The authors gathered imaging findings of hemodialysis access challenges in mapping and follow-up.
Patients were studied with Eco-Doppler,
contrast-enhanced CT (dialysis patientes) ans MR without gadolinium (chronic renal disease).
1.
PREOPERATIVE EVALUATION - CHECKPOINTS
Complete clinical history (including the cause of the renal failure),
is important to determine the urgency of which access is needed to be constructed.
It is also important to know if patient was submitted to previous endovascular therapeutic procedures and evaluate the patency of vessels.
Recognizing the presence of atherosclerosis will allow a correct selection of the artery for the construction of a fistula.
The success of an arteriovenous fistula (AVF) depends on having a healthy feeding artery and doing the correct determination of the better outflow vein.
Eco-Doppler before AVF creation has proven to increase the success rate of arteriovenous fistula placement and maturation5.
Thus,
vessel mapping with eco-Doppler is recommended to all patients waiting for a AVF surgery construction6.
1.1 MAPPING
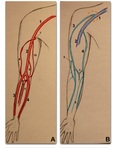
Variations in the origin and configuration of the arteries in the upper limb are often present and it has important clinical and surgical implications.
Description of the vascular pattern of upper limb Fig. 2 ,
including anatomical variants of the origin,
course and branching is very important to plan surgical construction of the vascular access.
1.1.1 Arteries
1.1.1.1 Brachial Artery
Brachial artery7 usually assumes two terminal branches patterns Fig. 2 :
a) 2 divisions - ulnar artery and median-interosseous arterial trunk
b) 3 divisions – ulnar artery,
radial artery and common interosseous artery and median artery
Arterial variation in the upper limb has been firstly documented by von Haller,
in 1813.
An uncountable number of arterial variants are perceived in the human brachio-antebrachial arteries.
Thus,
arm arterial variants include:
A) Brachial artery in front of the median nerve that continues as
a) Arteria brachialis superficialis superior
b) Arteria brachialis inferior
B) Double brachial artery i.e.,
superficial and deep:
a) Brachialis superficial superior
b) Brachialis inferior:
I) Superficial and deep reunite
II) Superficial continues as the radial:
i) without anastomosis
ii) with anastomosis
C) Superficial brachial continues as
a) Ulnar
b) Median
c) Ulnar and Median
D) Superficial brachial as the radial and superficial antebrachial
There are three superficial brachial artery subdivision types Fig. 3 :
A) Bifurcation into ulnar and radial artery in cubital fossa
B) High origin of the radial artery (when superficial brachial artery continues as radial artery)
C) High origin of the ulnar artery (when superficial brachial artery continues as ulnar artery)
Profunda brachial artery has different origin levels and subdivisions.
1.1.1.2 Radial Artery7
Origin proximal to the intercondylar line is the greatest radial artery variant.
There are two types of variants:
A) Single dorsal division and entirely superficial
B) Dorsal division and subsequent division into 2 branches (superficial and deep)
Anastomotic connection types:
A) No gross anastomosis
B) Anastomosis with the deep or regular brachial artery in the antecubital region.
Communicating vessel is anterior to the biceps tendon
C) Anastomosis with brachial artery.
Communicating vessel is posterior to the biceps tendon
D) Anastomosis with median artery in the forearm
Atypical radial artery arises from the axillary artery,
gives thoracoacromial trunk and a second branch more distally,
which gives lateral thoracic artery proximally,
and the thoracodorsal artery and typical radial artery,
as the sole contribution to the deep palm arch and no contribution to the superficial palmar arch.
1.1.1.3 Ulnar Artery7
High origin of superficial ulnar artery is often unilateral.
1.1.2 Veins
The main venous return of the upper limb is done by the basilic vein.
All the others converge to it.
Usually,
basilic vein drains to brachial venous system to finally join axillary vein Fig. 2 .
In other patients,
basilic vein drains into the brachial venous system in the distal third or in the middle of the upper limb.
Cephalic vein classically originates from the dorsal venous network of the hand and runs through the radial aspect of the forearm.
It usually occupies deltopectoral muscle groove and ends in axillary vein Fig. 2 .8
The cephalic vein was found to be of two types:
A) In most cases the cephalic vein gives rise to the median cubital vein
B) In a smaller group,
the cephalic vein receives median cubital vein from the median antebrachial vein
The median cubital vein may be doubled.
There are two main variants in the termination of the cephalic vein:
A) The cephalic crosses the distal third of the arm to join the basilic vein
B) The cephalic vein continues with the median cubital vein and then drains to the basilic vein
Median antebrachial vein may terminate:
A) More often in basilic or median cubital veins
B) After divided in vena mediana basilica and vena mediana cephalica – “M-shape”
In almost 50% of cases,
oblique vein leaves the origin of the basilic vein to join the cephalic one.
