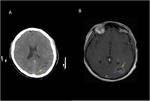
Radiology Features
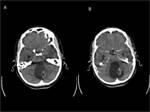
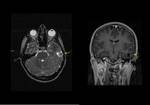
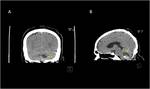
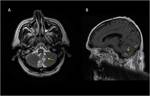
Pilocytic astrocytoma
Most common in the cerebellar hemispheres.
Other typical location is optic nerve/chiasm/tract.
In T1-weighted sequences,
the solid portion of the CMNT is iso/hypointense to gray matter while the cyst content is iso- to slightly hyperintense to cerebrospinal fluid (CSF).
In T2 and fluid attenuated inversion recovery (FLAIR) sequences,
the solid portion is hyperintense to gray matter while thecyst content is hyperintense to CSF.
In FLAIR sequences,
the cyst content is not suppressed.
The cyst wall occasionally enhances,
but cyst wall enhancement does not necessarily mean the presence of neoplastic tissue and removal of the cyst wall does not affect the outcome in the case of pilocytic astrocytoma.
Fig (1,2).
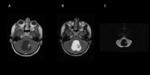
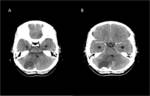
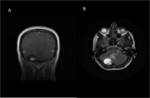
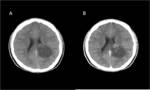
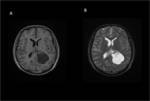
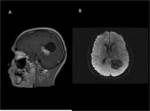
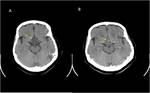
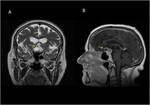
Hemangioblastoma
Most common in the posterior fossa. The nodular portion occasionally demonstrates flow voids visible in T1- and T2- sequences,
while the cyst is slightly hyperintense in T1 images compared with CSF.
In T2 and FLAIR images,
both cyst and nodule are hyperintense.
The enhancement of the wall of the cyst is rarely seen in hemangioblastoma. Fig (3,4).
Pleomorphic xanthoastrocytoma
Supratentorial superficial cortical mass.
Usually in the temporal lobe.
Cystic portion is isointense to CSF.
Enhancement of adjacent meninges,
with an appearance of dural tail.
The mass is round to oval but despite its circumscribed appearance,
the tumor often infiltrates into the brain.
On T1 images,
the nodule appears hypointense or isointense to gray matter while the cystic portion is isointense to CSF.
Sometimes an associated cortical dysplasia may also be seen.
On T2 images,
the pleomorphic xanthoastrocytoma looks hyperintense or may have mixed signal intensity,
and surrounding edema is rare.
On FLAIR images,
the cyst content is normally suppressed.
A peculiar feature is the presence of enhancement of adjacent meninges,
with the appearance of a dural tail (in approximately 70% of cases) as visible in.
The enhancing nodule often abuts the pial surface.Fig (5)
Ganglioglioma
Cortically based mass in a child/young adult with temporal lobe epilepsy.
Calcifications inside the lesion are common. It is a well-circumscribed mass that often expands the cortex.
Calcifications inside the lesion are a common finding.
In T1 images it is hypo-isointense to gray matter; rarely it can be hyperintense for the presence of Ca2þ; and has associated cortical dysplasia.
In T2 images it is typically hyperintense.
Enhancement is usually moderate and heterogeneous.Their appearance on imaging is very variable: from a partially cystic mass with an enhancing mural nodule (~45% of cases) to a solid mass expanding the overlying gyrus.
Contrast enhancement is variable.Fig (6,7,8).
Desmoplastic infantile ganglioglioma
Typical features are the presence of a large cyst with a cortical-based enhancing tumor nodule.
Enhancement of the adjacent pia and the reactive dural thickening are quite specific findings.
It tends to be frontal or parietal.
On T1 images,
the hypointense cyst may contain septae while the nodule is heterogeneous.
On T2 images the cyst is hyperintense and the nodule usually has a low signal.
The solid tumor nodule enhances markedly along with the leptomeninges and dura adjacent to the solid tumor.
Ependymoma
The majority of intracranial ependymomas (60%) are located in the posterior fossa (infratentorial),
usually arising from the floor of the fourth ventricle .
This is especially true in children.
The remainder (40%) are located supratentorially and up to half of these are intraparenchymal.
Posterior fossa ependymomas are apt to extend through the foramina of Luschka and Magendie,
hence the term plastic ependymoma.
This is a characteristic feature and can be seen on both CT and MRI.
Ependymomas are typically heterogeneous masses with areas of necrosis, calcification,
cystic change and haemorrhage frequently seen.
This results in a heterogeneous appearance on all modalities.
Intraparenchymal lesions (usually supratentorial) are usually large and variable in appearance,
ranging from completely solid,
enhancing masses to cysts with a mural nodule,
or more heterogeneous masses.
They are believed to arise from trapping of embryonic rests of ependymal tissue in the developing cerebral parenchym.
CT:coarse calcification is common (50%) ,cystic areas (50%) ,solid component iso to hypodense,heterogeneous enhancement ,variable haemorrhage.
MRI:T1 solid portions of ependymoma typically are isointense to hypointense relative to white matter.
T2 hyperintense to white matter more reliable in differentiating tumour margins than non-contrast T1-weighted images (but less reliable than contrast enhanced T1).
T1 C+ (Gd) enhancement present but heterogeneous enhancement with gadolinium is useful in differentiating tumour from adjacent vasogenic oedema and normal brain parenchyma
DWI/ADC restricted diffusion may be seen in solid components,
especially in anaplastic tumour diffusion should be interpreted with caution in masses with significant haemorrhage or calcification
MRS Choline peak elevation according to the cellularity of tumour,
NAA peak reduction elevated Cho/Cr ratio lipid and lactate rise when degeneration occurs.Fig (9,10).
Cystic meningioma
Meningiomas generally have the characteristic imaging appearance of a wellcircumscribed,
solid,
homogeneously enhancing extra-axial mass on both CT and MRI.
Adjacent osseous changes,
most commonly hyperostosis,
may also be seen.
Th e term “cystic meningioma” has been used to describe meningiomas with intratumoral or peritumoral cysts.
Th e presence of an associated cyst is an uncommon imaging feature that may make it diffi cult to distinguish the tumor from an intra-axial primary glial neoplasm.
The presence of peritumoral edema,
as in the case presented,
can also be a misleading fi nding.
Th e exact cause of cyst formation is not entirely known,
although many mechanisms have been proposed.
Th ese include cystic degeneration of the tumor,
secretion of fl uid from tumor cells,
or loculated cerebrospinal fl uid from scar tissue within or adjacent to the tumor. Fig (11,12).
Metastases
The classical appearance of a metastasis is a solid enhancing mass with well-defined margins and extensive edema.
Occasionally,
central necrosis produces a ring enhancing mass.
Multiple lesions with marked vasogenic edema and mass effect are typically seen in patients with brain metastases.
Lesions are isointense to mildly hypointense on T1-weighted images,
hyperintense on T2-weighted images or with FLAIR.
Surrounding edema is relatively hypointense on FLAIR and T1-weighted images and hyperintense on T2-weighted images.
Following administration of a contrast agent,
solid,
nodular,
or irregular ring patterns of enhancement are seen.
It has been shown that treatment with dexamethasone leads to a reduction in evidence on MRI of peritumoral edema and occasionally,
a lessening in the extent of contrast enhancement.
Definitive diagnosis can be established on biopsy.Fig (13).