Keywords:
eHealth, Computer applications, RIS, PACS, Structured reporting, Outcomes, Multidisciplinary cancer care
Authors:
D. J. Vining1, A. Pitici2, C. Popovici2, A. Prisacariu2, M. Kontak2; 1Houston, TX/US, 2Houston/US
DOI:
10.1594/ecr2018/C-2771
Methods and materials
We developed a multimedia structured reporting system that works as follows:
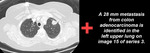
- Record key images and voice descriptions of findings (figure 3)
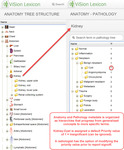
- Tag images using natural language processing (NLP) with metadata (figure 4) that is referenced to SNOMED-CT terminology (figure 5) and organized as hierarchies (figure 6)
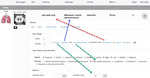
- Link related serial findings in timelines (figure 7)
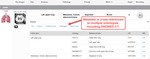
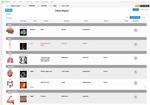
- Assemble a multimedia report organized by anatomical groups and/or medical priorities (figure 8)
- Filter information as required to produce a relevant patient problem list (figure 9)
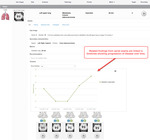
As illustrated in figure 6, each radiologic diagnosis is assigned a default Priority value on a 5-point scale to indicate a level of action required by a clinician:
- Insignificant (Can be ignored)
- Important (Needs serial monitoring)
- Indeterminate (Requires further evaluation to make a diagnosis)
- Urgent (Needs attention as soon as possible)
- Life-threatening (Needs immediate attention)
In the example in figure 8,
the concept of "Kidney Cyst" is assigned a default Priority value of 1 = Insignificant (can be ignored).
A radiologist has the option to modify the Priority value prior to report signoff.
To create an effective PPL,
the list should have the following attributes [4]:
- Accurate - Uses confirmed diagnoses
- Specific - Employs detailed coding
- Relevant - Addresses clinical needs
- Current - Excludes inactive problems
To achieve these requirements, the structured findings can be filtered to exclude insignificant and inactive findings from display. This interactive process results in a dynamic PPL using radiologic information.