Accessory cephalic vein is a variable vein that passes along the radial of the forearm. Fig. 5
Parallel and proximally to the oblique vein,
an accessory cephalic vein can arise from the basilica vein to join the cephalic vein.
Absence of cephalic or basilica vein and duplication of the axillary vein can also be seen.
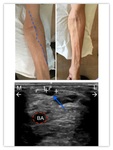
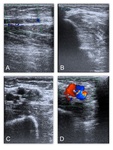
The Doppler ultrasound evaluation shows basilic and cephalic veins running in a fascial folding.
1.2 DEEP VEINS
Sometimes,
patients initiating dialysis have adequate arterial and venous vessels for construction of an arteriovenous fistula,
but they may be too deep to cannulate,
because of the amount of adipose tissue.
Liposuction and vessel transposition are used to superficialize deep arteriovenous fistulas.9
Lipectomy is done in obese patients to superficialize radio-cephalic fistulas.
Basilic vein superficialization is mandatory for brachial-basilic arteriovenous fistula.
Superficialization is usually performed in a second surgical procedure.
Because of the substantial risk of serious surgical complications,
superficial veins are preferred as first option.
1.3 VEIN DEPLETION
Long term use of vascular access in dialysis patients lead to different complications that drive patient to venous depletion. Progressive loss of multiple vascular access forces systematic search for alternative sites,
in order to maximize patient survival.
Fig. 6
Exhaustion of the upper limb vessels predisposes to creation of exotic AVFs.
2. IMMEDIATE POST VASCULAR FISTULA CONSTRUCTION AND FOLLOW-UP
Nowadays,
surgeons often perform end-to-side anastomosis.10
Vascular access is responsible for the increase of blood flow in the venous system.
Before the surgery,
the venous pressure is about 20mmHg; after surgery it increases to 60-120mmHg.
Thus,
it is important to use surgical techniques that reduce the amount of turbulence and endothelium injury.11
Immediately after surgery,
the most probable complications are hemorrhage,
low venous flow and hematoma Fig. 7 .
At a later stage,
infections,
aneurysm and pseudoaneurysm development,
vascular access stenosis,
congestive heart failure,
steal syndrome,
ischemic neuropathy and thrombosis may occur.
2.1 INFECTIONS
Arteriovenous grafts have a much higher rate of infection than arteriovenous fistulas.12 AVF infections usually resolves with antibiotherapy.
It is usually characterized by perivascular cellulitis.
When associated to aneurysm,
hematoma or abcesses,
it requires drainage / surgical excision.
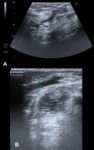
Ultrasound examination reveals edema and soft tissue collections.
Diminished flow and vein thrombosis can be associated. Fig. 8
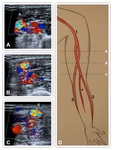
2.2 STENOSIS
Stenosis is the most common complication of a vascular access.13 It can affect morbidity and mortality of patients.1,2
Indications to treat stenosis depend on the location and the hemodynamics of the arteriovenous fistula.14 Fig. 9
Treatment options include Percutaneous transluminal angioplasty (PTA) and surgery.
PTA is the preferred approach15: it is less invasive,
more reproducible and can more frequently spare the access.
Inflow stenosis complies the arterial limb,
from the origin of the subclavian artery to the anastomotic and juxta-anastomotic vein region.
The last one (anastomotic and juxta-anastomotic) are the most frequent type.
Stenosis are usually caused by atherosclerosis and Monckenber’s medial calcification.3,
16
Inflow stenosis is characterized by reduced flow along the stenosis.17
However,
if there is no low flow (<0,5mL/min) nor significant drop (>20%) in two consecutive assessments,
treatment is not necessary.14
A mid-vein stenosis can be complicated with aneurismal degeneration,
blood leakage after dialysis and skin necrosis.
Outflow stenosis,
namely graft-to-vein anastomotic stenosis,
is the most common complication of vascular access grafts,
and is characterized by decreased or low flow,
resulting in an increased risk of thrombosis.14
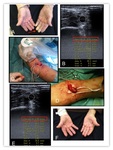
2.3 PSEUDOANEURYSMS
Pseudoaneurysms can be caused by different mechanisms:
A) Perioperatively,
in the anastomosis,
due to the presence of a leak of blood
B) Recurrent standard puncture with a dyalisis needle Fig. 10
C) Later complication of infection
D) After intervention Fig. 11
Pseudoaneurysms can be found in both arterial and venous sides of the hemodialysis access.
Pseudoaneurysms with less than 5 mm diameter are usually not clinically significant.
If greater than 5 mm,
pseudoaneurysms should be treated with surgery or embolization.
2.4 ANEURYSMS
Aneurysm is a focal enlargement of the vascular caliber.
Repeated punctures in the same vascular segment can weaken the vascular wall and lead to aneurysm formation.
Furthermore,
dilatation can naturally occur because of the high flow and high pressure within the fistula.
