surrounds the lesion,
better seen on T1 weighted sequences and also seen on T2 (Fig. 3).
These signs are frequently associated to PNSTs but are not specific for BPNSTs; fascicular sign corresponds to neurogenic origin of tumors,
target signs represents a typical feature,
even if not pathognomonic,
of neurofibromas and split fat sign suggests that tumor originates in the intermuscular space [4].
A heterogeneous appearance with degeneration and cystic changes is more common in schwannomas,
especially ancient ones,
than in neurofibromas [10].
Plexiform neurofibromas are pathognomonic for NF1,
usually involve a long segment of a major nerve trunk,
extend into the nerve branches and they result in the so-called bag of worms appearance on gross and cross-sectional,
as well as malignant forms may show heterogeneity and bone erosion [7,13].
MPNSTs
Malignant tumors involve medium to large deep-seated nerves: sciatic nerve,
brachial plexus,
and sacral plexus; the most frequent localization is trunk for some authors and extremities for others,
without a full agreement in literature [14,15].
Many authors searched to find some radiological findings typical of malignant forms suggesting that these following features are most commonly identified in MPNSTs (Table 2):
-tumor size > 5 cm
-rapid and infiltrating growth pattern with ill-defined margins
-perilesional edema
-central necrosis with peripheral enhancement [3,16,17].
MPNSTs are typically heterogeneous on both unenhanced and intravenous contrast material-enhanced CT and MR acquisitions due to the presence of variable amount of necrotic tissue within the tumor [18] (Fig. 4 - Fig. 5).
Intratumoral cystic change,
with hyperintense T2 signal,
is commonly found in schwannomas and rarely seen in neurofibromas; this feature may help in the differentiation of neurofibromas from MPNSTs,
in which malignant transition may result in the presence of necrosis and/or hemorrhage [3].
Chhabra et al.
also found that MPNSTs in patients with NF1 show a higher incidence of cystic/necrotic degeneration compared with sporadic forms.
However,
a large overlap in radiologic features between benign and malignant tumors remains,
because MPNSTs can show an expansive growth pattern,
fascicular and split fat sign (often incomplete).
Furthermore,
heterogeneity and bone erosion may be also present in benign forms [4,7,11,18].
Doubtful cases with suspected malignancy require biopsy sample.
Pathologic Evaluation
Gross inspection of MPNSTs reveals a globoid or fusiform shape mass with mean size usually > 5 cm,
a typically tan-gray color and,
on cut section,
necrosis and areas of cyst formation are commonly present; MPNSTS may be also surrounded by portions of plexiform neurofibroma which have not yet undergone malignant transformation.
At histologic analysis they are constituted by spindle cells organized in fascicles,
high-grade tumors tend to have high mitotic activity and necrosis [18] (Fig. 6 Fig. 7 Fig. 8).