If not treated,
aneurysm can rupture and even be fatal due to exsanguination.18
2.5 THROMBOSIS
Thrombosis is a common early and late complication.
An increased thrombotic predisposition is an important cause of complications in hemodialysis patients.
Patency is important to achieve fistula maturation.
Early thrombosis should actively be prevented in order to increase the rate of fistula maturation.
The main cause of thrombosis of the vascular access is the proliferation of venous neointimal,
which drives fistula to stenosis and subsequent thrombosis.19
Early thrombosis is usually caused by wrong surgical options or Doppler measurements (inadequate sized draining vein or bad anastomotic technique).
It can also be caused by external compression,
dehydration and hypotension,
early puncture of an immature access.
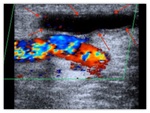
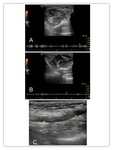
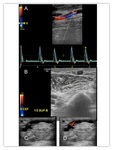
B-mode ultrasound can easily determine the presence of intraluminal clots (hypo or anechoic) and Color / spectral Doppler confirm the absence of blood flow. Fig. 12 Fig. 13
Late Thrombosis often results from acquired stenosis of the venous segment of the access.
It can also be caused by low vascular volume (dehydration,
hypotension),
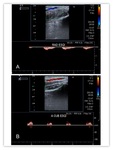
compression or trauma. Fig. 14 Fig. 15
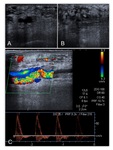
Late thrombosis can be complete or partial.
If complete,
Spectral Doppler presents with “to and fro” wave pattern.
Low peak systolic velocity,
absence of color Doppler signal,
and echogenic material within the vascular access are also common ultrasound findings on late thrombosis.
2.6 ISCHEMIC MONOMELIC NEUROPATHY
Although rare,
ischemic monomelic neuropathy is an important complication of vascular access and requires an early diagnosis and treatment.
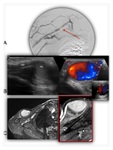
Ischemic Monomelic Neuropathy is characterized by “steal” blood flow from distal nerve tissue,
causing multiple axonal loss distally in the limb.20 Brachiocephalic fistula is often associated with this complication because brachial artery is the only blood suppliy of the distal arm. Fig. 12
Doppler ultrasound shows high flow.
Symptoms immediately after surgery are common: acute pain,
weakness and muscle paralysis,
which are nonspecific immediately after surgery.
Vascular access ligature is the treatment.
2.7 HIGH FLOW VASCULAR ACCESS
Excessive flow is defined as an arterial flow exceeding 1-1,5 L/min,
with a cardio pulmonary recirculation exceeding 20%.
It can lead to pulmonary edema,
recurrent pulmonary infections,
steal syndrome and heart failure.
Banding is a surgical procedure that allow to limit vascular access flow and pressure,
with the advantage of real-time intravascular monitoring.
It is also effective to treat vascular access steal syndrome. Fig. 16
2.8 VASCULAR ACCESS STEAL SYNDROME
Steal Syndrome is caused by reduced blood flow distal to the vascular access.
It occurs more frequently in diabetic and elderly patients.11
Steal syndrome usually occurs with large anastomoses,
with high blood flow.
It is more common in proximal access than distal.
It becomes symptomatic when compensatory mechanisms,
such as peripheral arteries,
are insufficient.
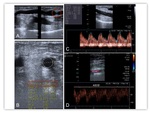
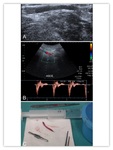
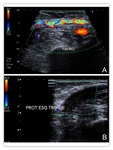
On Doppler ultrasound,
this entity is characterized by retrograde flow in the native artery,
distal to the anastomosis.
Flow can always be retrograde in the distal segment or bidirectional,
anterograde in the systole and retrograde in diastole. Fig. 17
Low resistance in vascular access veins and retrograde flow in palmar arch threatens adequate perfusion of the hand,
predisposing to ischemia.
A wide range of signs and symptoms may occur.
Some patients only have clinical manifestations during dialysis,
such as paresthesia,
pain and coldness.
Others can have pain at rest,
ulceration and tissue necrosis.
In severe cases,
steal syndrome may result in lower limbs,
bowel ischemia and heart failure.
Prevention must be the main objective.
Preoperative assessment and adequate post surgical follow up avoid unnecessary finger amputations.
There are multiple treatment options,
thus it depends on the severity of symptoms,
comorbidities and the experience of the surgical team.
2.9 CONGESTIVE HEART FAILURE
Cardiovascular disease is the leading cause of death in patients doing dialysis.
Left ventricular hypertrophy is the most common pathology in end-stage renal failure patients.
The construction of the vascular access increases cardiac output in 15% and 4% of the end-diastolic ventricular pressure.21